This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Trauma, Speech disorders, Education, Decision analysis, CT, Thyroid / Parathyroids, Head and neck
Authors:
J. A. Sheehan, K. Davies, P. Gormley, P. McCarthy; Galway/IE
DOI:
10.1594/ecr2014/C-1698
Findings and procedure details
The three patient's in our series all presented to the emergency room following direct trauma to the neck region and complaining of related symptoms such as: hoarseness,
dyspnoea,
dysphonia,
aphonia,
dysphagia,
odynophagia,
or odynophonia.
On physical examination,
the most common signs related to laryngeal trauma include pain on palpation,
haemoptysis,
subcutaneous emphysema or stridor[3].
In the emergency department,
Advanced Trauma Life Support(ATLS) protocol dictates securing the airway.
This step is specifically important in the setting of suspected laryngeal trauma.
Once immediate life-threatening injuries have been corrected,
a cervical spine x-ray should be cleared as 9% of all cervical spine fractures have associated laryngeal fractures[2].
A normal cervical spine x-ray,
with a patient complaining of one or more of the symptoms or signs above,
should direct the clinician to order a CT scan of the neck and perform a transnasal fiberoptic laryngoscopy.
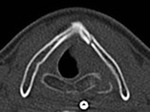
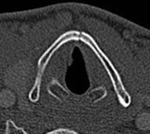
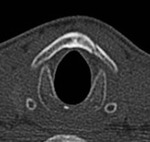
One of the patient's in our series (Figure 1),
had ongoing stridor after blunt trauma to the neck.
The patient underwent a transnasal fiberoptic laryngoscopy that revealed a haematoma and an underlying fracture was confirmed on CT neck.
In this case,
CT imaging was necessary to further assess neck anatomy and to determine the extent of injury.
Appropriate use of CT imaging in this way,
when correlated with signs and symptoms,
is cost effective and can avoid the need for further surgical intervention[4].