Image acquisition protocols:
Routine head CT often requires additional spiral aquisitions in trauma,
or when angio-CT is employed (detection of cerebral aneurysms or vascular malformations).
- Recommended acquisition parameters for routine head CT on a Siemens Somatom 16: sequential (axial) scan: 120 kV,
effective mAs 400,
rotation time = 1s,
detector acqusition/collimation : 8x1,2,
slice thickness 4,8 mm (recon: 2,4 mm),
Kernel H31s.
- Spiral (helical) scan using fine detectors (16x0.6),
rotation time = 1s,
pitch = 0.85 slice thickness up to 1 mm for trauma/Angio-CT
The routine MRI protocol for the brain includes,
on a GE Signa 1.5 T machine:
- Axial T2,
Ax/Cor FLAIR,
Axial T1 SE,
3D T1 FSPGR,
DWI
- Selected cases benefit from SWI,
T2 gradient recalled echo sequences,
arterial and/or venous MRA (3D TOF/2D TOF),
and if necesary,
gadolinium administration.
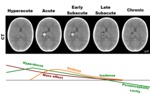
CT appearance of bleeding (Fig. 6):
–Hyperacute: extravasated blood has a slightly heterogeneous appearance with specific densities between 45-60 HU (similar to normal cerebral parenchyme areas)
–Acute and early subacute: blood clot retraction with increased density of the accumulation (80 HU) surrounded by an area of edema
–Late subacute: hematoma is isodense to normal cerebral parenchyme areas
–Chronic: hypodense appearance as the hematoma is progressively resorbed,
and can associate atrophy of surrounding parenchyme and ventriculomegaly
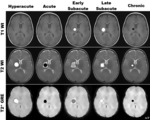
MRI appearance of bleeding (Fig. 7) :
–Hyperacute: long T1 and T2 relaxation times: hypo-/ or isointense on T1-weigthed images and high signal intensity on T2-weighted images = protein containing fluid [6]
–Acute: preferential T2 proton relaxation enhancement shortens T2 but not T1: slightly hypo-/ or isointense on T1-weigthed images and low signal intensity on T2-weighted images (Fig. 8)
–Early subacute: proton-electron dipole-dipole interaction shortens T1 as well as T2; accentuated T2 relaxation (T2 proton relaxation enhancement) leading to high signal intensity on T1-weigthed images and low signal intensity on T2-weighted images (Fig. 9)
–Late subacute: loss of T2 proton relaxation enhancement; proton-electron dipole-dipole relaxation enhancement leading to a decrease of T1.
Remaining high signal intensity on T1-weigthed images .
T2 shortening leading to high signal on T2-weighted images = protein containing fluid (Fig. 10)
–Chronic: no dipole-dipole interaction occurs; hemosiderin is slightly hypointense on T1-weigthed images,
and very hypointense on T2-weighted images,
especially due to the inhomogenous distribution which leads to T2 proton relaxation enhancement. (Fig. 11)
Compartments of intracranial bleeding (Fig. 12) :
The location of the bleeding is important,
as it brings information relevent for the cause of the hemorrhage,
as follows:
A.
Intraaxial (=Intraparenchymal) hemorrhage occurs most frequently dur to hypertensive damage to blood vessel walls (hypertension,
eclampsia,
drug abuse),
altered hemostasis,
hemorrhagic transformation or other. (Fig. 2)
B.
Extraaxial:
- Subdural or epidural - Subdural hematomas occur between the skull and the outer endosteal layer of the dura mater,
involve meningeal or ethmoidal arteries or venous sinuses and have a typical biconvex lens appearance (Fig. 13). Epidural hematomas occur between the dura and the arachnoid,
involve bridging veins and have a typical crescent shape appearance (Fig. 14).
- Subarachnoid - occurs most commonly in head trauma; non-traumatic appears in the setting of a ruptured cerebral aneurysm or arteriovenous malformation (AVM) (Fig. 15).
- Intraventricular - is uncommon without parenchymal involvement; primary intraventricular hemorrhage has been noted in hypertension,
anterior comunicating artery aneurysm,
anticoagulation,
moyamoya disease and intraventricular neoplasia (Fig. 16).
What is important to report?
- Location and etiology of the hemorrhagic lesion
- Signes of gravity: mass effect,
hydrocephaly
- Prognostic-evolution in time

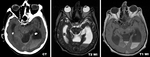
![Fig. 9: Early subacute stage hematoma. CT demonstrates right cerebellar hemisphere hematoma with surrounding oedema. Relative hyperintensity on T1 WI appears due to the oxydation of deoxyhemoglobin to methemoglobin. DWI shows decreased signal intensity which also translates to the ADC map (T2 “dark-through”) caused by low signal on the T2 images, a feature of the acute and earlysubacute hemorrhages [9].](https://epos.myesr.org/posterimage/esr/ecr2014/119782/media/530768?maxheight=150&maxwidth=150)
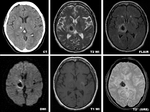
![Fig. 10: Late subacute stage hematoma. CT shows isodense lesion in the left lenticular-insular region, with fine hyperdense rim on the anterior side. MRI shows hyperintensity on the T2 WI caused by loss of susceptibility effect due to degradation of the red cell membranes. Note that the degree of vasogenic oedema is lesser compared to the earlier phases. Restricted diffusion on the DWI, typical of hyperacute and late subacute hemorrhages [9].](https://epos.myesr.org/posterimage/esr/ecr2014/119782/media/530769?maxheight=150&maxwidth=150)

![Fig. 12: Frequency of bleeding sites in the brain (adaptation after Scarabino T et al. Emergency Neuroradiology, Springer 2006 [8]).](https://epos.myesr.org/posterimage/esr/ecr2014/119782/media/530588?maxheight=150&maxwidth=150)