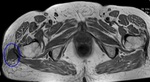
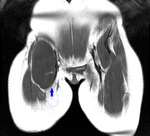
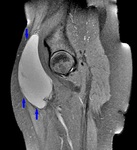
ARTICULAR CAUSES OF HIP PAIN
A. FEMOROACETABULAR IMPINGEMENT (FAI)
FAI is clinically characterized by a history of painful internal rotation and a positive impingement test.
During this test,
groin pain is provoked by a combined maneuver of 90° flexion,
adduction,
and internal rotation of the hip.
FAI refers to a conflict between the proximal femur and the acetabular rim and is a reason for premature osteoarthritis of the hip.
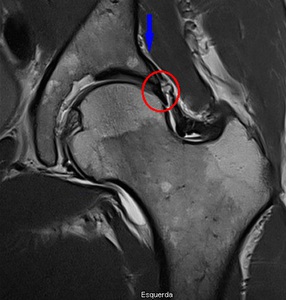
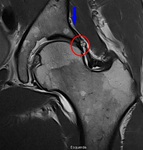
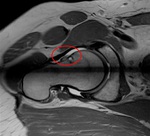
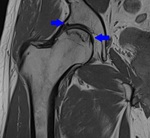
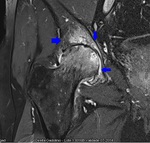
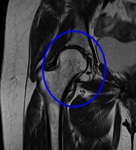
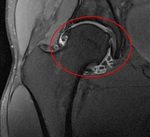
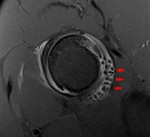
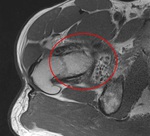
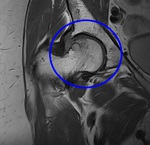
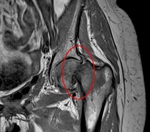
Fig. 8: Coronal PD WI of the left hip (arthro-MRI). Increased acetabular coverage (blue arrowhead) and hypertrophic labrum (red circle).
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
There are two different types of FAI (as well as the combined impingement type):
- CAM
In CAM FAI an aspherical shape of the femoral head and a reduced depth of the femoral waist (offset) leads to an abutment of the femoral head-neck junction against the acetabular rim (Fig. 5 and Fig. 6).
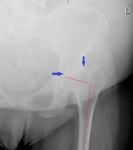
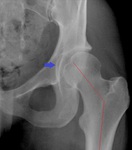
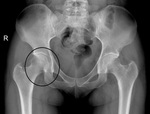
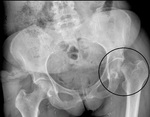
In CAM FAI the anteroposterior standard radiograph of the hip may demonstrate a so-called pistol-grip configuration with a flattened lateral femoral head-neck junction.
In addition synovial herniation,
changes of the acetabulum,
such as an os acetabuli,
and ossification of the acetabular rim may be seen ( Fig. 9 ).
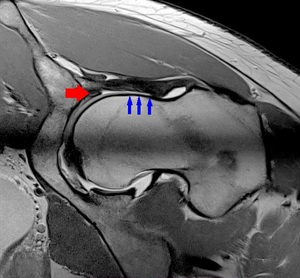
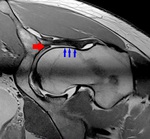
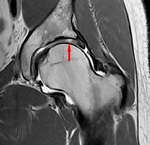
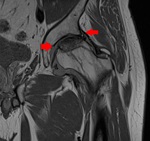
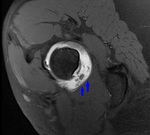
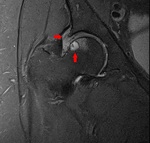
Fig. 6: Radial PD WI of the left hip (arthro-MR). Increased alpha angle, labral degeneration (red arrowhead) and CAM-deformity (blue arrowhead).
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
2.
PINCER
In PINCER impingement acetabular overcoverage leads to a conflict between the acetabulum and the femur ( Fig. 7 and Fig. 8 ).
Labral tears and cartilage lesions nearby to the abnormal labrum are commonly found in these joints ( Fig. 10 ).
.
B. LABRAL TEARS
Labral lesions are a common cause of hip pain ( Fig. 11 and Fig. 12).
In about half of these patients acetabular and femoral osseous abnormalities are found on standard radiographs,
including:
- a decreased head-neck waist,
- an aspherical femoral head,
- hip dysplasia,
- retroverted acetabulum,
or
- osteoarthritis.
Most labral abnormalities are thought to be part of a continuum of morphological changes associated with hip deformities,
resulting in labral tears,
delamination of the adjacent cartilage,
and,
finally ,
early osteoarthritis.
The most relevant etiologies of such changes are developmental dysplasia and femoroacetabular impingement .
MR arthrography is the modality of choice to assess the acetabular labrum with a sensitivity and accuracy of about 90-95% according to different series.
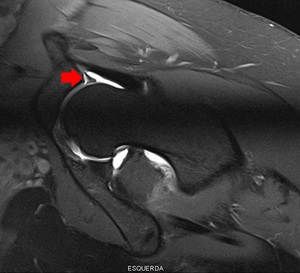
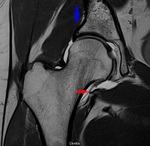
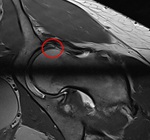
Fig. 12: Radial PD Fat-Sat WI of the left hip (arthro-MRI). Rupture of the labral base.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
C. DYSPLASIA AND DEVELOPMENTAL ABNORMALITIES
- DYSPLASIA
Hip dysplasia can range from barely detectable to severely malformed /dislocated hips.
The condition can be bilateral or unilateral .
In acetabular dysplasia the acetabulum is too shallow or deformed.
The center-edge angle is measured as described by Wiberg and is a reliable indicator of dysplasia.
If the joint is fully dislocated a false acetabulum often forms (often higher up on the pelvis).
There is evidence that patients with hip dysplasia are prone to develop osteoarthritis at an early age.
2.
DEVELOPMENTAL ABNORMALITIES
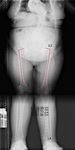
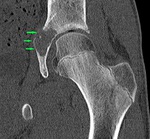
a) In coxa vara the femoral head grows at too narrow an angle to the shaft (Fig. 13 and Fig. 14 );
b) In coxa valga the angle is too wide ( Fig. 15 and Fig. 16);
c) Achondroplasia,
common cause of dwarfism ( Fig. 13 and Fig. 14);
d) Others.
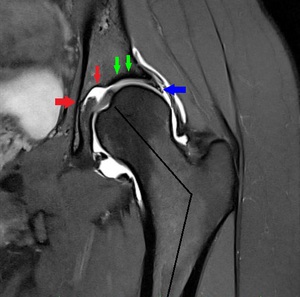
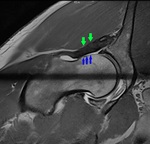
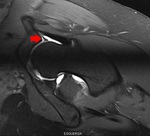
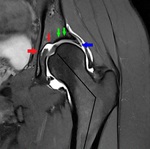
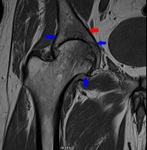
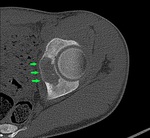
Fig. 15: Coronal PD Fat-Sat WI of the left hip (arthro-MRI). Acetabular dysplasia (green arrowhead) with fovea Alta (red arrowhead), coxa valga (angle black lines) and hypertrophic labrum(blue arrowhead).
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
D. OSTEOARTHRITIS
Radiographically,
joint space narrowing due to cartilage damage is seen,
typically in the superior,
load-bearing area. Less frequently,
medial loss of joint space is seen,
which may be associated with mild acetabular protrusion ( Fig. 17).
Femoral and acetabular osteophytes,
subchondral sclerosis,
and subchondral cysts are typically present on standard radiographs (Fig. 18 and Fig. 19).
MR images also demonstrate degeneration,
tears,
and detachment of the labrum as well as subchondral edema-like bone marrow changes.
Thickening or buttressing of the medial femoral cortex may be apparent.
In advanced osteoarthritis,
standard radiographs are sufficient for the diagnosis and for surgical decision making.
Additional imaging may be used in suspected early osteoarthritis with normal or nearly normal radiographs and for differential diagnostic purposes (for instance,
for exclusion of avascular necrosis and radiographically occult stress fracture).
.
E. AVASCULAR NECROSIS OF FEMORAL HEAD (AVN)
MR imaging is the imaging modality of choice in suspected AVN of the femoral head ( Fig. 20 and Fig. 21 and Fig. 22).
AVN occurs typically between the third and sixth decades of age and is more common in men than in women.
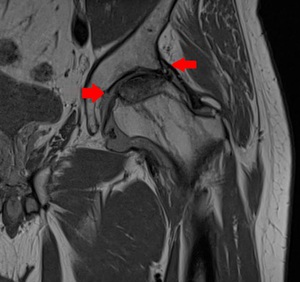
Fig. 22: Coronal PD WI left hip. Irregularity of the femoral epiphyseal region with serpiginous appearance.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
Commonly,
no etiology can be determined.
Main causes include:
1.
Trauma with fracture of the femoral head or neck or hip dislocation are typical causes for AVN.
2.
Nontraumatic etiologies :
- corticosteroid use,
- alcohol abuse,
- sickle cell anemia,
- lupus erythematosus,
- coagulopathies,
- hyperlipidemia and
- Gaucher's disease.
In contrast to standard radiography or CT,
MR imaging is capable of detecting early stages of AVN with the possibility of early joint-sparing therapy such as core decompression.
Typically,
on T1-weighted images a serpiginous line of low signal surrounding an area of fatty marrow is seen in the anterosuperior femoral head.
On T2-weighted images,
a characteristic double line sign has been described: parallel to the hypointense serpiginous line a hyperintense inner line is visible,
representing granulation tissue at the interface of necrotic and viable bone.
Due to the frequent bilateral occurrence of AVN the contralateral hip must be evaluated.
On standard radiographs,
the existence of a crescente and collapse of the femoral head have been used as predictors for the outcome.
With MR imaging,
the assessment has become more precise.
The extent of involved bone measured in relation to the weight-bearing surface is relevant for the clinical outcome.
The percentage of involved weight-bearing femoral area in relationship to the acetabular roof appears to be the most accurate parameter.
Clinical outcome is consistently poor for osteonecrosis involving more than 45% of the weight-bearing surface.
.
F. INFLAMMATORY CONDITIONS
- Septic arthritis
- Traditionally it is a clinical diagnosis,
but findings are not specific: Warm,
swollen joint,
decreased range of motion with or without fever/chills
- Monoarticular in 90% of patients
- Blood cultures positive in 50% of patients
- Demographics: Septic hip in children generally under 3 yo and there is an increase in incidence in teenagers.
Elderly are also at risk due to prevalence of arthroplasties & chronic diseases
- Natural History & Prognosis With appropriate treatment: 60% recover completely.
Remainder have permanent damage to joint,
resulting in deformity or mechanical arthritis.
- Treatment: Antibiotics appropriate to infecting organism and Drainage;
- MR imaging sensitive (100%) & more specific (77%) than other imaging and is often abnormal within 24 hours of onset
- Fluid-sensitive sequences: Hyperintense effusion,
hyperintense subchondral bone,
perisynovial soft tissue enhancement
- Post-contrast T1 fat-saturated imaging: Synovial thickening surrounding effusion,
subchondral bone enhancement,
occasional adjacent soft tissue abscess
- Frequency of findings: Synovial enhancement (98%); Marrow bare area changes (86%); Abnormal T2 marrow signal (84%) & abnormal enhancement (81%); Abnormal T1 marrow signal (66%); Perisynovial edema (84%); Joint effusion (70%) (almost 1/3 lack effusion; joints of hand or foot predominate)
2. Rheumatoid arthritis (RA)
- In RA inflammation and proliferation of the synovial membrane with or without bone erosion as well as intra-articular fluid collections are typically found ( Fig. 23 and Fig. 24).
- It affects all synovial structures,
including tendon sheaths and bursae.
Due to the commonly bilateral involvement of the hip joints in RA at least one fluid-sensitive sequence of the entire pelvis should be included in the MR imaging protocol.
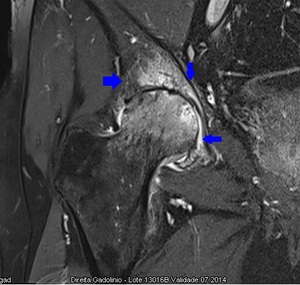
Fig. 24: Coronal T1 FS WI GAD of the right hip. Marked enhancement of both articular surfaces associated with synovitis, protrusion and tiny erosions.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
Typically findings on MR images are:
- synovial thickening (with low signal on T1-weighted images and high signal on T2-weighted or STIR sequences) and effusion
- In active disease this pannus enhances strongly after intrave- nous injection of contrast.
In chronic disease,
pannus may become fibrotic.
- there may be deposits of hemosiderin,
influencing MR signal characteristics (hypo- intense signal on all sequences).
- Detachment of fibrotic parts of the pannus from the synovial membrane leads to so-called rice bodies (diameter of few millimeters).
- Pannus may erode bone which most typically occurs at the central portion of the femoral head and acetabulum.
- Diffuse cartilage loss leads to superomedial migration of the femoral head,
contrary to the typical superolateral migration found in cartilage damage asso-ciated with osteoarthritis.
- There may be a subchondral edema-like signal pattern and subchondral cysts may be found.
3. Seronegative Spondylarthropathies
Two main considerations in this group:
A. Psoriatic Arthritis ( Fig. 25 and Fig. 26)
Inflammatory arthritis,
usually developing after or coincident with skin changes of psoriasis.
Arthritis precedes skin changes by 2 years in 15%.
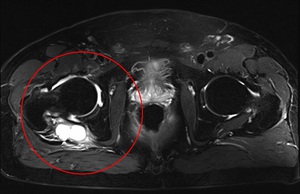
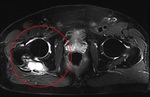
Fig. 25: Axial T2 Fat-Sat WI of the pelvis. Psoriatic arthritis with huge peri-articular cysts of the right hip.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
Imaging Diagnosis most frequently made on radiographs
- Peripheral arthropathy Interphalangeal (IP) joints predominate with soft tissue swelling
- Productive arthropathy,
with enthesopathy and periostitis
- Ankylosis is common feature
- Normal bone density
- Bilaterality and symmetry less frequent than in rheumatoid arthritis
- Sacroiliitis: 35% of patients usually begins asymmetrically but bilaterally.
At any time in the course of the disease may appear symmetric.
- Spondylitis: 30% of patients have bulky paravertebral ossifications more prominently seen on AP than lateral view (asymmetric with skipped levels)
In early disease,
MR shows abnormalities,
though usually nonspecific: Edema,
synovitis in peripheral joints.
Marrow edema at SI joints.
Enthesopathy,
periostitis,
Marrow enhancement are also common features.
B. Ankylosing Spondilitis
.
4. Chemical Synovitis
Following some arthrographic procedures chemical synovial reaction may occur (reported with a frequency of less than 1 to 500).
Although it is infrequent it is always necessary to exclude septic athritis (Fig. 27 and Fig. 28).
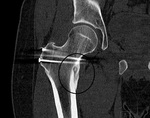
5. Osteomyelitis (Fig. 3 and Fig. 29 and Fig. 30)
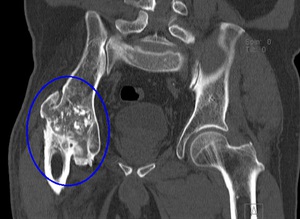
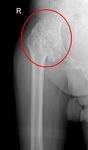
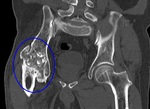
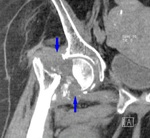
Fig. 30: CT of the right hip (coronal reformat). Osteomyelitis. Huge dense lesion with articular destruction.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
G. DEPOSITION DISEASE and SYNOVIAL ABNORMALITIES
1. Chondromatosis
Synovial osteochondromatosis can be divided into:
a) Primary Form ( Fig. 31 and Fig. 32 and Fig. 33)
b) Secondary Form occurs in association with (Fig. 34 and Fig. 35):
- trauma,
- osteoarthritis,
- osteonecrosis,
- neuropathic arthropathy.
In secondary osteochondromatosis,
the intra-articular bodies tend to be:
- larger,
- less numerous,
- more varied in size than in the primary form,
- Typically associated with more pronounced degenerative disease of the joint.
On radiographs ossified or calcified juxta-articular bodies are present in about 80% of the involved joints.
In half of the patients bone erosions and osteophytes are found,
and in one-third of the patients joint space narrowing is present.
MR imaging demonstrates:
- synovial thickening (87%),
- bone erosions,
- intra-articular bodies (73%),
- synovial herniation (40%).
Signal characteristics of unmineralized bodies are similar to hyaline cartilage.
Ossified bodies may either be hypointense (in the presence of dense bone) or be hyperintense on T1-weighted images due to the presence of fatty bone marrow.
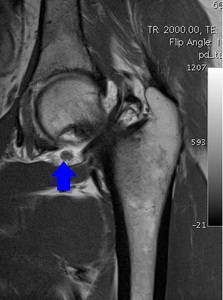
Fig. 34: Coronal PD WI of the left hip (arthro-MRI). Synovitis with some intra-articular bodies of different sizes.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
2. Pigmented Villonodular Synovitis (PVNS)
Pigmented villonodular synovitis ( Fig. 37 and Fig. 38) is a benign proliferative disorder of the synovial membrane.
-
Usually seen in young adults,
with a peak presentation in the third and fourth decades of life.
-
The hip joint is the second most commonly involved location after the knee (80% of cases).
-
Patients typically present with swelling,
stiffness,
and progressive pain in the involved joint.
Tends to locally destruct the joint.
- Malignant transformation has been reported,
although this is extremely rare and controversial
- On standard radiographs advanced PVNS presents with multiple juxta-articular erosions,
osteoarthritis,
and arthritis-like changes.
- MR imaging is the modality of choice for the assessment of PVNS.
Typically,
synovial-based nodules or masses with hypointense signal on both T1- and T2-weighted images are found.
There may be a blooming artifact on gradient echo sequences due to the commonly present hemosiderin.
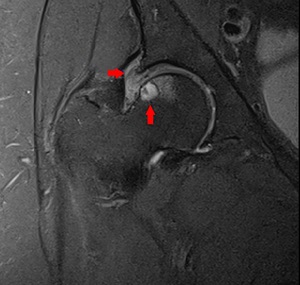
Fig. 37: Coronal DP Fat-Sat WI of the right hip. Synovitis and focal single erosion of the femoral head.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
H. TUMORS
As this presentation does not intend to demonstrate the full range and depth of tumoral pathologies we only give some examples of some tumors found during the time period reviewed.
1.
Primary Bone Tumors
2 Metastasis (Fig. 44 and Fig. 45 and Fig. 46 and Fig. 47)
3.
Myeloma/Lymphoma
4.
Soft Tissue Tumors ( Fig. 48 and Fig. 49 and Fig. 50)
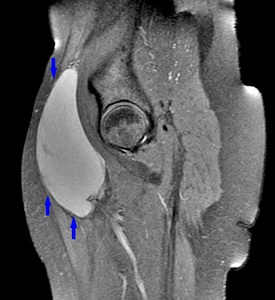
Fig. 50: Sagital PD Fat-Sat WI of the pelvis. Mass in the right inguinal area with high signal in T2 WI and focal adipose septa.
References: Hospital da Luz - MSK Imaging Unit - Lisbon/PT
Common tumors of the proximal femur are osteoid osteoma,
osteoblastoma,
chondroblastoma,
chondrosarcoma,
multiple myeloma,
and metastasis;
In general, standard radiographs remain the most important image modality in the diagnosis of bone tumors and MR imaging is used to determine the extent of the tumor;
CT is most useful in the assessment of bones in anatomically complex regions including the hip;
CT may demonstrate cortical destruction and periosteal reaction.
It may also demonstrate subtle matrix calcification not seen on standard radiographs,
especially of the pelvis with its complex anatomy;
The role of MR imaging is to evaluate the intramedullary and soft tissue extent of bone neoplasm,
such as metastasis,
myeloma,
lymphoma,
or giant cell tumor; In some types of tumors,
characterization of the lesion is possible.
In osteoid osteoma a small nidus surrounded by an edema-like signal is typically found and often CT is used to confirm the diagnosis;
On MR imaging well-differentiated cartilaginous tumors may have a nodular appearance with high signal intensity on fluid-sensitive images and low signal foci representing calcification.