Study population
The institutional review board approved this retrospective study,
and the requirement to obtain informed consent was waived.
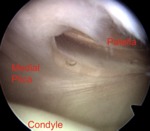
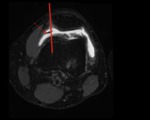
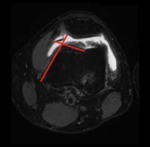
19 teenagers suspect of medial plica syndrome underwent MRI of the knee and arthroscopy,
which confirmed a pathologic medial plica (Sakakibara C or D) with resection of this plica (Fig.
2).
We established a control group with 25 patients who underwent knee MRI and arthroscopy for another reason,
without medial plica identified.
All the arthroscopy have been performed at Amiens University Medical Center by pediatric surgeons,
between August 2005 and June 2013.
Images Analysis
We reviewed the MRI,
blinded to clinical data.
Only axial T2 Fat-Sat weighted images of the femoro patellar joint were analysed in order not to be influenced by a knee pathology in the control group.
Images acquisition was not the same for all the patients because it was preoperatively obtained from different MRI scanner,
not exclusively at Amiens University Medical Center.
Images with Cube DP Fat-Sat acquisition were remodelled by a third party to obtain axial slices on the femoro-patellar joint.
The review was done on Advantages Windows console 4.6.
The criteria studied were: presence of the plica,
floating aspect,
interposition into the femoro-patellar joint,
number of slices with interposition,
height of the interposition,
total length and length after the interposition line,
length of the floating part,
thickness,
high signal in T2 FatSat weighted image,
contact with femoral or trochlear cartilage,
focal femoral or trochlear chondromalacia (on the medial facet),
focal or diffuse synovitis,
intra articular effusion,
and fenestrated aspect.
We practiced a « learning session » on random knee MRI for evaluating this criteria.
Usually for radiologists,
a medial plica exists when there is a linear structure floating at the expected location.
During our learning session,
this finding was rare.
Thus,
in order to be coherent with the epidemiological data available in the literature,
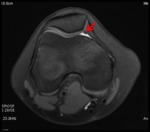
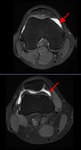
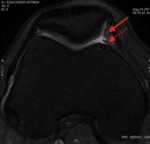
we considered a medial plica present when we found a linear structure floating but also when there was a thickening or a bulge of the joint capsule back the retro patellar fat pad,
supposing that this thickening is composite of the joint capsule and the medial plica collapsed against the capsule (Fig.
3 and 4).
The medial plica was considered floating when we could individualize a linear band with local effusion (Fig.
5).
The interposition was defined as a medial plica crossing the interposition line (Fig.
6).
The interposition line was defined as a line extended between the medial tip of the patella and the point X.
This point X was variable on each slice,
and was defined as the intersection of the tangents of the medial condylar facet and the medial trochlear facet (Fig.
7).
Height of the interposition was automatically calculated from the slice thickness and the gap value of the acquisition.
Thickness of the plica was graded in 4 levels: grade 0 was absence of plica,
grade 1 less than 1 mm,
grade 2 less than 2 mm,
grade 3 less than 3 mm.
Intra-articular effusion was also graded in 4 levels: grade 0 was no effusion or physiological effusion,
grade 1 small effusion,
grade 2 intermediary effusion and grade 3 important effusion.
The plica was considered fenestrated when there had fluid inside making a windows.
Statistical Analysis
The distribution of patients according to gender was compared with that of control group by using Fisher exact test.
The age of patients was compared with the control group distribution by using the Mann-Whitney U test.
We used non-parametric statistical tests with a significance level for p-value <0,05: Fischer test for qualitative criteria,
Mann-Whitney test for quantitative criteria.
A p-value less than 0,05 was considered to indicate a significant difference.
XLStat software (version 2013.4.05) with Microsoft Excel (for Mac 2011 version 14.2.0) was used.