In the period from 2005 to 2012,
29 cases with cerebrovascular occlusion were treated.
38 endovascular procedures were performed: 24 targeted thrombolysis and 14 mechanical thrombectomy.
Mechanical thrombectomy was performed using 7 Penumbra sets,
5 Solitaire FR sets and twice using the microcatheter and microguidewire.
The combination therapy (targeted thrombolysis and mechanical thrombectomy) was used 4 times (Table 3).
The 7 times during thrombolysis was used ReoPro (Abciximab),
16 times the rt-PA.
In 7 cases of the vascular spasm papaverine was applied.
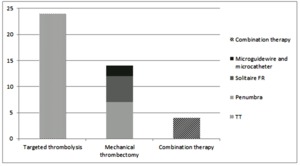
Table 3
References: Student Scientific Society of Interventional Radiology, Medical University of Silesia/ Katowice 2013
Obstruction occurred most frequently in the middle cerebral artery (41,67%),
basilar artery (16,67%),
vertebral artery (11,11%) and internal carotid artery (11,11%).
(Table 4).
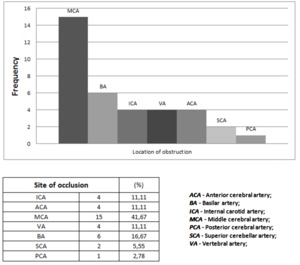
Table 4
References: Student Scientific Society of Interventional Radiology, Medical University of Silesia/ Katowice 2013
We evaluated 29 patients with cerebrovascular obstruction who underwent invasive treatment.
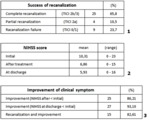
Neurological status of patients before treatment,
assessed using the NIHSS scale,
ranged from 0 to 23 (mean 10.31,
SD ± 5.27).
The status of patients after treatment,
according to the NIHSS scale,
ranged from 0 to 15 with an average of 6.86 (SD ± 4.57).
However,
on the day of discharge from the hospital,
the status of patients,
was in the range of 0 to 16 with an average of 5.93 (SD ± 4.85) (Table 5.2).
The mean time from symptom onset to recanalization was 390 minutes (with a range of 201 - 538 minutes).
The mean duration time of the procedure was 98 minutes (with a range of 40 - 250 minutes) and 53 minutes for efficient procedures.
86.21% of all patients had improved neurological status (assessed using the NIHSS scale) after treatment and the status level was maintained increased to 93,10% the day of discharge.
76,32% of all procedures performed resulted in successful recanalization (TICI 2a,
TICI 2b/3) (Table 5.1),
thus succeeding to obtain blood flow through brain vessels in 79.31% of patients.
Among these,
clinical improvement in NIHSS was 82.61%.
(Table 5.3).
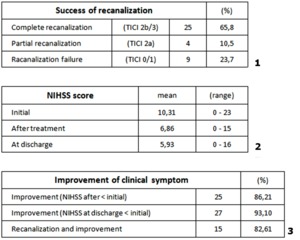
Table 5
References: Student Scientific Society of Interventional Radiology, Medical University of Silesia/ Katowice 2013
Mechanical thrombectomy treatment performed using the Penumbra system ended in the clearing of 42.86% of obstructed vessels,
the use of the Solitaire FR set was successful in 100%.
The overall efficiency of mechanical thrombectomy (Penumbra + Solitaire FR + microcatheter and microguidewire) was 71.43%.
The efficiency of targeted thrombolysis was 79.17% (Table 6).
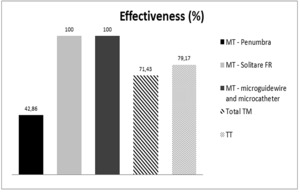
Table 6
References: Student Scientific Society of Interventional Radiology, Medical University of Silesia/ Katowice 2013









