1.
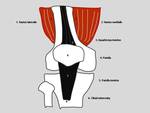
EXTENSOR MECHANISM:
The primary structures of the extensor mechanism are shown in the below drawing.

Fig. 2
PATELLAR AND QUADRICEPS TENDONS:
The patellar tendon originates in the inferior pole of the patella and inserts distally onto the anterior tibial tubercle.
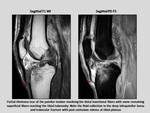
On MR imaging has a low signal intensity in all pulse sequences although due to the “magic angle” phenomenon,
the proximal patellar tendon may have not low signal and exhibit localized hyperintensity,
specially its posterior fibers,
resulting in false positive findings.
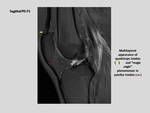
The quadriceps tendon is a multilayered tendon that consists of a superficial portion receiving the fibers of the rectus femoris muscle and a deep portion receiving fibers of the vastus intermedius muscle,
which is joined by the tendinous fibers of the vastus medialis and vastus lateralis muscles.
We find fibro-fatty connective tissue between these layers,
so the appearance on MR imaging will not be homogenously black,
as with most of the other tendons,
but will have longitudinal streaks of intermediate signal on most sequences.
Most of its fibers insert on the superior pole of the patella; however the most superficial ones (contributed by the rectus femoris) continue over the anterior surface of the patella,
forming an aponeurosis that merges into the patellar tendon.

Fig. 3
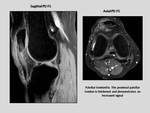
PATELLAR TENDINOPATHY:
The patellar tendon shows an intratendinous high signal on sequences T1,
T2 and STIR.
It is focally or fusiform thickened.
Its posterior aspect is the location usually involved,
next to the inferior pole of the patella and sometimes the distal patellar tendon next to the tibial tuberosity is the one affected (jumper´s knee).
Ocasionally,
there is cystic degeneration or an intratendinous cystic ganglion.

Fig. 4

Fig. 5
QUADRICIPITAL TENDINOPATHY:
It is less frequent than patellar tendinopathy and imaging findings are similar.
In teenagers,
the proximal patelar pole avulsion or the apophysitis are more often seen.
In older patients might be calcifications at the site of insertion.

Fig. 6
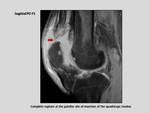
ACUTE TENDON RUPTURE:
Tendinous ruptures are usually at the sites of insertion on the patella.
MRI allows to distinguish between complete and partial ruptures.
There is a gap between the tendon and the patella in the complete ruptures,
with bleeding associated.
Partial ruptures might be low or high grade ruptures depending on the number of intact hypointense fibers on all pulse sequences we see.

Fig. 7

Fig. 8
SINDING-LARSEN-JOHANSON DISEASE (SLJD) and OSGOOD-SCHLATTER DISEASE (OSD):
SLJD is the equivalent of jumper´s knee on immature skeletons.
On MRI the proximal patellar tendon is thickened with peritendinous edema and sometimes we see ossified fragments which are secondary to the inferior patellar pole avulsion or dystrophic fragments that are developed in the tendon due to long overuse.
OSD: consists in a apophysitis due to patellar tendon traction over the tibial tuberosity.
The imaging findings are similar to the ones we find in SLJD.

Fig. 9
PATELLA:
The patella is a a sesamoid bone in the quadriceps tendon making easier its tracking on the trochlear groove.
BIPARTITE PATELLA:
It is considered an anatomic variant.
The most frequent location is the superolateral aspect of the patella.
It is usually asymptomatic but it may be painful sometimes,
on MRI we find bone marrow edema and high signal of the surrounding soft tissues on fat-supressed T2 SE or STIR sequences.

Fig. 10
FRACTURES: secondary to direct traumas.

Fig. 11
2.
LESIONS OF THE CARTILAGE/CARTILAGINOUS LESIONS:
PATELLAR CHONDROMALACIA:
It is classified in 4 grades:
- Grade 1: scattered areas of edema identified by increased signal on T2-weighted images but with an intact cartilage surface.
- Grade 2: chondral fissurations.
- Grade 3: fibrillation and crabmeat appearance.
- Grade 4: full thickness loss of hyaline cartilage with underlying reactive bony changes.

Fig. 12
CHONDRAL AND OSTEOCHONDRAL LESIONS:
Chondral lesions included chondral thinning,
fissurations or chondral defects without underlying bone marrow edema.

Fig. 13
In osteochondral lesions,
the cartilaginous lesion is accompanied by an underlying osseous fracture,
trabecular osseous lesions or reactive bony stress response.
An example of this is the osteochondritis dissecans which tipically involves the medial femoral condyle with an estable or an instable osteochondral fragment.

Fig. 14

Fig. 15
3.
PATELLOFEMORAL JOINT LESIONS:
TRANSIENT PATELLAR DISLOCATION:
It occurs in lateral direction.
There are conditions that this entity more likely such as patella alta and trochlear dysplasia (an abnormal trochlear morphology and a shallow groove).
On MRI there is a lesion of the medial retinaculum and medial capsule and post-contusive bone marrow edema appears on the anterolateral femoral condyle and the medial aspect of the patella with or without concomitant chondral lesion.

Fig. 16
OSTEOARTHRITIS:
It is a degenerative articular process with loss of articular cartilage,
cortical irregularity,
osteophytes,
subchondral cysts,
and subchondral sclerosis.
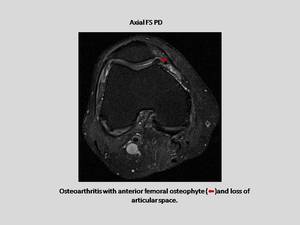
Fig. 17
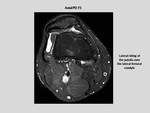
PATELLAR MALALIGNMENT:
It refers to any abnormality of the position or tracking of the patella and may potencially cause pain and/or instability.
These conditions include: lateral tilting of the patella,
lateral ridging or the combination of both.

Fig. 18

Fig. 19
4.
SURROUNDING SOFT-TISSUE LESIONS:
We refer to superficial and deep soft tissue structures surround the extensor mechanism.

Fig. 20
ANTERIOR BURSITIS:
There are three different anterior bursitis:
- Prepatellar bursitis: anterior to the inferior pole of the patella and the proximal patellar tendon.

Fig. 21
- Pretibial bursitis (superficial infrapatellar) anterior and superficial to the distal patellar tendon.
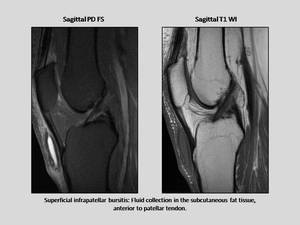
Fig. 22
- The deep infrapatellar bursitis located between the patellar tendon and the anterior aspect of the proximal tibia.
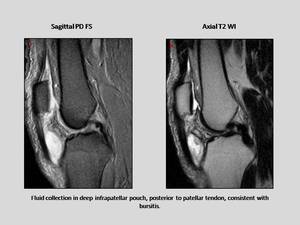
Fig. 23
SUPRAPATELLAR RECESS:
We show examples of inflammatory synovitis,
“rice-bodies” synovitis,
pigmented villonodular synovitis,
synovial ostochondromatosis and arborescens lipoma.

Fig. 24

Fig. 25
- “Rice-bodies” synovitis: it is usually secondary to reumathologic diseases (reumatoid arthritis,
systemic lupus erythematosus …) or infectious diseases (e.g.
tuberculous arthritis).

Fig. 26
- Pigmented villonodular synovitis: it is a synovial proliferation with characteristic hemosiderin deposition.

Fig. 27
- Synovial osteochondromatosis: it is characterized by the synovial proliferation and metaplasia with formation of cartilaginous loose bodies that may calcified and/or ossified.

Fig. 28
FAT PAD SYNDROMES:
1) HOFFA´S FAT PAD:
Hoffa´s fat pad is an intraarticular and extrasinovial estructure located posterior to patella tendon and anterior to the intercondylar notch and the ACL.
Hoffa´s fat pad syndome: it is produce due to the impingement between the intercondylar fat pad and the tibial plateau during extension of the knee.
On an acute onset,
there is inflammation identified by high signal on T2 WI and small effusion; on chronic stages there is low signal on T1 and T2 WI secondary to fibrin and hemosiderine deposition.

Fig. 29
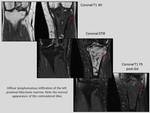
Impingement of the superolateral aspect of the fat pad: it is caused by the impingement of the Hoffa´s fat pad due to the altered biomechanic of the femoropatellar Joint.
On MRI edema in the superior aspect of the Hoffa´s fat pad is seen,
between the patellar tendon and the lateral femoral condyle.

Fig. 30
Ganglion in Hoffa´s fat pad: a cystic benign lesion.

Fig. 31
Vascular lesion: synovial hemangioma.
It shows intermediate signal on T1,
very high signal on T2 with lineal fibrous septa,
phlebolytes and intense enhancement after gadolinium injection.
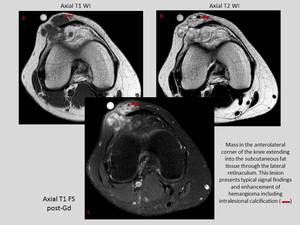
Fig. 32
Tumours: we show examples of:
- Localized nodular synovitis: it is a benign neoplasm of the synovium.
Typically appears as an ovoid mass which may be iso or hyperintense on T1 WI related to skeletal muscle and with variable signal on T2 WI and enhancement after contrast administration.
The infrapatellar fat pad is the most frequent location.

Fig. 33
- Tenosynovial giant cell tumour: also called nodular tenosynovitis or fibrous histiocitoma of the synovial membrane.
It is a benign proliferative process affecting the synovial membranes histologically related to pigmented villonodular synovitis.
It is considered the extraarticular form of pigmented villnodular synovitis.

Fig. 34
- Hoffa´s fat pad chondroma: it originates from the articular capsule or the connective tissue that surrounds the capsule.
On MRI it shows intermediate signal on T1 WI,
heterogeneous signal on T2 WI with areas with similar signal to that of bone marrow in all pulse sequences and predominantely peripheral enhancement.

Fig. 35
2) QUADRICEPS´S FAT PAD:
This fat pad lies between the distal quadricipital tendon anteriorly,
the patella distally,
and the suprapatellar recess posteriorly.
There is edema sometimes and convexity of its dorsal margin causing mass effect on the suprapatellar recess.

Fig. 36
PLICA SYNDROME:
Plicae are folds of embryonic remnants of synovial membrane into the knee joint.
There are three different types of synovial plicae:
- Mediopatellar plica: localized in the medial aspect of the knee joint descending oblicually and inserts on the synovial lining of the Hoffa´s fat pad.
- Suprapatellar plica: its extents from the inferior portion of the quadriceps tendon to the medial aspect of the knee joint.
- Infrapatellar plica: also known as ligamentum mucosum.
It arises from the intercondylar notch,
widens as it descends through the infrapatellar fat pad,
anterior to the ACL.
On MRI the plicae appear as linear low signal intensity structures surrounded by articular fluid and they are usually asymptomatic.
Some conditions such as direct trauma or overuse may affect the pliability of the synovial folds and can become symptomatic.
The mediopatellar plica is considered the most likely to cause problems.
In these cases the plica becomes thickened,
with high signal on T2 WI and chondral lesions in the medial aspecto of the patella may be associated.

Fig. 37
ILIOTIBIAL BAND SYNDROME:
It is the result of inflammation an irritation of the distal portion of the iliotibial band as it rubs against the lateral femoral condyle during exercise.
It is seen in long distance runners,
cyclists,
and other activities with repetitive flexion and extension of the knee.
On MRI the iliotibial band is thickened and the soft tissues interposed between this band and the femoral condyle show high signal on T2 WI and STIR sequences.
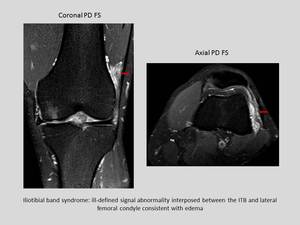
Fig. 38
5.
INTRAMEDULLARY ABNORMALITIES OF THE KNEE:
- TUMOURS: are rare and cause focal destruction of bone.
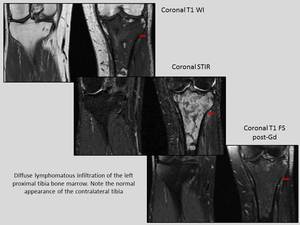
Fig. 39
- BONE INFARCTS: metaphysis is the most frequent location,
they show irregular or serpinginous morphology with a typical “double line sign”.
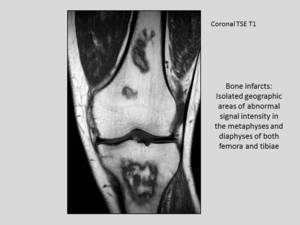
Fig. 40
- INFECTION: acute osteomyelitis,
as in the following example.
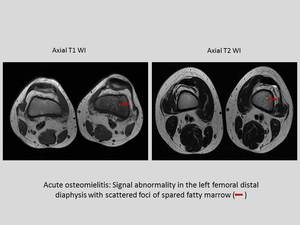
Fig. 41
6.
EXTRAARTICULAR ORIGIN:
Hip must be always explored.
Anterior knee pain may be an irradiation of pain perception due to a hip lesion or due to malalignment of the lower limb.