Tuberculosis (TB) is an infection that is transmitted by air,
caused by mycobacteria,
Mycobacterium tuberculosis.
It is the most common cause of death from infectious diseases worldwide.
According to WHO,
2 million people die of TB every year and 6 million develop active disease.
In fact,
1/3 of the world population is considered carrier of TB (latent disease).
The incidence of this disease has resurfaced in non-endemic countries,
mainly due to immigration,
the HIV epidemic and resistance to antituberculosis drugs.
Various organs can be affected by infection,
though the most common is lung involvement.
We find manifestations in the central nervous system (meningitis),
musculoskeletal system,
genitourinary system,
gastrointestinal (GI) tract,
heart (pericarditis,
myocardial),
lymphatic system (lymph nodes),
and so on.
Extrapulmonary dissemination is more frequently found in immunosuppressed population.
Radiological findings in abdominal tuberculosis:
It is the most common extrapulmonary affection.
The solid viscera is more often affected than the gastrointestinal tract.
In the present review we will address the imaging findings on the following systems:
- Genitourinary.
- Lymphatic system.
- Peritoneum.
- Gastrointestinal tract.
- Hepatosplenic.
- Adrenal glands.
1.
- GENITOURINARY SYSTEM
It is the most common manifestation of extrapulmonary TB (20%).
It can occur by either hematogenous spread (to kidneys,
prostate,
seminal vesicles) and by contiguity (bladder,
epididymis).
The most common symptoms it produces are frequency and dysuria.
Urine culture may be normal.
Within the genitourinary system,
we will address the involvement of the kidney,
ureter,
bladder and genitals both male and female.
- Kidney:
The infection triggers the formation of small cortical granulomas.
In patients with intact cell immunity bacterial replication inhibition is found,
which can confine the disease development for many years,
until there is a decrease in immunity.
In 75% of cases the involvement is unilateral.
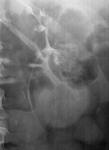
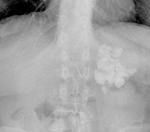
- Intravenous urography can demonstrate filling defects in the collecting systems for caseous detritus formation.
It is the earliest finding.
Papillary necrosis produces calyces of moth-eaten look,
with appearance of annular calcification in the collecting system ( Fig. 1 ).
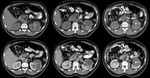
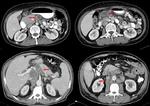
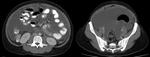
- In computed tomography (CT) scan,
the most common finding is renal calcification (50%) ( Fig. 2 and Fig. 3 ).
In later stages parenchymal cavitation may occur,
which communicates with the excretory system.
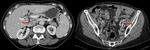
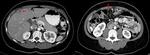
In study with intravenous contrast,
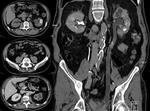
the contrast can form collections ( Fig. 3 and Fig. 4 ).
Stenosis of calyceal infundibula may appear directly or by folding of the pelvis,
causing incomplete opacification of the calyce,
hydronephrosis with filling defects,
scarring and cortical thinning ( Fig. 3 ).
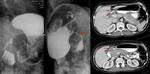
In a final stage,
large calcifications with lobar distribution (autonephrectomy) and mastic kidney (nonfunctional) ( Fig. 5 ) appear.
In short,
a temporal sequence can be defined: granuloma -> papillary necrosis -> parenchymal cavitation -> scarring and calcification -> dysfunction.
Differential diagnosis includes chronic pyelonephritis,
xanthogranulomatous pyelonephritis,
papillary necrosis,
sponge kidney,
calyceal diverticulum,
renal cell carcinoma and urothelial carcinoma.
- Ureter:
The ureter is affected in nearly 50% of patients with renal TBC,
especially in the distal third,
with preference for narrow anatomical areas.
The infection causes wall thickening,
mural enhancement and stenosis,
with a sawtooth-like appearance of the ureter.
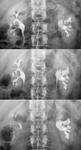
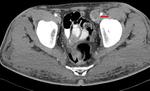
If there is progression,
a corkscrew-shaped ureter is identified,
as well as alternating stenosis,
shortening,
filling defects and/or wall calcification ( Fig. 3 and Fig. 4 ).
Differential diagnosis includes lithiasis,
cystic ureteritis,
calcifications from schistosomiasis,
multiple urothelial carcinoma.
- Bladder:
The main consequence of its affectation is decreased filling capacity.
In an image study we can see wall thickening,
ulcers and filling defects.
In advanced disease we will see it deformed,
reduced in size,
with scars and calcifications (less frequent than in the kidney).
Ureteral orifice stiffness may produce reflux.
Differential diagnosis includes schistosomiasis,
sequelae after treatment with cyclophosphamide or other drugs,
effects of radiotherapy and bladder carcinoma with calcifications.
- Genital:
- Female: The most common location is tubal (90%).
May cause bilateral salpingitis,
adhesions and sometimes deformity of the endometrial cavity.
A tuboovarian abscess passing through the peritoneum to the extraperitoneal compartment is suggestive of tuberculous infection.
- Male: The most common locations are seminal vesicles and prostate.
We find prostate calcifications in 10% of cases.
- In a CT scan low-attenuation foci may occur secondary to caseous necrosis and inflammation.
- Magnetic resonance imaging(MRI) can show stellate hypointense areas on T2-weighted sequences.
The testes and epididymides involvement is rarer,
with nonspecific findings in the image.
Differential diagnosis includes pyogenic abscesses,
nontuberculous.
2.
- LYMPHATIC SYSTEM
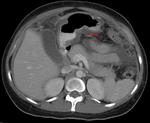
Lymph nodes are the most common finding (55-65%) in TB infection.
The most frequently affected groups are the peripancreatic and mesenteric ( Fig. 6 ).
50% of the lymph nodes are enlarged on CT,
with a hypodense center and peripheral rim enhancement.
Other imaging patterns are conglomerate masses of lymph nodes with mixed or homogeneous attenuation ( Fig. 7 and Fig. 8 ).
Given the multiple etiologies that cause enlarged lymph nodes in the abdomen,
the differential diagnosis is broad,
including metastasis,
lymphoma,
Whipple's disease or infection by other mycobacteria.
3.
- PERITONEUM
It is a rare affection,
difficult to assess for having nonspecific imaging findings.
Usually primary (hematogenous spread),
but may be secondary to rupture of a lymph node,
to gastrointestinal involvement or to tubal affection.
Peritonitis is classified into three main types,
although they may overlap:
- Wet: 90%.
Imaging studies demonstrate an important ascites,
either free or loculated.
In the CT scan it appears as a slightly hyperdense liquid (20-45 hounsfield units) due to its high protein and cell content ( Fig. 9 ).
- Fibrotic: 60%.
Appears as "Omental cake",
with formation of low-attenuation mesenteric and omental masses as well as small soft tissue nodules ( Fig. 10 ).
This type may cause stenosis of bowel loops.
- Dry: 10%.
Presents along with fibrous adhesions.
Thickening of the mesentery,
omentum and small peritoneal nodules that enhance with contrast.
Differential diagnosis includes peritoneal carcinomatosis,
nontuberculous peritonitis,
mesothelioma.
4.
- GASTROINTESTINAL TRACT
It is a rare affection.
It focuses primarily on the ileocecal region (90%),
followed by the jejunum,
because of the larger amount of lymphoid tissue in these locations.
It consists mainly of mural thickening,
typically concentric.
Retraction of the caecum or ileal stenosis can also appear.
If there is obstruction,
this may be due to stenosis in the wall or to extrinsic compression by lymph nodes.
- In a barium study,
the earliest manifestation is edematous ileocecal valve with spasm and hypermotility.
We describe several signs:
- Fleischner sign: narrowed terminal ileum with valve wide open.
- Stierlin sign: narrow terminal ileum with rapid emptying to rigid and shortened caecum.
- In double contrast study: linear or stellate superficial ulcers can be observed,
with elevated margins.
Canker sores also appear in the early stages of the disease,
in the same orientation than the lymphoid follicles (ie,
longitudinal in terminal ileum and transverse in the colon).
Advanced TB may appear as a stenosis "in napkin-ring" with a conical caecum,
pulled out of the right iliac fossa (RIF) by mesocolon retraction.
Over time we identify a rigid and incompetent valve.
In other proximal segments of the GI tract,
the less frequent involvement is attributed to the bactericidal property of gastric acid and the paucity of lymphoid tissue.
- Esophagus: usually manifests as extrinsic compression by lymph nodes.
- Stomach: simulates a peptic ulcer in the antrum ( Fig. 11 and Fig. 12 ).
- Proximal intestine: mucosal fold thickening,
nonspecific.
The clinical presentation is also nonspecific,
with vomiting,
abdominal pain or weight loss.
Should be suspected in patients with risk factors,
non-responders to anti-ulcer therapy and youth.
Differential diagnosis includes terminal ileitis,
Crohn's disease,
neoplasm,
lymphoma,
giardiasis,
amoebiasis and yersinia infection.
5.
- HEPATOSPLENIC
It can be seen in patients with disseminated disease.
There are two patterns of presentation:
- Micronodular / miliary: Multiple foci that may not be seen on CT scan,
hypodense,
from 0.5 to 2 mm.
On ultrasound parenchyma is hyperechoic.
It is usually associated with pulmonary miliary tuberculosis.
- Macronodular / tuberculoma: Uncommon.
On CT scan appears as hypodense lesions of 1-3 cm,
ill-defined margins,
with peripheral enhancement.
Organomegaly may associate ( Fig. 13 ).
In MRI tuberculomas are hypointense on T1-weighted images,
hyperintense on T2-weighted and with peripheral contrast enhancement.
Calcification of tuberculoma will lead to calcified granuloma.
Differential diagnosis includes:
- Micronodular: multiple metastases,
fungal abscesses,
sarcoidosis and lymphoma.
- Macronodular: metastases,
primary tumor and pyogenic abscess.
6.
- ADRENAL GLANDS
Adrenal glands are also rarely affected.
It is found in 6% of patients with active TB.
According to an autopsy study,
adrenal glands were the 5th extrapulmonar TB affected organ after kidney,
liver,
spleen and bone.
It may occur either unilateral,
bilateral or asymmetric,
producing glandular atrophy in advanced disease,
which can result in appearance of symptoms of Addison’s disease.
In the CT scan we can find enlarged glands,
with hypodense areas of necrosis and/or calcifications ( Fig. 14 ).
Differential diagnosis includes metastasis,
haemorrhage and primary adrenal neoplasm.