We revised the patients with proven EPTB in a retrospective 10-year (2002-2012) study performed in our hospital.
We retrieved 20 patients with microbiologically confirmed EPTB and we performed a posterior revision of their imaging data and clinical histories.
We present a pictorial review of different locations of EPTB,
according to our experience: 9 tuberculous lymphadenitis,
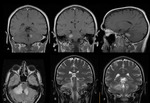
2 central nervous system (CNS) TB,
3 urinary TB,
1 tuberculous pericarditis,
3 musculoskeletal TB (2 spondylitis and 1 arthritis),
1 splenic TB,
and 1 gastrointestinal TB.
Tuberculous Lymphadenitis
Lymphadenitis is the most commonly occurring form of EPTB.
Cervical nodes are most frequently affected,
accounting for approximately 63% of cases,
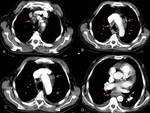
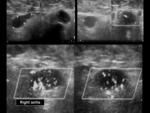
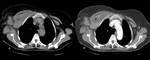
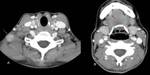
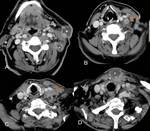
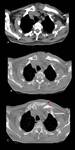
followed by mediastinal (27%) (Figure 1) and axillary ones (8%) (Figure 2 and Figure 3), but submandibular,
intraabdominal,
inguinal and intramammary locations were also described.
TB cervical lymphadenitis (also known as Scrofula or King's evil) is the most common manifestation of EPTB and is a very frequent cause of peripheral lymphadenitis.
Within the neck,
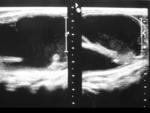
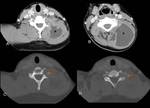
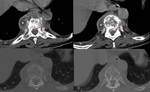
the nodes in the posterior triangle (51%) (Figure 4 and Figure 5) and deep upper cervical (48%) are more frequently involved than others.
In the majority of cases lymphadenitis is unilateral.
Ultrasound (US) is an excellent first line investigation,
able to assess cervical lymphadenopathies and to enable guided fine needle aspiration cytology if necessary.
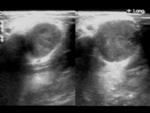
On gray-scale US,
TB nodes tend to be hypoechoic,
round,
without echogenic hilum and tend to show intranodal cystic necrosis,
nodal matting,
and adjacent soft-tissue edema.
On color Doppler,
power Doppler,
and 3D sonography,
the vascular distribution of TB nodes is varied.
However,
displacement of hilar vascularity is common and is due to the high incidence of intranodal cystic necrosis,
which displaces the vessels (Figure 6).
CT appearance of TB lymphadenitis is variable,
depending on the degree of caseation present in the node.
Nodes may initially appear merely enlarged (Figure 7),
often with attenuation similar to muscle.
Eventually central caseation develops and the nodes become centrally low density and eventually frankly cystic,
with peripheral rim enhancement (Figure 8).
They are usually matted together with only minor surrounding inflammatory changes.
On MRI the involved nodes are initially homogeneously enlarged but later undergo central necrosis,
manifesting with central hypointensity and hyperintensity on T1- and T2-weighted MR images,
respectively.
Finally,
cystic transformation with peripheral enhancement is seen.
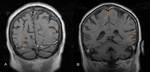
Central Nervous System (CNS) Tuberculosis
CNS tuberculosis (TB) is uncommon; involvement of the CNS is seen in approximately 5% of patients with TB,
with a greater prevalence in immunocompromised ones (up to 15% of cases of AIDS– related TB).
CNS TB usually results from hematogenous spread,
or from direct rupture or extension of a subependymal or subpial focus (Rich focus) and may be located in the meninges,
brain,
or spinal cord.
CNS TB can manifest in a variety of forms,
including tuberculous meningitis,
tuberculomas,
tuberculous abscesses,
tuberculous cerebritis,
spinal tuberculous arachnoiditis and miliary tuberculosis.
The most common parenchymal lesion of CNS TB is tuberculoma (tuberculous granuloma).
This lesion may be solitary,
multiple,
or miliary and may be seen anywhere within the brain parenchyma,
although it most commonly occurs within the frontal and parietal lobes.
At CT,
tuberculomas appear as round or lobulated masses with low or high attenuation.
They demonstrate homogeneous or ring enhancement and have irregular walls of varying thickness.
One-third of patients demonstrate the “target sign” (central calcification or punctate enhancement with surrounding hypoattenuation and ring enhancement).
This finding is highly suggestive of,
but not pathognomonic for,
tuberculosis.
The MRI findings depend on whether the tuberculoma is caseating.
It is thought that there is a progression from a noncaseating (solid) to a caseating (liquid) center.
A noncaseating tuberculoma is hypointense relative to gray matter on T1W and hyperintense on T2W images,
with homogeneous gadolinium enhancement.
Caseating tuberculomas with a solid center are isointense to hypointense on both T1- and T2W images.
They usually have a variable amount of surrounding edema (hyperintense on T2W images) (Figure 9).
Caseating tuberculomas with a liquid center are hypointense on T1-W images and centrally hyperintense on T2-W images,
with a peripheral capsule (seen as a hypointense rim on T2-W images).
Rim enhancement is usually seen at gadolinium-enhanced MRI (Figure 10).
After treatment,
tuberculomas can completely resolve; however,
calcification is seen in up to one-fourth of cases and is identified most clearly at CT.
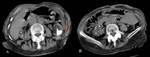
Urinary Tuberculosis
Urinary TB is a common clinical manifestation of EPTB,
more frequently seen in young males.
The kidney,
the epididymis and the collecting system are usually first infected; the other genitourinary organs may be affected by ascendant or descendant dissemination.
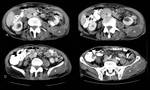
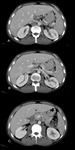
Approximately 75% of renal TB involvement is unilateral,
the most common CT finding being renal calcification (50% of cases) (Figure 11). At intravenous urography,
the earliest abnormality is a “moth-eaten” calix due to erosions,
which progresses to papillary necrosis.
Hydronephrosis tends to have irregular margins and filling defects owing to caseous debris.
Renal parenchymal cavitation may be detected as irregular pools of contrast material.
Dilated calices (hydrocalicosis) with related infundibular stricture at one or more sites within the collecting system may be seen.
Characteristic calcifications in a lobar distribution are often seen in end-stage tuberculosis (tuberculous autonephrectomy).
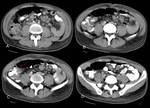
Sometimes an iliopsoas abscess may be originated from kidney involving (Figure 12).
Musculoskeletal Tuberculosis
The musculoskeletal TB accounts for up to 35% of all forms of EPTB,
and up to 2% of all cases of tuberculosis.
Tuberculous Spondylitis
Approximately 50% of skeletal tuberculosis involves the spine (mostly the lower thoracic and upper lumbar levels),
with TB spondylitis.
Infection usually begins in the anterior part of the vertebral body adjacent to the end plate,
with subsequent demineralization,
seen on conventional radiographs as loss of definition of its dense margins.
The classic pattern is the involvement of more than one vertebral body together with the intervening disks.
Tuberculosis rarely affects the posterior vertebral elements (including the pedicles) and is characteristically associated with little or no reactive sclerosis or local periosteal reaction,
a feature that helps distinguish it from pyogenic infections of the spine.
TB spondylitis also allows spread into the paraspinal tissues,
resulting in the formation of a paravertebral abscess known as a Pott abscess.
Calcification within the abscess is virtually diagnostic for tuberculosis.
If left untreated,
the infection eventually results in vertebral collapse and anterior wedging,
leading to kyphosis and gibbus formation.
With healing,
ankylosis of the vertebral bodies occurs,
with obliteration of the intervening disk space.
CT is especially useful for guided fine needle aspiration cytology or biopsy.
MRI is the preferred imaging modality in the diagnosis of TB spondylitis,
in order to assess the soft-tissue abnormalities and the possible medullary compression.
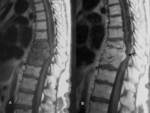
In a Pott abscess the disc and the adjacent vertebral plates are hyper-intense on STIR and T2W MRI,
and hypointense on T1W MRI,
with intense Gadolinium-enhancement (Figure 13 and Figure 14).
Tuberculous Arthritis
Tuberculous arthritis is characteristically a monoarthritis affecting large weight-bearing joints like hip and knee.
There are no pathognomonic radiological findings for TB arthritis.
Nonspecific changes may be seen,
such as juxtaarticular osteopenia,
synovitis and other soft-tissue swellings,
marginal erosions,
and varying degrees of cartilage destruction.
Joint space narrowing is usually delayed.
The end result is usually fibrous ankylosis of the joint.
Factors favoring a diagnosis of tuberculosis include insidious onset,
minimal sclerosis,
the relative absence of periosteal reaction and bone proliferation,
and relative preservation of joint space in the early stages (Figure 15).
Tuberculous Pericarditis
Tuberculosis involving the heart is rare,
accounting for only 0.5% of cases of EPTB.
The main presenting finding is pericardial involvement,
particularly in immunocompromised patients.
The primary sign of TB pericarditis is pericardial thickening of more than 3 mm in adults,
seen in the majority of cases.
CT demonstrates a thickened,
irregular pericardium,
frequently with associated mediastinal lymphadenopathy.
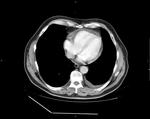
Most patients have distention of the inferior vena cava to a diameter exceeding 3 cm; pleural effusions,
typically bilateral; and deformities of the intraventricular septum.
Less than 20% of patients have pericardial effusions (Figure 16) or develop localized pericardial calcification.
Splenic Tuberculosis
Tuberculous splenic involvement is very rare and it is most likely secondary to hematogenous dissemination of the primary form of the disease.
Miliary splenic TB manifests as multiple tiny (0.5-2.0-mm),
low-attenuation foci on CT (Figure 17) and multiple hypoechoic nodules on US.
The macronodular form is rare and manifests as diffuse splenic enlargement with multiple low-attenuation lesions or a single tumorlike mass.
On contrast-enhanced CT,
early-stage lesions may demonstrate central enhancement whereas more advanced lesions may demonstrate calcification.
Intraabdominal lymphadenopathies are usually seen.
Gastrointestinal Tuberculosis
Gastrointestinal tuberculosis is rare; when present,
however,
it almost always involves the ileocecal region (90% of cases),
usually both the terminal ileum and the cecum,
with or without proximal dilatation.
The most common CT finding is mural thickening,
which is typically concentric but if eccentric tends to involve the medial cecal wall.
Localized lymphadenopathy is usually seen (with hypodense center that represents the caseum).
(Figure 18)