A 97 year old female patient visited our University Hospital due to regurgitation,
epigastric pain and progressive dysphagia when eating solids lasting 24 months before hospitalization.
She presented a lump sensation in the throat,
mild oropharyngeal and suprasternal dysphagia for several months,
globus sensation,
heartburn,
nighttime coughing and hoarseness,
attributable to the diverticulum; history of aspiration pneumonia,
no weight loss and she was nonsmoker.
According to her anamnesis,
she was taking Captopril + Hydrochlorothiazide because she had hypertension for about 10 years; she was taking Rabeprazole Sodium (the patient suffered from gastroesophageal reflux disease,
possible complicity causing the diverticulum) and taking Brimonidine Tartrate for cure a transitive ocular hypertension.
A clinical examination of the head and neck was unremarkable.
Evaluation of otorhinolaryngologist noted that the patient complained fetid halitosis,
regurgitation with rumination in hypopharynx and dysphagia for solids; laryngoscopy didn’t show anything abnormal except for the presence of mucous exudate level of the arytenoids.
Afterwards,
during the hospitalization,
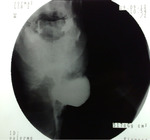
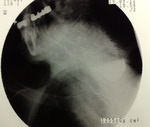
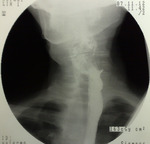
barium-swallow-pharyngoesophagraphy was performed with the patient in the erect position,
revealed a 5 cm left-sided KJD with a wide neck (Figure 1 and 2),
protruding through a muscular gap in the antero-lateral wall of the proximal esophagus,
on the lateral pharyngoesophageal junction area,
with smoothly marginated round-to-ovoid sacs.
The diverticulum opening was broader during swallowing than either before or after swallowing; was not revealed simultaneous presence of ZD,
reflux of barium from the diverticulum into the hypopharynx or overflow aspiration; therefore,
our patient had normal pharyngeal motility (except for incomplete opening of the cricopharyngeus).
An esophagogastroduodenoscopy was performed to confirm the suspected diagnosis and viewing the location of the opening of the diverticulum in relation to the cricopharyngeal muscle.
Sonographic examination demonstrated a heterogeneous,
hyperechoic smooth wall with hypoechoic crouched lumen involving the anterolateral wall of the cervical esophagus; the lesion appeared to arise in continuity with the esophagus.
Intra-hospitalization specialist cardiology control,
noted good hemodynamic compensation,
sinus rhythm with right bundle branch block with PR interval 200 ms,
normal for the age of our patient.
After consultation with the patient,
she received surgical treatment for esophageal diverticulum under general anesthesia.
The left side location of the diverticulum on the esophagogram,
has led us to decide a left cervical approach for surgeon’s convenience.
The diverticulum was approached through an oblique incision along the anterior border of the left sternocleidomastoid muscle with the patient’s head extended and slightly turned to the right.
After medialization of the thyroid gland,
saving recurrent laryngeal nerveand lateralization of the omohyoid muscle,
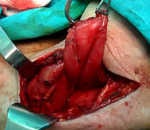
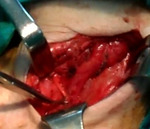
diverticulum was visualized to its emergence in the Killian-Jamieson space (Figure 3).
Diverticulum (5 × 5 cm sized) was found with a wide base and adhered to circumjacent tissues; in particular,
it strongly adhered to the prevertebral fascia in the rear of the trachea.
Cervical esophagus proximal to the diverticulum was dissected cautiously and the diverticulum was dissected from adjacent tissues (following isolation of the left recurrent laryngeal nerve and carotid artery lateralization).
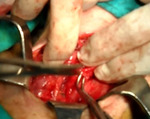
Antigravity diverticulopexy along the prevertebral band with three prolene® zero points and myotomy of the cricopharyngeal muscle extramucosal of about 3 cm along the cervical esophagus was conducted (Figure 4 and 5).
The esophageal patency was evaluated through the introduction of nasogastric tube.
Surgical suture closed the breach.
The surgery was completed without the insertion of a drainage tube.
The patient was started on a clear fluid diet postoperative (day 1) and advanced to a soft diet on day 3.
The patient was discharged from our University Hospital 6 days after the surgery procedure without complications such as nerve damage or hemorrhage.
The Rx pharyngoesophagraphy on the twenty day after the surgery showed that there were not abnormalities such as leakage or stenosis (Figure 6).
Follow-up observation has been performed for 3 months,
during which the patient has not shown any abnormalities such as diverticulum relapse,
dysphagia,
regurgitation,
nighttime cough or stenosis.
A follow up esophagoscopy was performed at three months after the procedure; it revealed a wide communication between the diverticular sac and the esophageal lumen without a significant tissue bridge.