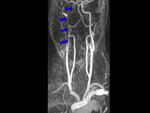
Multidetector computed tomography (MDCT) angiography allows multiplanar reconstructions and volume rendering images and it is noninvasive.
The signs found in carotid dissection are:
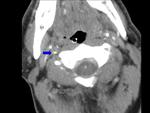
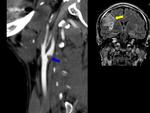
- A narrow eccentric lumen,
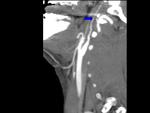
Fig. 1 Fig. 2
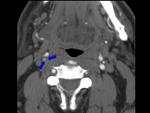
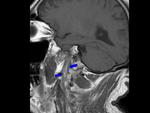
- crescent-shaped mural thickening,
Fig. 3
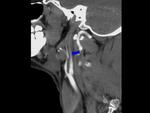
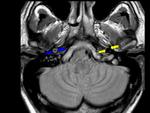
- enlargement of the overall vessel diameter,
Fig. 4
- hypodense line separating both lumens (intimal flap),
Fig. 5
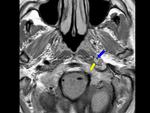
- stenosis,
Fig. 2
- occlusion,
- aneurysm formation,
- thin rim-like enhancement.
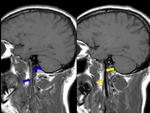
MRI allows a wide variety of sequences and modalities to asses carotid dissection.
We have the cross sectional T1WI,
T2WI and PDWI which allows to study the vessel wall and the intramural haematoma.
Also we can study the vessel lumen with imaging techniques which include MR angiography (MRA) after contrast administration (CE-MRA),
Time-of-flight MRA (TOF-MRA) and phase-contrast MRA (PC-MRA).
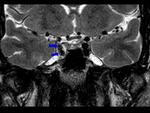
On cross sectional MRI images,
it is characteristic of carotid dissection a narrowing of the flow void surrounded by "the crescent sign",
an eccentric hyperintensity within the wall of the vessel corresponding to methemoglobine in the hematoma wall.
Increase of the external diameter of the vessel is also characteristic in this process.
Fig. 6 Fig. 8
The intramural hematoma signal depends of the stage of the blood products like in other locations.
In the early and chronic stage,
the hematoma is usually isointense to surrounding structures,
whereas between 7 days and 2 months it is almost invariably bright on T1-weighted images. However,
fresh thrombus may be misinterpreted as intramural hematoma as they can have the same appearance,
so we must look for the other signs described before to characterize the finding. Fig. 9
On the vessel lumen imaging techniques we can be demonstrated a luminal irregularity,
change of the vessel diameter or occlusion and pseudoaneurysm .
Fig. 7 Fig. 10 In addition,
on TOF-MRA images not only we can demostrate subacute intramural hematoma,
as well to evaluate the intracranial and extracranial vessels.
Fig. 11
MRI also allows to complete with other sequences that can demonstrate the repercussion of the Carotid dissection on the cerebral parenchyma such as acute strokes on Diffusion-WI.
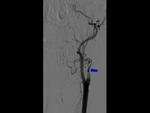
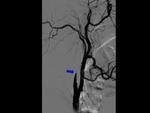
Digital subtraction angiography (DSA) has been the gold standard imaging technique to diagnose CD and for endovascular treatment.
However it is an invasive modality and only displays the endoluminal compartment.
Carotid dissection classical findings are irregular stenosis ("rat's tail sign" or "string sign") aneurysm formation and arterial occlusion.
The most frequent location of stenosis is 2-3 cm distal to the carotid bulb.
Focal narrowing with a distal site of dilatation is referred to as the “string and pearl” sign.
Fig. 12 Fig. 13
Treatment
The most cases of ischemic strokes in carotid dissection are secondary to distal embolisation,
so that anticoagulant therapy is the most accepted treatment. The first week it is administered intravenous heparin and then it is administered during 3-6 months oral anticoagulants and aspirin.
However,
anticoagulants are contraindicated in the intracranial carotid dissection,
due to the risk of subarachnoid haemorrhage and the risk of rupture in pseudoaneurysm.
Endovascular stents or surgical intervention is reserved for patients with recurrent thromboembolic events and in dissecting aneurysms.
Some of the features above described can mimic others diseases,
so it is important to perform a good differential diagnosis.
Principally the carotid dissection should be differentiated from fibromuscular dysplasia,
dysgenesis of theICA,
and other causes of arterial wall thickening (atherosclerosis,
radiation treatment,
and vasculitis).