Tuberculosis (TB) has always been a major public health problem in developing countries.
The incidence had decreased with the introduction of antituberculous drugs but resurgence has been seen due to drug resistance.
Prevalence has increased in developed countries due to large population suffering from chronic diseases (e.g.,
diabetes mellitus,
chronic renal failure,
chronic obstructive disease,
liver cirrhosis,
lymphoproliferative disorders,
etc.),
a growing number of immunocompromised patients; the emergence of multidrug-resistant TB; and various socioeconomic factors (e.g.,
alcohol and drug abuse,
poverty,
homelessness,
etc.).
High prevalence is seen among patients with AIDS who often present with it as first manifestation of HIV infection.1
In 20% of patients with TB extrapulmonary manifestations occur.
Musculoskeletal TB accounts for 1-3% of tuberculous infections.
The most common form being tuberculous spondylitis (50%).
Extraspinal manifestations are uncommon.
Frequency of peripheral arthritis is around 60%,
of osteomyelitis 38%,
and of tenosynovitis and bursitis 2%.
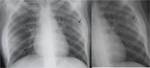
Coexistent active pulmonary TB is seen only in 50% of the patients.2
Patients with musculoskeletal TB present with nonspecific,
subtle symptoms due to which diagnosis may be delayed.
However,
if prompt diagnosis is made an early treatment can prevent joint deformity and permanent bone destruction. Clinical and imaging findings alone cannot diagnose musculoskeletal TB but correlation with rest of diagnostic workup can help in an earlier diagnosis and prompt institution of treatment.
It is essential to identify the common and uncommon radiologic findings so that an accurate and early diagnosis can be made to prevent complications.
ETIOPATHOGENESIS:
Main causative organism is Mycobacterium tuberculosis,
only a few cases are caused by Mycobacterium bovis.
1-4% of cases are caused by atypical mycobacteria like Mycobacterium kansasii,
Mycobacterium marinum, Mycobacterium scrofulaceum,
and Mycobacterium avium complex .
Dissemination of mycobacteria to musculoskeleton occurs mostly by haematogenous route.
Direct inoculation of the organism into the site occurs rarely.
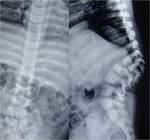
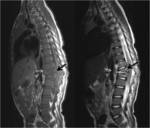
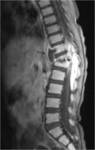
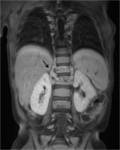
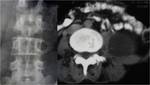
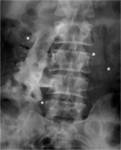
TUBERCULOUS SPONDYLITIS:
Also known as Pott disease.
Thoracolumbar junction is most frequently involved.
Usually infection spreads hematogenously by perivertebral arterial plexus or venous plexus of Batson,
or rarely by contiguous spread from a paraspinal infection.
Clinical manifestations include persistent spinal pain,
tenderness,
limitation of mobility and constitutional symptoms3.
The superior or inferior anterior vertebral body corner in the paradiscal location are involved first.
Further spread of infection can occur by subligamentous route or through the subchondral plate.
Disc involvement occurs late with narrowing due to herniation of the disc into the collapsed vertebral body.
Gibbus deformity can occur due to collapse of multiple vertebrae with anterior wedging.
TYPES OF TUBERCULOUS INVOLVEMENT OF THE SPINE:
Paradiscal or the marginal type: It is the most common type.
Infection starts at the end plates with subsequent involvement of the vertebral body.
Anterior subperiosteal : Infection starts beneath the periosteum at the anterior vertebral margin and spreads underneath the anterior longitudinal ligament.
Central: It is seen as a lytic area in the center of the vertebral body.
Initially expansion occurs followed by a concentric collapse resembling vertebra plana.
Appendiceal or neural arch tuberculosis (NAT): There is involvement of posterior elements.
Its a rare type of tubercular spine (<2% ).
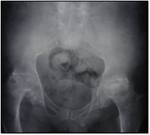
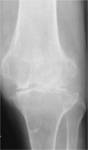
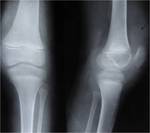
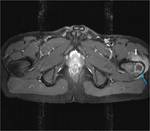
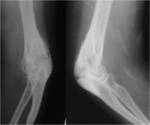
TUBERCULOUS ARTHRITIS:
Infection can spread to the joints by contiguous spread (from adjacent metaphyseal lesion) or hematogenously.
Monoarticular joint involvement is more common,
multifocal disease is seen in approximately 10% of patients4.
Due to the Synovial hypertrophy pressure necrosis occurs causing peripheral and central erosions.
Subchondral bone and articular cartilage destruction occurs however joint space narrowing is a late complication.
Paraarticular soft tissue masses,
cold abscesses and sinus tracts may also develop.
Demineralization and local bone destruction can occur due to reactive hyperemia.
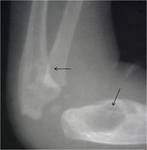
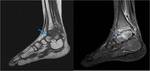
TUBERCULOUS OSTEOMYELITIS:
Monoostotic involvement with the bones of extremities including small bones of hands and feet more commonly involved.
Infection spreads from an active focus by haematogenous route5.
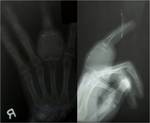
In tubercular dactylitis short tubular bones of the hands and feet are more commonly involved.
Presentation is subtle without fever and acute inflammatory signs unlike acute osteomyelitis.
The involved bone has a ballooned out appearance with an internal cyst like cavity.
Soft tissue swelling with periosteal thickening and bone destruction occurs.
Presentation is subtle without fever and acute inflammatory signs unlike acute osteomyelitis.
Multifocal tuberculous osteomyelitis (osteitis cystica tuberculosa multiplex),
is a rare pattern of TB osteomyelitis which is more common in children.
Commonly the metaphyses of long bones are affected.
TUBERCULOUS TENOSYNOVITIS AND BURSITIS:
This may result from hematogenous spread or there maybe periarticular extension of tuberculous arthritis.
Thickening and infiltration of tendon or synovium can occur,
in the later stage of the disease thinning of the tendon and tendon rupture may occur1.
Secondary involvement of synovium of bursae is more common than primary bursitis.
TUBERCULOUS MYOSITIS:
Muscle and deep fascia is rarely seen in musculoskeltal TB.It is mostly seen in immunosuppressed patients.
Chest wall involvement occurs more commonly in parasternal region,
costovertebral junction,
and along the shafts of the ribs.