Usually the diagnosis of the CAB approach begins with ultrasound,
is generally indicated by the symptoms secondary to mass effect,
although it is sometimes seen when testing for other causes.
After identifying the lesions on ultrasound usually complements the study with CT and in some cases of diagnostic uncertainty complements MRI.
Among the most commonly visualized findings in the CAB include:
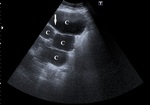
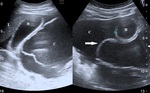
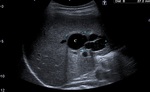
- Ultrasound anechoic cystic lesions of varying sizes,
most often with thick septa hyperechoic intrahepatic.
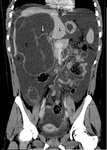
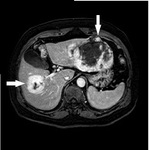
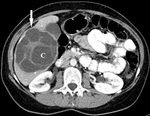
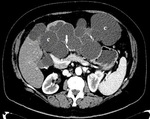
- TC: Confirm ultrasound findings,
observing liquid containing lesions with thick septa that can contrast-enhanced and sometimes have nodules on their wall.
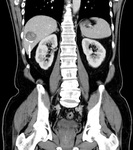
CT also allows better anatomical localization of lesions as pre surgical study,
would observe other findings such as ascites and other signs of compression of adjacent structures by mass effect.
They may have a calcified wall.
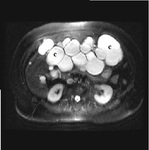
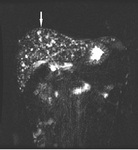
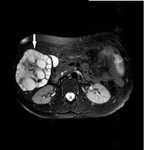
- RM: They are hypointense on T1 and hyperintense on T2 variably evenly,
with its wall enhancement after administration of gadolinium.
In differential diagnosis should be done with congenital diseases among which are simple cysts, which usually have thin wall without septa without contrast enhancement,
biliary hamartomas are usually multiple and small but no communication with the biliary tree,
which are useful for observing cholangiographic sequences of magnetic resonance,
unlike caroli disease cystic dilation observed that are up to 5 cm and communicate with the biliary tree,
the vessel site may view inside after administration of in the portal phase contrast.
For neoplastic diseases,
must be distinguished from hemangiomas whose irregular outline and progressive centripetal nodular enhance after contrast administration in late stages,
helps eliminate this possibility,
while tumor personal history (especially lung,
breast,
pancreas and melanoma among others) requires discarding cysts metastases,
also depending on their histological features may have variable patterns of contrast.
Inflammatory diseases must be ruled out include abscesses that ultrasound can have septa,
fluid levels and internal echoes while enhancing the wall after administration of contrast evident in the sequences surrounding edema on T2-weighted MRI,
while perhaps hydatid cysts diagnosis is more difficult to dismiss as these also are anechoic cystic lesions on ultrasound,
CT is observed in greater tendency to calcification of its wall also may have wall enhancement on both CT and MRI,
also vesicles mothers usually T2 hyperintense more daughter cysts,
noting membranes floating medium or low signal inside.
Finally both the hematoma should be discarded as biloma that are usually associated with a history of trauma or iatrogenic following surgery and rarely spontaneous,
showing in the first heterogeneous density on CT according to the state of evolution of the lesion and hyperintense on being weighted sequences T1-weighted MRI of the paramagnetic effect of methemoglobin while biloma usually no septa or calcifications
Importantly,
the definitive treatment is surgical CAB either deferred or priority because of symptoms referred to the mass effect,
performing cystectomy,
but requires strict control image due to its high rate of recurrence and malignant transformation to cystadenocarcinoma why the definitive diagnosis which is based on pathological study.