Facial nerve paralysis is a frequent problem encountered in the primary care department.
Misdiagnosis of other causes of facial nerve paralysis as Bell’s palsy is not uncommon,
because they have similar clinical signs.
Radiologic techniques can provide a useful tool to get the right diagnosis.
|
The first step in imaging diagnosis of facial paralysis is to know the
anatomy and physiology of the facial nerve.
|
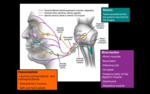
The facial nerve structure is highly complex.
In its course it provides motor control of most of the muscles of facial expression and parasympathetic innervations to the salivary and lacrimal glands.
Moreover,
it receive taste sensations from the anterior two-third of the tongue and cutaneous sensation from the skin in and around the auricle.
Motors fibers are carried via the motor facial nerve and parasympathetic,
sensorial and general somatic afferent fibers are carried via the intermediate nerve of Wrisberg (Fig. 1).
To make easier the study of the facial nerve we divide it course in topographical portions: intra axial,
apparent origin,
intra cranial course,
intra temporal course,
extra cranial and branches.
We describe the anatomy in each of these portions below.
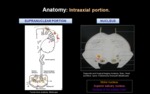
a) INTRA AXIAL PORTION: includes supranuclear connections and nucleus of origin (Fig. 2).
- Supranuclear connections: Voluntary responses of mimic expressions arise from efferent discharge from the motor area (precentral gyrus) of the cerebral cortex (facial segment in Penfiel’s homunculus diagram).
Axons run along the corticobulbar tract to the internal capsule,
through the upper midbrain to the lower brainstem,
where they synapse in the pontine motor facial nerve nucleus.
- Nucleus:
-
- Motor nucleus: Located in the ventrolateral pontine tegmentum.
Efferent fibers surround nuclei of VI cranial nerve and form small mounds on floor of 4th ventricle (facial colliculi).
- Superior salivary nucleus: Parasympathetic preganglionic neurons.
- Nucleus of the solitary tract: Sensory nucleus in the dorsal medulla.
Receives afferent fibers with gustatory information from the tongue.
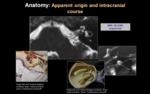
b) APPARENT ORIGIN AND INTRACRANIAL COURSE:
The facial nerve emerges from the brainstem with the nerve of Wrisberg in the cerebellopontine angle (CPA).
They run anterolaterally through the cerebellopontine cistern to the internal auditory canal (IAC).
The facial nerve and the intermediate nerve lie above to 8th cranial nerve
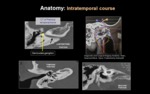
c) INTRA TEMPORAL COURSE:
At the fundus of the IAC,
the falciform crest divides it into superior and inferior compartments.
The facial nerve passes along the anterosuperior quadrant.
Through the petrous temporal bone (Fallopian canal) the nerve course is divided in three portions fot it study (Fig. 4).
-Labyrinthine: From the IAC to the geniculate ganglion (“anterior genu”).
Geniculate ganglion contains cell bodies of taste fibers from tongue.
-Tympanic: Fibers course posteriorly,
under lateral semicircular canal in middle ear.
-Mastoid: Inferiorly from “posterior genu” to stylomastoid foramen.
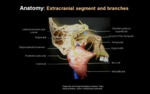
d) EXTRA CRANIAL COURSE
Facial nerve exits skull base at stylomastoid foramen.
Then it angles superiorly and anteriorly behind the posterior margin of the vertical mandibular ramus and enters into parotid gland parenchyma (lateral to retromandibular vein).
It ramifies withing parotid gland ().
e) BRANCHES
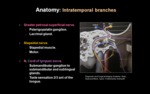
Intratemporal branches (Fig. 6):
- Greater superficial petrosal nerve:
From anterior genu.
Parasympathetic fibers synapse in pterygopalatine ganglion.
To lacrimal gland.
- Stapedius nerve:
From high mastoid segment.
Motor innervation to stapedius muscle.
- Chorda tympani nerve:
From lower mastoid segment.
Parasympathetic fibers synapse in submandibular ganglion.
To submandibular and sublingual salivary glands.
Sensory fibers 2/3 anterior of tongue.
Extracranial branches (before entering parotid gland): Posterior auricular,
digastric and stylohyoid nerves (Fig. 5).
Terminal motor branches (within parotid gland): Temporal,
zygomatic,
buccal,
orbicularis oris,
mandibular and cervical nerves (Fig. 5).
|
Once we know the anatomy,
the next step is the knowledge of
clinical signs which suggest the location of facial nerve lesion.
|
Facial nerve paralysis is a common problem that involves the paralysis of any structures innervated by the facial nerve.
It can be central o peripheral (Fig. 7).
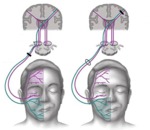
Central Paralysis:
Supranuclear injury results in paralysis of contralateral muscles of facial expression with forehead sparing.
Peripheral Paralysis:
Injury from brainstem nucleus and distal course of the nerve results in paralysis of all ipsilateral muscles of facial expression.
→ This clinical difference is due to upper facial territory is supplied by bilateral motor cortices while lower facial territory is supplied only by contralateral motor cortex (Fig.
).
Moreover:
-If lesion is proximal to geniculate ganglion: lacrimation,
sound dampening and taste are affected.
-If lesion is in pons: 6th cranial nerve injury clinical signs can be associated.
-If lesion is in the CPA-IAC region: 8th cranial nerve injury clinical signs can be associated.
-If lesion is in the extracranial portion of the nerve: lacrimation,
sound dampening and taste should be spared.
|
Finally we describe the most frequent causes of facial paralysis
according to the location of nerve injury
|
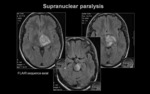
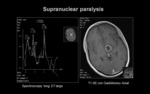
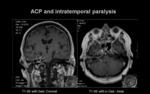
a) SUPRANUCLEAR or CENTRAL FACIAL PARALYSIS
Injury location:
Motor cortex: Precentral gyrus in frontal lobe.
Internal capsule: Genu and a few fibers in the posterior limb.
Cerebral peduncle of midbrain (medial fibers).
Clinical signs: Contralateral central facial paralysis (forehead spared) +/- contralateral limb paralysis.
Imaging technique:
Emergent CT of the brain is recommended (if acute).
Cerebral MRI can be provided without emergent character.
Etiology:
-Cerebrovascular Accident (CVA)
-In medial cerebral artery (MCA) territory: Motor cortex.
-In anterior choroidal artery territory: Internal capsule.
-In peduncular branches of posterior cerebral artery or posterior
choroidal artery territories: Midbrain.
-Intracranial bleeding.
-Tumors.
-Infectious/Inflamatory process.
b) PERIPHERAL FACIAL PARALYSIS
Bell’s palsy accounts for 75% of cases of acute peripheral facial nerve paralysis.
Etiology is not entirely understood,
with possible viral (Herpes Simplex Virus) or idiopathic origin,
which results in demyelination,
inflammation and swelling of the nerve.
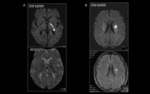
Imaging is not needed in majority of patients unless they have atypical features.
Computed tomography or MRI is indicated in the following cases to rule out other causes of facial paralysis:
• No improvement in facial paresis after one month.
• Hearing loss
• Multiple cranial nerve deficits.
• Signs of limb paresis or sensory loss.
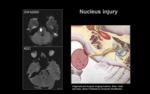
b.1) LESION LOCATED IN THE NUCLEUS
Injury location: Lower pons in the posterior area.
Clinical signs: Homolateral peripheral facial paralysis +/- lacrimation,
sound dampening and taste affectation +/- 6th cranial nerve injury clinical signs.
Imaging technique: Cerebral MRI + / - intravenous gadolinium.
Etiology:
-Cerebrovascular Accident in anterior-inferior cerebellar artery (AICA) and perforants branches from basilar artery.
-AV malformation,
cavernous hemangioma.
-Intracranial bleeding.
-Tumors.
-Infectious/Inflamatory/demyelinating process.
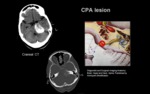
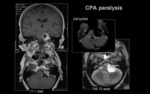
b.2) LESION LOCATED IN THE CPA.
Injury location: CPA cistern.
Clinical signs: Homolateral peripheral facial paralysis +/- lacrimation,
sound dampening and taste affectation +/- 8TH cranial nerve injury clinical signs.
Imaging technique: Cerebral MRI + / - intravenous gadolinium.
Etiology:
-AV malformation,
aneurism (antero inferior cerebelar artery).
-Intra-axial tumors.
-Extra-axial tumors: Vestibular/facial nerve schwannoma,
meningioma,
epidermoid cyst,
aracnoid cyst,
metastasis,
etc.
-Inflamatory: Meningitis.
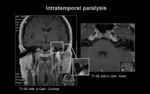
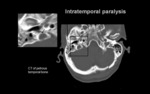
b.3) LESION LOCATED IN THE INTRATEMPORAL SEGMENT.
Injury location: Fallopian canal.
Clinical signs: It depends on the injury location.
Homolateral peripheral facial paralysis +/- lacrimation +/- sound dampening and +/- taste.
Imaging technique:
-Multidetector CT of the petrous temporal bone.
-MRI with contrast enhancement.
Etiology:
-Tumors:Cholesteatoma,
paraganglionic tumor,
metastasis,
hemagioma.Intra-axial tumors.
- Inflamatory:Bell’s palsy,
external or medial otitis.
-Traumatic.
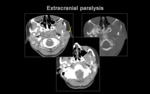
b.4) LESION LOCATED IN THE EXTRACRANIAL SEGMENT.
Imaging technique:
-Multidetector CT of the petrous temporal bone.
-MRI with contrast enhancement.
Clinical signs:
Homolateral peripheral facial paralysis
Imaging technique:
-Multidetector CT of the neck with IV contrast.
-MRI with contrast enhancement.
Etiology:
-Tumors of the parotid gland..
- Inflamatory disease of the parotid gland.
-Traumatic: previous surgery,
trauma.