Data were mainly extracted from the most actual and representative articles as the research basis,
and recommendations of practice guidelines of official organizations of radiology and nephrology (ESUR,
ACR,
NKF).
GENERAL PREVENTION MEASURES:
Alternative diagnostic techniques that do not utilize iodine contrast media must be considered in high risk patients.
Other measures include limiting contribuitory risk factors (like hypovolaemia,
NSAIDs and certain antibiotics) and limit both the total dose and the number of doses administered in a 48 - 72 hour period.
Different autors have tried to establish the optimal dose,
and determinate that it should be less than or equal to 100 ml when the TFGe is less than 60,
and 5 mlkg of maximum weight when the creatinine exceeds 1.8 mldl; although even a volume less than 30 ml may cause NCI in high-risk patients.
CONTRASTS
Many trials have evaluated the relative effectiveness of non-ionic,
low osmolarity agent related to ionic hyperosmolar agent,
showing reduced risk of NCI with the use of the low osmolal,
but in patients with preserved renal function,
the difference is not so relevant.
Ioxaglato,
an ionic low osmolal,
agent is also associated with low risk of nephropathy by contrast compared to the ionic hyperosmolar agents.
There was no significant difference between Ionic,
low osmolal agent,
and isoosmolal in patients with normal renal function,
but in high-risk population data are heterogeneous,
the greater part of the trials not found differences between these two type of agents in terms of incidence of NCI (CARE,
IMPACT,
PREDICT),
in others this pathology is less frequent in patients who has been administered isoosmolal agents (NEPHRIC,
RECOVER) or hipoosmolal agents(ACTIVE).
This heterogeneity in the results of different studies is due to differences in standardization of the monitoring of creatinine values,
different proportion of patients with risk factors,
chronic renal insufficiency and diabetes,
variety of clinical situations (coronary angiography CT),
different protocols of prophylaxis,
volumes and doses of contrast.
Gadolinium was proposed as an alternative contrast agent in angiographic procedures but the dose needed to avoid nephrotoxic injury (< 0.3mmol) not allowed to obtain satisfactory images.
Non-ionic low osmolarity agents are the most used in the most radiological,
as a result of the reduction of costs,
the patient tolerability,
decrease of hypersensitivity reactions and less incidence of NCI in high risk patients.
SPECIFIC STRATEGIES
The hydration has proven to be the only major preventive action against CIN.
It would appear that intravenous hydration is superior to oral hydration.
The optimal fluid choice,
infusion rate and volume are unclear.
Different patterns of intravenous hydration (table)
Before selecting the solution (isotonic normal N-saline; ½ N-saline,
and isotonic sodium bicarbonate) and the rate of administration it must be taken into account the peri-operative hydration policies of each centre,
the patient’s ability to tolerate a fluid load and alkalinisation; and the degree of risk for nephropathy.
None of the pharmacological measures (renalvasodilators,
receptors antagonists of endogenous vasoactive mediators or cytoprotective drugs) have shown consistent protection against the NCI.
The use of acetylcysteineis based on its potential vasodilator capacity and reduce oxygen-free radical generation and although the results from clinical trials have been inconsistent (fig table),
the trend is suggestive of benefit and it is well tolerated and relatively inexpensive,
so it is usually administrated to high risk patients.
The preferred dose is 1200 mg administered orally twice daily on the day before and the day of the procedure to patients at risk for CIN. It must not be administred intravenous because of potential risk of anaphylactoid reactions.
All gadolinium and iodinated contrast media may be removed by hemodialysis or peritoneal dialysis,
however there is no evidence that hemodinalisis protects patients with impaired renal function from NCI or Nephrogenic Systemic Fibrosis.
So correlation of time of the contrast medium injection with the hemodialysis session and extra hemodialysis session to remove contrast medium is unnecessary.
METFORMIN AND CONTRAST NEPHROPATHY
Metformin does not cause kidney failure per se,
but in the case of pre-existing or iodinated contrast-induced kidney failure,
can cause lactic acidosis.
Therefore,
when eGFR is equal to or greater than 60 ml/min/1.73m2 can continue to take metformin normally.
Patients with eGFR 30-59 ml/min/1.73 m2 and receiving intra-arterial contrast medium,
and those receiving intravenous contrast medium with an eGFR between 30 and 44 ml/min/1.73 m2,
should stop metformin 48 h before contrast medium and should only restart metformin 48 h after contrast medium if renal function has not deteriorated.
Metformin is contraindicated and iodine-based contrast media should be avoided for patients with eGFR less than 30 ml/min/1.73 m2,
or with an intercurrent illness causing reduced liver function or hypoxia.
In emergency patients metformin should be stopped from the time of contrast medium administration and should be restarted 48 h after.
PROTOCOL
To study the clinical guidelines for the use of iodinated contrast,
published by American and European Radiology societies there were some problems: do not cover all aspects of patient managenment (for example there specificity by technique),
is not suitable to use a unique algorithm for all patients given the variety of clinical settings as limited space, human resources,
etc.
One of the main difficulties is to set the parameter that should be used to recommend prophylaxis measures.
Several measurements have been proposed: serum creatinine concentration,
calculated creatinine clearance,
and estimated glomerular filtration rate (eGFR).
- Serum creatinine concentration,
(cutoff of 1.5mg/dL) ,
is a parameter that does not detect the 40% of risk patients because this parameter is affected by factors independent of the glomerular filtration rate .
- The clearance of creatinine,
calculated using Cockcroft-Gault formula,
takes into account the age,
weight and gender as variables.
- Glomerular filtration rate (GFR) is the best index of kidney function,
and can be calculated as estimated by the MDRM formula.
It has been shown useful especially in obese patients,
older and with diabetes mellitus.
It is essential to determinate a baseline serum creatinine before the hydration.
In emergencies we should determine eGFR if the procedure can be deferred until the result is available without harm to the patient.
There is no universally agreed upon acceptable interval between the baseline serum creatinine measurement and contrast medium administration but some autors accept a 30-day interval as adequate.
Cystatin C seems to be a promising marker of kidney function,
is independent of sex,
body mass index and less influenced by external factors.
It constitutes a more accurate marker of renal damage in patients with diabetes mellitus early.
Its cut-off point is 1.2 mgdl.
Discussed other biomarkers of renal function,
both serum and urinary needing more studies for validation.
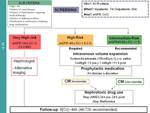
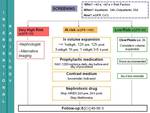
Based on the most actual and representative articles as the research basis,
and recommendations of practice guidelines of official organizations of radiology and nephrology (ESUR,
ACR,
NKF) we have proposed the following algorithms of NCI prevention in those patients that undergo a radiologic technique that requires intravascular administration of contrast iodized depending on the type of procedure,
renal function of the patient and urgency of the procedure.