For optimal images 5-10 MHz linear-array transducers are used in neonates and infants and for children and adolescents 2-4/ 4-7 MHz convex or linear-array transducers may be required.
The pacient is held in decubitus,
supine or prone position.
The approaches used for scanning of the lung,
pleura and anterior mediastinum are transternal,
parasternal and intercoastal whereas for lung apices and the upper mediastinum suprasternal and supraclavicular approaches are better.
For juxtaphrenic paravertebral lesions,
subxyphoid and transdiaphragmatic approaches are used with the liver as an acoustic window.
The images obtained are in transverse,
longitudinal,
inclined transverse or inclined-longitudinal (14).
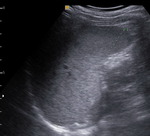
In order to depict and corectly identify pathological aspects of lung and pleura we need a good knowledge of the normal appearances (Fig 1).
It is important to know that all signs of lung ultrasound arise from the pleural line.
Knowing this,
the signs that appear in normal lungs (without pathology) are:
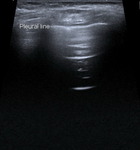
The bat sign - one of the most important signs in lung ultrasound (3).
The probe is placed longitudinally over an intercostal space and the image depicted consists of the superior and inferiors ribs, their acoustic shades (the wings of the bat) and the pleural line (and the lung underneath - the body of the bat) (Fig 2).
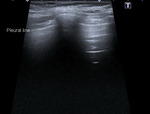
A lines - These are the hyperechoic lines parallel with the pleural line,
demostrating the air in the lungs.
The distance between the A lines is constant and equals the distance between the pleural line and the thoracic wall.
It is important to know that A lines appear in normal aerated parenchyma (where they are associated with lung sliding) but also in pneumothorax (where lung sliding is absent) (Fig 3).
The seashore sign or lung sliding - it represents the sliding movement of the lung against the thoracic wall,
a movement that is in accordance with respiration and is minimal at the apices and increases at the bases of the lungs.
This sign can be better depicted and quantified with M-mode.
The signs that appear in pathological lungs are:
The B lines - these lines constitue of an artifact that has 7 characteristics (2): they are hydroaeric comet-tail artifacts,
they arise from the pleural line,
they are hyperechoic,
well defined,
spreading up indefinetely (uninterrupted to the edge of the screen),
they erase the A lines and they move with lung sliding.
The B lines appear when there are simoultaneously elements with great acoustic impedance gradient like fluid and air (2) (i.e.
alveolar-interstitial syndrome).
Three or more B lines seen in a single view are called B+ lines or lung rockets (3,
4) (Fig 5).
Stratosphere sign - this sign indicates the absence of the lung sliding and it is consistent with pneumothorax.
The lung sliding sign is replaced by parallel horizontal lines above and beyond the pleural line and this means the absence of structures at these levels.
Lung point - this sign appears at the transition between normal and pathological pulmonary parenchyma and represents the alternation normal/ pathological parenchyma during respiration.
Lung pulse - means the pulsation of the lung with the heartbeat in complete atelectasis.
Alveolar consolidation - this appearance is made by a “parenchymal” structure when alveoli are filled with fluid (given by the reflections of the interfaces between alveoli and interstitial spaces) that looks like the parenchyma of the liver or spleen.
The structure’s borders are smooth near the pleural line and irregular in the deeper parenchyma,
where the consolidated area is near normal aerated parenchyma.
Air bronchogram - consists with either straight or irregullar hyperecoic lines which only appear in a consolidated areas.
This sign is very important because it helps differentiate pneumonia from atelectasis.
All these normal and pathological signs described above concur to help diagnose and differentiate between various diseases of the lung and pleura.
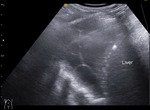
Pleural effusion
Is very easily recognisable on ultrasound like any other fluid collection as being an anechoic image between the visceral and the parietal pleura.
It is also easy to drain these collections when using ultrasound guided needles.
A pleural effusion can be either free in the pleural cavity or secluded.
The collection can be clear or with fibrin strands (atached to one pleural surface - floating,
atached to both pleural surfaces – loculated,
or as a halo of fibrin - thickening the pleural surface).
It is important to know that a large quantity of pleural effusion is accompanied by pressor atelectasis (5).
By using thoracic ultrasound we can detect and quantify smaller sized pleural effusions than on plain X-ray.
(6).
Even if it is not always of great importance to detect the quantity of pleural fluid,
most of the times it is useful in determining the etiology (7),
prognosis (8) and even in guiding the treatment (9) (Fig 4,
Fig 5).
Empyema - a secluded pleural effusion with thick walls and with or without air inside it (Fig 6,
Fig 7).
Pleural tumors - primar pleural tumors are extremely rare in children.
Most frequently pleural tumors encountered are metastases.
The ultrasonographic characteristics are: echoic structures,
well vascularized (using Doppler),
most of the times they are associated with pleural effusion and do not shift with the lung parenchyma during respiration .
The role of ultrasound in diagnosing pleural tumors is not to differentiate between benign and malignant tumors but to localize and guide for percutaneous biopsy (10) (Fig 8).
Pneumothorax - is the filling of the pleural cavity with air usually associated with the compression of the underlying lung parenchyma.
The signs appearing in this situation are a combination of A-lines,
the abscence of lung sliding/presence of lung sliding in the same area - the lung point (11).
Pneumonia – in this disease the appearance is the one of alveolar consolidation.
It is important to realise that by the means of ultrasound we can only depict consolidation areas that are either of a superficial location or close to the diaphragm.
Also air bronchogram and B lines appear in pneumonia.
Lung sliding is abolished,
which can be explained by the inflamatory adherences due to exudate (2) (Fig 9).
Atelectasis - lung pulse appears in complete atelectasis.
Atelectasis is associated with the changing in the imaging location of the heart,
diaphragm,
the presence of at least 250 ml of pleural effusion,
the abolition of the movement of the diaphragm (3,
12,
13) (Fig 10).
Tumors/metastases of the lungs - have mainly the same features as pleural tumors,
except that they do shift with the lung during respiration.
Ultrasound can reveal tumours that reach the pleura (Fig 11).
Pulmonary abcess - Hypoechoic,
fluid collection (looking ”dirty” with the presence of echogenic detritus and maybe gas inside it) usually localized inside an area of pulmonary consolidation (Fig 12,
Fig 13).
Mediastinal tumors - need to be differentiated from the normal thymus.
Parenchymatous structure which can be seen through the heart or diaphragmatic window usually when they reach a certain size (Fig 14,
Fig 15,
Fig 16).