This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Multidisciplinary cancer care, Cirrhosis, Cancer, Treatment effects, Education, Ablation procedures, Ultrasound, Percutaneous, CT, Management, Liver, Abdomen
Authors:
S. W. Jeon, J. H. Kwon, M. J. Kim; Daegu/KR
DOI:
10.1594/ecr2014/C-0747
Background
1.
Understanding and rationale of combination therapy for treatment of HCC
Liver cancer is the fifth most common cancer in the world and its incidence is increasing worldwide.
But only about 30% of patients can benefit from curative therapies such as resection or liver transplantation due to poor liver function,
as well as multiplicity of tumors.
Therefore,
non-surgical locoregional therapies have been used worldwide,
such as transcatheter arterial chemoembolization(TACE), percutaneous ethanol injection(PEI) and radiofrequency ablation(RFA).
They are minimally invasive options that can achieve the successful tumor eradication and preservation of liver function.
Recent evidence suggests that combination therapy has a synergistic effect in treating hepatocellular carcinoma(HCC),
especially for: (1) larger lesions that do not respond adequately to either procedure alone; (2) tumor at risky location or difficult to be treated by either procedure alone.
2.
Principle,
technique,
advantage and disadvantage of each monotherapy
2.1.
TACE(transcatheter arterial chemoembolization)
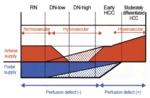
- Principle and technique: Usually the normal liver parenchyma has dual blood supply from the portal vein and hepatic artery.
Two-third from portal vein and one-third from hepatic artery.
But during hepatocarcinogenesis,
most HCC show a deterioration of arterial blood flow and are eventually fed mainly by arterial flow(Fig.
1).
So TACE exploits hepatic artery to deliver chemotherapic agent such as 5-fluorouracil,
mitomycin C,
doxorubicin,
or cisplantin without damaging the normal liver parenchyma.
TACE is based on the synergistic effect of arterial occlusion and local chemotherapy by using microcatheter technology.
The purpose of embolization is to prevent the washout of the chemotherapic agent at the site of tumor and to induce ischemic necrosis.
Well knowned embolic materials for occlusion of the hepatic artery are metallic coils,
Gelfoam,
lipiodol,
polyvinyl alcohol,
starch microspheres,
or collagen particles.
- Advantage: Can make selective arterial occlusion which induces ischemic tumor necrosis while minimizing damage to the liver tissue with preserved liver function.
- Disadvantage: Can not be done for patients with severely compromised liver function,
such as: (1) Child-Pugh classification C or late B; (2) massive HCC or HCC involving major portal veins coexistence of inferior vena cava thrombosis (IVTT) and/or portal vein tumor thrombosis (PVTT).
In these situations,
TACE shows a high risk of ischemic liver insufficiency or a lack of efficacy.
2.2.
PEI(percutaneous ethanol injection)
- Principle and technique: Most HCCs arise in a background of cirrhosis caused by hepatitis virus or alcohol.
The patients with underlying cirrhotic liver need percutaneous ablation because of minimal invasiveness and ready reproducibility.
The principle of PEI is percutaneous injection of absolute ethanol (99.9%) into HCC for making tumor necrosis.
Needle targeting into tumor is performed by ultrasonography or CT-guidance.
- Advantage: Can be performed in any portion of the liver because of less invasive rather than RFA.
The effect of PEI reveal nearly equal result of 5-year survival rates compared with surgical resection for small (<3cm) HCC.
In patients with large HCC,
high-dose PEI would be a valid alternative for volume debulking.
- Disadvantage: Incomplete necrosis is more frequent than RFA because diffusion of ethanol is affected by the capsule or septa of HCC that can make uneven and imcomplete necrosis.
2.3.
RFA(radiofrequency ablation)
- Principle and technique: The principle of RFA is percutaneous insertion of electrode into HCC which can produce heat for thermal cytotoxicity and tumor necrosis. Use of electrical currents in the radiofrequency range to make heat. Most HCCs arise in a cirrhotic liver and often is surrounded by a capsule.
The tumor capsule functions as thermal insulators like oven,
resulting in higher peak temperatures and more effective ablation,
so-called oven effect.
Electrode targeting into tumor is performed by ultrasonography or CT-guidance.
- Advantage: Complete necrosis is more frequent with fewer treatment sessions rather than PEI because heat effect distributes homogeneously in all directions and are less affected by intratumoral septa than PEI.
So RFA can makes better overall survival and disease-free survival rate with lower local recurrence rate.