Magnetic resonance imaging (MRI) has an important role in detection and characterization of changes in muscular signal caused by different pathologic conditions.
MRI allows an optimal evaluation of anatomical detail and muscles morphology.
T1 weighted images (T1WI) are the best suited for the evaluation of anatomy and also provide presence of subacute haemorrhage and muscle atrophy. T2 weighted images (T2WI) are indispensable to detect edema and therefore pathology. Contrast-enhanced T1WI are useful to differ solid lesions and recognise muscular abscesses.
Diffusion weighted images (DWI) help to detect subtle muscular edema and to characterize mass like lesions.
MRI is necessary to decide a suitable treatment,
on some occasions avoiding unnecessary manipulations,
and,
when diagnostic biopsy is necessary,
MRI helps to choose the most accurate place.
Although the MRI findings are often slightly specific,
recognize the described patterns of signal alteration and correlate them with clinical history can allow a correct diagnosis.
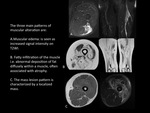
The three main patterns of muscular alteration are:
(FIGURE 1)
1.Muscular edema: is seen as increased signal intensity on T2WI,
superimposed on an otherwise normal appearance of the involved muscles.
It can be focal or a diffuse alteration.
When edema is subtle it can be only detectable with fat saturation sequences.
2.
Fatty infiltration of the muscle i.e.
abnormal deposition of fat diffusely within a muscle,
often associated with atrophy,
it occurs in the chronic stages of many pathologies.
3.
The mass lesion pattern is characterized by a localized mass with morphology and signal different from normal muscle.
We will describe not tumoural muscular principal pathologies,
most of them appearing with any of these three patterns of signal intensity abnormality.
TRAUMATIC INJURIES
Acute traumatic muscle damage may be caused by two principal mechanisms: direct compression,
causing muscle contusion and hematomas,
or indirect injury by excessive lengthening of muscular fibers resulting in injuries from small myofibrilar strain to complete tear of the muscle.
These lesions are associated to a greater or lesser amount of haematic component,
often reabsorbed in weeks.
Sometimes hematoma can persist chronically causing a functional limitation or nonspecific discomfort.
Muscles located deeper into contact with osseous structures are more prone to be injured by direct trauma while superficial muscles are more prone to be injured by excessive lengthening.
In general,
indirect injuries are more frequent than direct trauma damages.
Injuries usually occur in anatomic and functional transition zones,
often in the vicinity of the musculotendinous junction (not in the musculotendinous junction itself).
Muscle tears occur most frequently in muscles that cross two joints,
contain fast-twitch fibers,
and contract during elongation (eccentric contraction).
The hamstring,
gastrocnemius,
and biceps brachii muscles have these features and are the most frequently affected.
A mild muscle strain causes muscle signal intensity changes on MRI consistent with edema.
More severe muscle tears may present mass-like features of MRI because of presence of fluid collections (haematomas) and grossly interrupted muscle fibers.
The image of the tear depends largely on the degree of injury and the elapsed time from trauma.
In the first 48 hours occurs an inflammatory response in breakage region with hyperemia and fibrillar necrosis.
The inflammatory component continues at least 2 weeks.
Muscular remodeling may take months due to stress forces.
Adapted from studies by ultrasound,
a fibrilar injuries degree classification has been described.
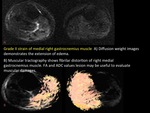
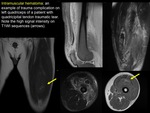
Grade I tears are secondary to fibrillar distraction beyond muscle compliance and are defined on MRI as high signal intensity due to intersticial haemorraghe and edema,
without tear (or with a tear affecting less than 5% of muscle fibers) and with musculotendinous junction maintained.
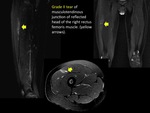
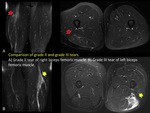
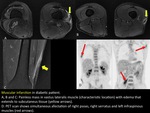
Grade II tears are secondary to a greater contraction causing endomysium and perimysium rupture and identifying fibers discontinuity with a hematic component.
(FIGURE 2).
Depending on the type of muscle,
the location of the lesion will be variable.
In some muscles (e.
g.
the peronei) the fibers are,
like the plumes of a quill pen,
to one side of a tendon,
which runs the entire length of the muscle; such muscles are termed unipennate.
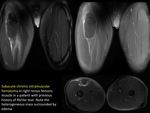
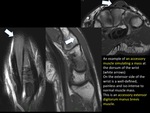
In this muscle type the musculotendinous junction lies superficial and may be associated epimysium rupture even in small lesions.
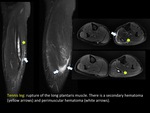
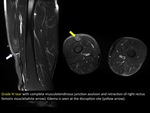
An example is the “tennis leg” affecting the distal region of the medial gastrocnemious (some authors exclusively call “tennis leg” when there is an injury of long plantaris muscle).
(FIGURE 3).
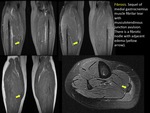
When there is epimysium rupture is called muscle-aponeurotic avulsion by some authors.
Breakage of the epimysium associates abundant perimuscular hematic component and usually heals in an exuberant way.
(FIGURE 4).
As grade II lesions have a very wide range of severity its recovery times are highly variable.
New technological advances in MRI with diffusion-tensor imaging (DTI) and fiber tractography (FT) can contribute to a more accurate approximation to the injuries extension and prognosis.
MRI new technical advances will be more deeply explained later.
(FIGURE 5).
Grade III tears correspond to a complete disruption of the muscle belly with or without muscular retraction.
Breakage usually occurs in patients with mature skeleton and without tendon degeneration.
(FIGURE 6).
(FIGURE 7)
Muscle atrophy (with fatty infiltration pattern) will occur if grade III and extensive grade II lesions are not repair.
(FIGURE 8)
Some pathology may mimic muscular injuries by elongation after sports practice.
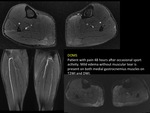
DOMS (delayed-onset muscle soreness) is a type of overuse injury without fibers breakage that does not become symptomatic until 24 to 48 hours after the episode (in contrast with muscular tears or contusions that are usually immediately painful).
DOMS is often due to uncommon intense efforts in recreational athletes.
It is a benign,
self-limiting inflammatory response and requires no medical action,
although severe forms may progress to rhabdomyolysis.
(FIGURE 9).
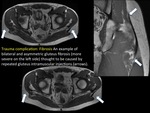
MUSCULAR COMPLICATIONS OF TRAUMATIC INJURIES
Moderate to severe muscle strain,
laceration and contusion may be complicated with a mass-like lesion associated to edema due to true intramuscular hematomas (instead of interstitial haemorrhage seen more frequently).
(FIGURE 10).
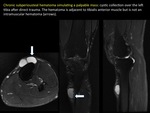
Intramuscular hematoma is usually reabsorbed spontaneously in about 6-8 weeks.
Occasionally,
the hematoma is not reabsorbed and it can persist over time in the form of chronic cystic haematoma causing chronic discomfort.
Cystic hematomas on MRI may mimic an intramuscular abscess since these lesions may contain fluid-fluid level and demonstrate surrounding edema.
(FIGURE 11).
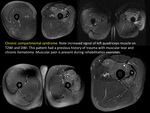
Compartment syndrome appears due to increased pressure within an enclosed space.
Acute compartment syndrome is a medical emergency and can occur secondary to an intramuscular hematoma.
Chronic compartment syndrome is usually a diagnosis of exclusion frequently seen in athletes causing pain during exercise (when muscle increases its volume).
The perimuscular aponeurosis does not expand and press on the muscles,
blood vessels and nerves.
Early MRI findings include extremity swelling and diffuse edema.
His treatment involves the fascial release.
(FIGURE 12).
Muscle fibrosis can be a muscular trauma complication.
Breakage of the epimysium may lead to fibrotic cicatricial changes seen as low signal nodules on MRI .
(FIGURE 4).
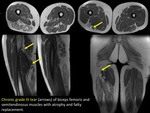
Chronic muscle injuries can lead to muscular fibrosis causing deformities and muscular signal intensity changes on MRI.
(FIGURE 13).
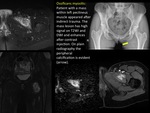
Other severe and late muscular complication is the development of Myositis ossificans,
seen as an intramuscular mass with internal calcification.
Sometimes traumatic background is not remembered for the patient and it is difficult differential diagnosis with some tumours as sarcoma (although the sarcoma calcifications tend to be central whereas Myositis ossificans has a peripheral calcification).
(FIGURE 14).
Rhabdomyolysis is a severe muscle complication characterized by loss of integrity of muscle cell membranes and it may result from a variety of insults,
including trauma,
severe exercise,
ischemia...
MRI initially reveals edema throughout the involved muscles (being the severity of the signal intensity correlated with the severity of injury) progressing to myonecrosis in late stages.
MUSCULAR INJURIES PITFALL
Extramuscular injuries caused by direct trauma as subperiosteal hematomas can be misdiagnosed as true muscular injuries.
(FIGURE 15).
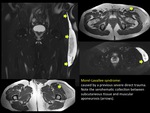
One example is Morel-Lavallee syndrome.
It consists on a chronic subperiosteal haematoma caused by closed degloving injuries representing a traumatic severance of the skin and subcutaneous tissue from underlying fascia.
This injury disrupts segmental perforating vessels and results in a hematoma composed of hemolymphatic fluid with a mixture of viable and necrotic fat.
Its most frequent location is the external aspect of the thigh.
Due to its tendency to relapse,
often is required surgical drainage with planes closure.
(FIGURE 16)
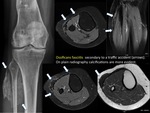
Ossifying fasciiitis is a rare benign tumour composed of metaplasic bone originated from subcutaneous or deep fascial tissues with a rapidly growing.
It must be differentiated of a true muscular affection.
Sometimes causes a chronic compartment syndrome associating muscular edema.
(FIGURE 17).
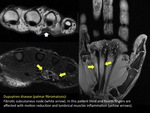
Fibrotic extramuscular pathology as the fibromatosis can secondarily affect adjacent muscles simulating a sequel of muscular lesion.
One example of fibromatosis is Dupuytren contracture or palmar fibromatosis that may cause secondary edema of interosseous and lumbricals muscles.
(FIGURE 18).
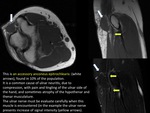
ACCESSORY MUSCLES
A good number of accessories and supernumerary muscles have been described in the scientific literature.
In the majority of cases are asymptomatic and are discovered as incidental findings in image.
However,
in some cases,
they may cause symptoms related to palpable masses or to mass effect. (FIGURE 19) (FIGURE 20).
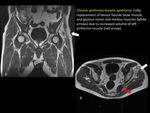
Accessory muscles may also be symptomatic if they are located in an enclosed region occupying space and damaging adjacent structures.
(FIGURE 21)
Sometimes,
accessories muscles cause symptoms secondary to an internal trauma.
An example of this trauma mechanism is seen when the third peroneal tendon is present (the peroneus tertius tendon).
When present,
it is located in the anterior compartment of the leg passing deep to the inferior extensor retinaculum,
to insert onto the fifth metatarsal.
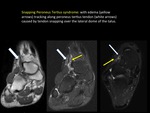
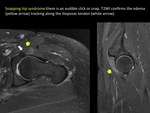
This inconstant tendon may cause snapping over the lateral dome of the talus (“Peroneus Tertius friction syndrome”) (FIGURE 22) with a similar lesion mechanism to the syndrome known as “Snapping Hip”.
(FIGURE 23).
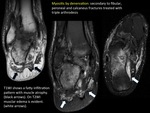
MUSCULAR INJURY BY DENERVATION
A muscle and the nerve that innervate it compose a motor or neuromuscular unit.
Damage of a nerve causes changes on muscles innervated by it.
The signal intensity alteration of the affected muscle groups can be identified on MRI and orients us to the involved root or nerve fascicle.
The utility of the MRI has been described to identify both the cause of denervation and the muscle groups involved.
Potential mechanisms of denervation are many: injury of the spinal cord,
polio,
peripheral nerve injury,
nerve entrapment,
neuritis… The pathology of a neuromuscular unit in the acute phase hasn’t MRI abnormal findings.
Later,
after about 2 weeks,
muscular denervation causes inflammatory changes with muscular edema,
which may persist until one year after the damage.
Subsequently the affected muscle begins to develop atrophic changes with fatty replacement (muscle edema may persist).
Finally the irreversible fatty replacement of the muscle belly is the predominant alteration.
These changes are nonspecific unless there is a typical muscular affectation that correlate with a neuromuscular unit.
In some cases the first phases go unnoticed and muscle atrophy is the first finding.
Differential diagnosis must be done with non-neurologic conditions causing fatty replacement and mimicking chronic denervation such as chronic muscle disuse secondary to chronic tendon tear,
long use of corticosteroids and intramuscular hemangiomas.
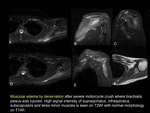
Etiologies of traumatic peripheral nerve injury include penetrating injury,
crush,
traction,
ischemia,
and less common mechanisms such as thermal,
electric shock,
radiation,
percussion,
and vibration.
(FIGURE 24).(FIGURE 25)
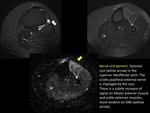
There are multiple nervous entrapment syndromes that may cause nervous lesion and would be associated with muscular alteration due to denervation.
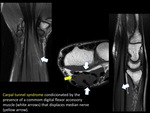
Some examples of the most common nervous entrapment locations are the carpal tunnel (FIGURE 26),
retroepitroclear tunnel (FIGURE 21),
and the tarsal tunnel.
Some of the possible causes or nerve entrapment are muscle hypertrophy (FIGURE 27) (FIGURE 28) (FIGURE 29) or mass lesions such as accessory muscles or synovial cysts.
(FIGURE 21) (FIGURE 30).
Idiopathic syndromes probably caused by autoimmune neuritis without apparent cause affect characteristically muscular groups depending of different nerve roots.
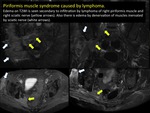
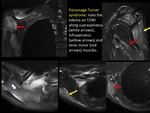
Parsonage - Turner syndrome is one example of idiopathic neuritis.
It is characterized by brachial plexus inflammation causing infraspinatus and supraspinatus muscle edema by denervation (may exist also affectation of the deltoid and teres minor muscle).
It is usually a self-limited process,
and there is often a complete recovery.
(FIGURE 31)
MYOSITIS
Multiple processes can be accompanied by inflammatory myositis causing pain and muscle swelling and presenting usually MRI features similar to the initial alteration seen in muscle denervation that should be considered in the differential diagnosis.
(FIGURE 32).
The infectious pathology is usually related to the manipulation of traumatic blood collections.
The pyomyositis can manifest with the presence of muscle abscesses (easily identifiable with MRI),
or it can appear as a muscle signal intensity diffuse alteration.
When there is a diffuse alteration the diagnosis is more complicated and is largely based on clinical suspicion.
The tropical pyomyositis very often has a clear history of recent travel to endemic countries.
The non-tropical pyomyositis is almost always related to muscular trauma or muscular strain (although muscular trauma episode is not always remembered).
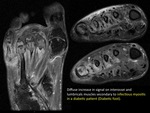
A particular case of muscular infectious process is the diabetic foot with myositis and distal osteomyelitis in long evolution diabetic patients.
In our assessment by MRI we must suspect the possibility of proximal infectious spread through tendons.
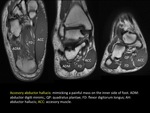
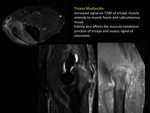
(FIGURE 33) Another inflammatory process associated with long evolution diabetes is muscle infarction.
We must consider this diagnosis in diabetic patients with not distal muscle swelling,
usually painless and very often affecting the quadriceps femoral (often vastus lateralis).
(FIGURE 34)
Other causes of inflammatory muscular pathology are iatrogenic,
secondary to treatments like myositis due to radioteraphy.
It seems to be a vascular injury accompanied by endothelial proliferation,
inflammation and ischemia within 3-10 months after exposure.
It is seen as muscular edema on T2WI with mild enhancement on T1-contrast enhanced images.
Also it may be seen a band like appearance,
corresponding with the radiation field.
The subacute myositis usually resolves within six months to one year.
(FIGURE 35).
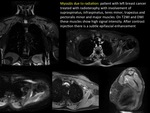
Radiation recall is a rare and infrequently reported adverse effect of radiotherapy.
Gemcitabine (GEM) is the most common leading agent to cause radiation recall myositis.
Toxicity of GEM occurs when given concomitantly or followed by radiation.
MRI of affected muscular groups shows edema and inflammation consistent with myositis.
Recall reactions usually regress with cessation of responsible agent.
(FIGURE 36).
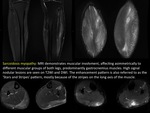
Other disease may associate muscular inflammation is Sarcoidosis,
a systemic disorder of unknown etiology characterized by noncaseating epithelioid granulomas.
Symptomatic muscle disease is rare,
however biopsy demonstrates skeletal muscle granulomas in 50-80% of sarcoidosis patients.
The most commonly involved site is the lower extremity.
The most common MRI findings are proximal muscle atrophy (fatty replacement).
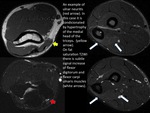
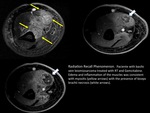
Nodular sarcoidosis manifests as focal intramuscular masses with classical MRI findings described as ,
“3 stripes” and “dark star” signs.
The finding described as “dark star” is due to the appearance of lesions with low signal intensity central rounded by a bright rim on T2WI and contrast-enhanced images.
DWI findings in muscular sarcoidosis are high signal intensity in those affected muscle groups due to severe inflammation.
(FIGURE 37).
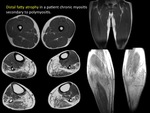
IDIOPATHIC INFLAMMATORY MYOPATHIES
The most common myopathies are idiopathic inflammatory myopathies including Dermatomyositis,
Polymyositis,
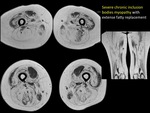
and Body inclusion myositis.
A specific pattern of muscular involvement was established for each muscular disease. MRI is useful to help diagnosis identifying the presence of muscular edema (in acute phases) and its distribution (usually bilateral and symmetrical distribution).
Moreover the MRI can help demonstrate involvement of subcutaneous tissue and associated soft tissue inflammation.
A characteristic sign is the presence myofascial edema associated.
(FIGURE 38) MRI can also demonstrate muscle calcification and muscular fatty infiltration in late phases of these diseases.
(FIGURE 39) (FIGURE 40) In any case the differentiation between these pathological entities cannot be exclusively with the MRI and the determination of autoantibodies,
the analysis of dermatologic pathology and finally muscle biopsy is necessary.
MRI is also helpful as a guide for muscle biopsy looking to an area with more inflammatory changes,
avoiding carrying out blind biopsies that may not be conclusive.
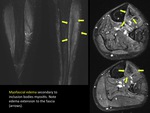
MYOFASCITIS
The initial muscular alteration in myositis may involve successively muscular fascia,
thus progressing into myofascitis.
The typical MRI finding in myofascitis is related to edema that will be seen on fat-suppressed sequences as a focal or diffuse pattern of high signal intensity (“comb-like”) involving musculofascial structures.
(FIGURE 32)(FIGURE 38) MRI is helpful indicating the edema extension and detecting possible fluid collections. MRI is very sensitive in detection of tissue edema,
but it is not specific.
When a “comb-like” appearance is present it only indicates a non-specific myofascitis.
Clinical correlation and more diagnostic analysis must be done for achieve an accurate diagnosis.
NEW MRI TECHNIQUES
The new MR techniques applied primarily to the study of sports injuries include the use of the diffusion tensor (DTI).
Its application in the study of the central nervous system is widely implemented,
but until these last years has not begun to be used in the evaluation of muscular pathology with encouraging results.
In anisotropic tissues such as skeletal muscle,
a 3D tissue fiber structure can be assessed with fiber DTI based muscle fiber tracking.
The diffusion weighted images can be crucial in the precocious diagnoses since early signal changes may be present even before changes in the fat saturation-T2W occur,
allowing an early detection of presence of muscle edema (which is common to most of muscular pathologies),
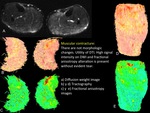
MR tractography provides a good approach of the muscle shape and the orientation of the muscle fibers.
(FIGURE 41) Also with DT-MRI data averaged microstructural parameters,
i.e.
the fractional anisotropy (FA) and the mean apparent diffusion coefficient (ADC) can be obtained.
(FIGURE 5) DT-MRI and tractography assessment is a non-invasive,
reproductive test that may be used to evaluate cellular microstructure,
muscle damage,
microstructure and architecture,
demonstrating differences in microstructural values after muscular exercises and among patients with muscle lesions from healthy controls.
These data suggest its possible utility in the evaluation of the evolution of muscle lesions,
which would be of great importance in selected patients as elite athletes where recovery time is essential.
More studies will be needed to corroborate this new application.