A bursa is a fluid-filled sac lined with synovial cells that provide cushioning between bony prominences and the surrounding soft tissues,
in order to reduce friction between moving structures.
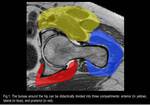
Several bursae are located around the hip and we didactically divided them into three groups: anterior compartment (iliopsoas bursa),
lateral compartment (subgluteus maximus,
subgluteus medius,
piriformis,
subgluteus minimus and gluteofemoral bursae),
and posterior compartment (obturator externus,
obturator internus and ischial bursae).
(Fig.1)
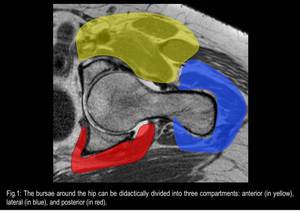
Fig. 1
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
We also illustrate many conditions that simulate bursitis such as peritendinitis,
tendon rupture,
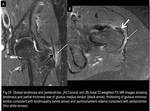
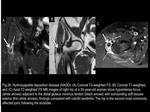
hydroxyapatite deposition disease,
ganglion and paralabral cysts,
tears involving the iliotibial band,
Morel-Lavallée lesion,
and ischiofemoral impingement with adventitous bursa.
ANTERIOR COMPARTMENT
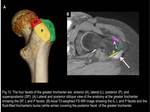
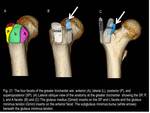
1) The Iliopsoas (or Iliopectineal) bursa
It is the largest bursa in the human body,
presenting in 98% of individuals.
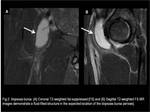
It is situated beneath the musculotendinous portion of the iliopsoas,
bordered medially by the pectineus muscle and laterally by the anterior inferior iliac spine.
(Fig.2 and 3)
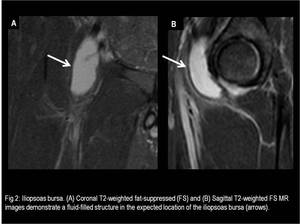
Fig. 2
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
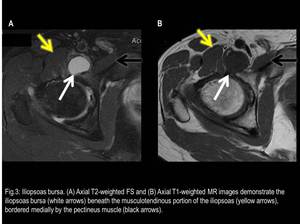
Fig. 3
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
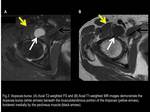
The Iliopsoas bursa lies anterior to the hip joint,
with which it communicates in 15% of normal asymptomatic individuals by way of a defect between the pubofemoral and iliofemoral ligaments.
(Fig.
4)
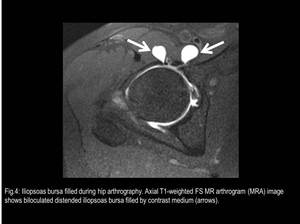
Fig. 4
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
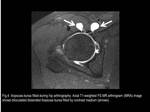
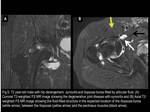
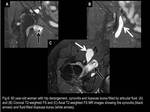
The incidence of this communication,
and thus bursitis,
is higher in the setting of hip derangement,
and is usually secondary to synovitis and/or increased intra-articular pressures,
which ultimately result in capsular thinning.
(Fig.
5 and 6)
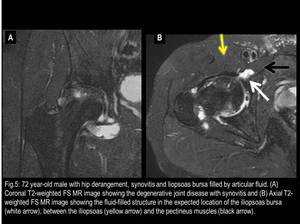
Fig. 5
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
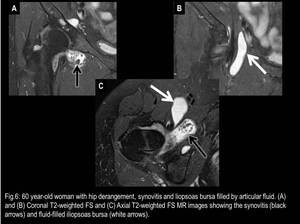
Fig. 6
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
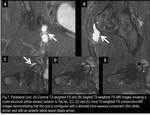
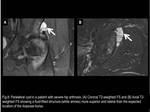
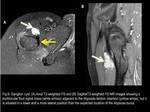
The differential diagnoses of the iliopsoas bursa include paralabral cyst (Fig.7 and 8),
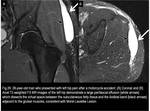
ganglion cyst (Fig.9) and iliopsoas musculotendinous strain or rupture (Fig.10 and 11).
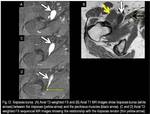
The correct diagnosis of an iliopsoas bursitis is made by following the fluid-filled structure on successive axial images,
recognizing that it is contiguous with the iliopsoas tendon (Fig.
12).
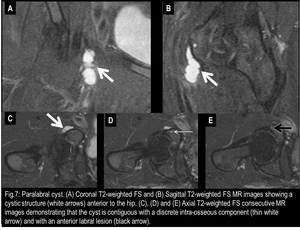
Fig. 7
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
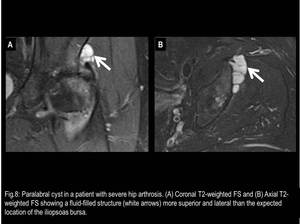
Fig. 8
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
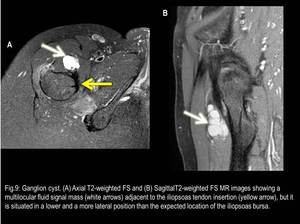
Fig. 9
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
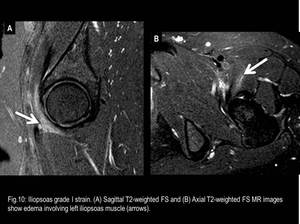
Fig. 10
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
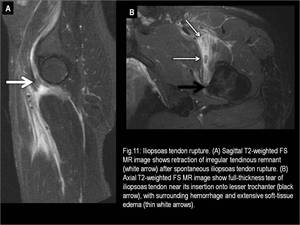
Fig. 11
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
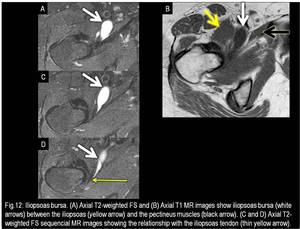
Fig. 12
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
LATERAL COMPARTMENT
Although pain over the lateral aspect of the hip has been commonly attributed to a trochanteric bursitis,
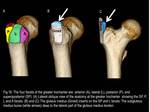
multiple bursae are associated with the greater trochanter (GT).
An understanding of the anatomy of the four facets of the greater trochanter is essential because each facet has specific tendinous attachments and specific nearby bursae.
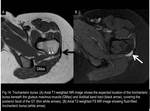
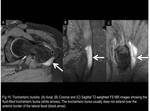
1) Trochanteric (or Subgluteus Maximus) Bursa
It covers the posterior facet of the GT (Fig.13) and it is located beneath the gluteus maximus muscle and iliotibial tract.
This bursa can be identified on axial MR images as an elongated structure paralleling the posterior facet and usually it does not extend over the anterior border of the lateral facet.
(Fig.14 and 15)
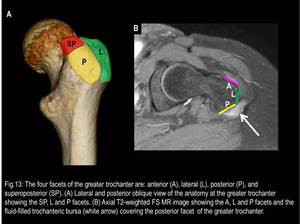
Fig. 13
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
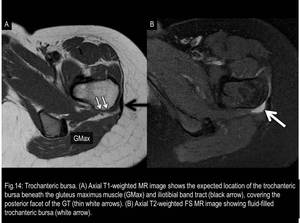
Fig. 14
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
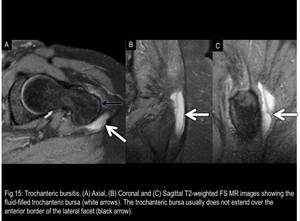
Fig. 15
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
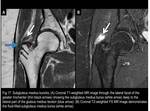
2) Subgluteus Medius (or Anterior Subgluteus Medius) Bursa
It is situated anterior to the apex of the GT (Fig.16),
deep to the lateral part of the gluteus medius tendon,
and proximal to its insertion,
covering an area of the superior part of the lateral facet of the GT.
(Figs.17 to 20)
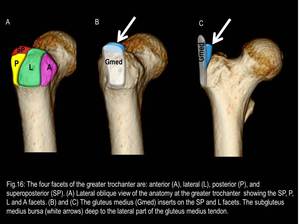
Fig. 16
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
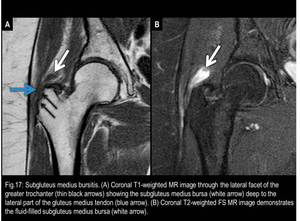
Fig. 17
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
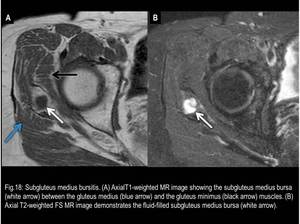
Fig. 18
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
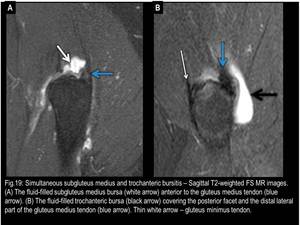
Fig. 19
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
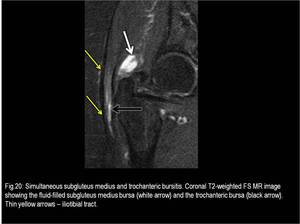
Fig. 20
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
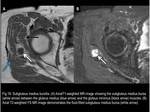
3) Subgluteus Minimus Bursa
It lies beneath the gluteus minimus tendon,
medial to its insertion,
in the area of the anterior facet of the GT.
(Fig.21 and 22)
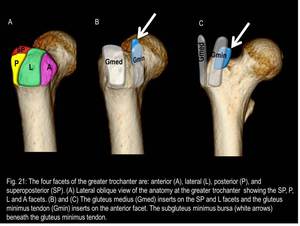
Fig. 21
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
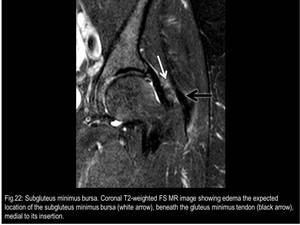
Fig. 22
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
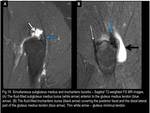
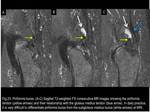
4) Piriformis (or Posterior Subgluteus Medius) Bursa
It is situated posterior to the apex of the GT.
The bursa lies on and follows the contour of the insertion of the piriformis tendon.
Its superficial surface is in contact with,
and often adhered to,
the deep surface of the gluteus medius tendon.
In daily practice,
it is very difficult to differentiate it from the anterior subgluteus medius bursa at MRI.
(Fig.23)
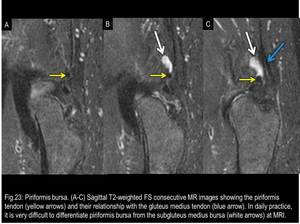
Fig. 23
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
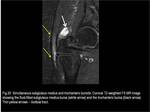
5) Gluteofemoral Bursa
It is situated caudal to the GT and it lies beneath,
and adhered to,
the iliotibial band in the area where the tendinous fibers of gluteus maximus inserts.
It is positioned over the posterior edge of the vastus lateralis,
separating it from the iliotibial band.
(Fig.24)
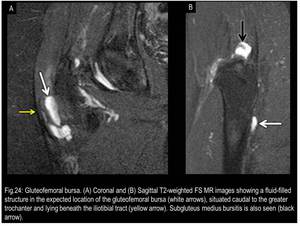
Fig. 24
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
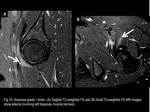
The differential diagnoses of lateral compartment bursae include gluteal tendinosis and peritendinitis (Fig.25),
hydroxyapatite deposition disease - HADD (Fig.26),
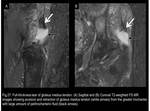
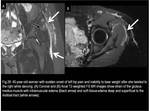
gluteal tendon rupture (Fig.27),
tears involving the iliotibial band (Fig.28),
and Morel-Lavallée lesion (Fig.29).
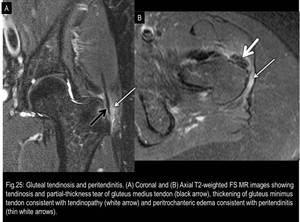
Fig. 25
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
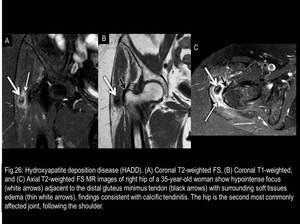
Fig. 26
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
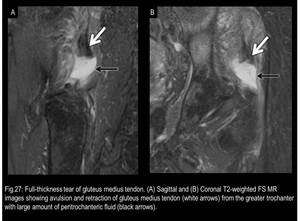
Fig. 27
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
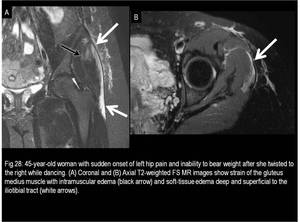
Fig. 28
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
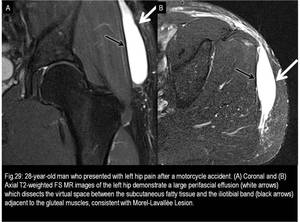
Fig. 29
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
POSTERIOR COMPARTMENT
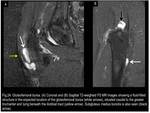
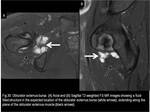
1) Obturator Externus Bursa
This bursa is thought to be formed by a protrusion of the posterior inferior hip synovium between the ischiofemoral ligament and the zona orbicularis.
It usually occurs in patients with hip synovitis and chronically increased intra-articular pressure.
When distended,
this bursa displaces the obturator externus muscle inferiorly while extending medially toward the obturator foramen.
(Fig.30)
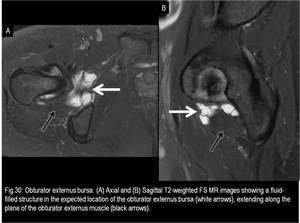
Fig. 30
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
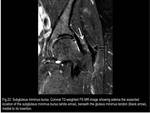
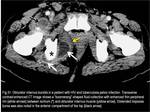
2) Obturador Internus Bursa
It is a “boomerang”-shaped fluid distension between the obturator internus tendon and the posterior grooved surface of the ischium.
Normally,
the obturator internus bursa is in a collapsed state,
and is only distended when it is inflamed or infected.
The majority of patients with obturator internus bursitis have been reported to respond adequately to antibiotics without surgical drainage.
Thus,
knowledge of the imaging features of obturator internus bursitis can avoid unnecessary surgery.
(Fig.31)
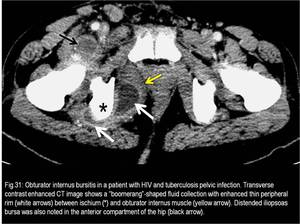
Fig. 31
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
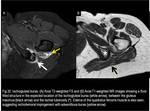
3) Ischial (or Ischiogluteal) Bursa
It separates the gluteus maximus from the ischial tuberosity.
Ischiogluteus bursitis is usually related to intermittent pressure upon the ischial tuberosity from prolonged sitting.
Tuberculosis,
gout,
rheumatoid arthritis,
systemic lupus erythematosus,
ankylosing spondylitis and Reiter’s syndrome have also been reported to involve the ischiogluteal bursa.
As the bursa lies in close contact to the sciatic and posterior femoral cutaneous nerve,
ischiogluteal bursitis can mimic the symptoms of radiculopathy.
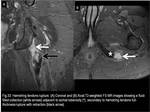
It may have a very heterogeneous appearance on imaging studies,
usually related to bleeding with blood-fluid levels,
synovial proliferation and internal septation.
(Fig.32)
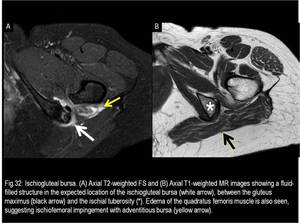
Fig. 32
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil
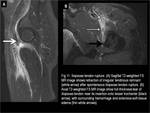
The differential diagnoses of posterior compartment bursae include hamstring tendinopathy/peritendinitis and/or rupture (Fig.33),
ischiofemoral impingement with adventitous bursa,
and ganglion cysts.
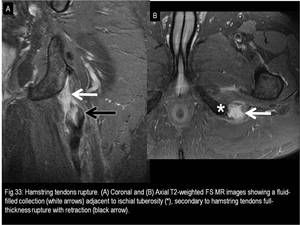
Fig. 33
References: Fleury Medicina e Saúde - Rio de Janeiro/Brazil