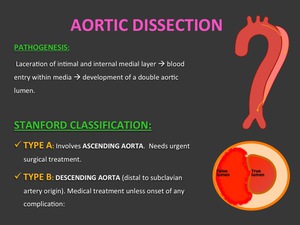
Fig. 1: Aortic dissection: Pathogenesis and Stanford classification
1.
AORTIC DISSECTION
Most frequent cause of aortic emergency.
High mortality without urgent treatment.
CT has high sensibility and specifity,
nearly 100%.
RISK FACTORS: Hypertension,
Marfan syndrome,
Ehler-Danlos syndrome,
Turner syndrome,
medial cyst necrosis.
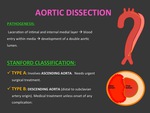
PATHOGENESIS: Laceration of intimal and internal medial layer that leads to blood entry within media through intimal tear and subsequent development of a double aortic lumen.
CLASSIFICATION: According to Stanford classification:
- TYPE A: Involves ascending aorta. Needs urgent surgical treatment.
- TYPE B: Descending aorta (distal to subclavian artery origin).
Medically treated (antihypertensive medication) unless onset of any complication:
- Aortic rupture
- Hemodynamic inestability
- Descending aorta >6cm
- Diminished abdominal perfusion (aortic branches involvement)
- Distal Embolization
- Pseudocoarctation syndrome
X-RAY FINDINGS:
- No findings in 10-40%
- 60% mediastinal widening
- 25%abnormal cardiac silhuette
- 4% >1cm desplacement of aortic calcification
FINDINGS THAT MAY SUGGEST COMPLICATION: significant increased cardiopericardic silhouette (suggesting pericardic effusion) and new pleural effusion.
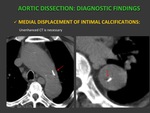
CT DIAGNOSTIC FEATURES:
a) MEDIAL DISPLACEMENT OF INTIMAL CALCIFICATIONS: Unenhanced CT is necessary to this evaluation.
Fig. 2
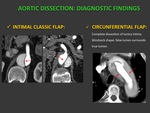
b) INTIMAL CLASSIC FLAP: aprox in 70% Fig. 3
c) CIRCUNFERENTIAL FLAP: Complete dissection of tunica intima,
has a windsock shape with the false lumen surrounding true lumen.
Fig. 3
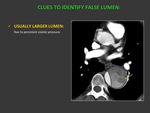
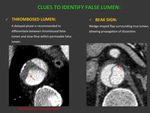
CLUES TO IDENTIFY THE FALSE LUMEN:
- It is usually the larger lumen due to persistent sistolic pressure Fig. 4
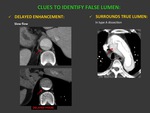
- Delayed enhancement because of slower flow Fig. 5
- Surrounds true lumen (circunferential flap) Fig. 5
- Beak sign: wedge shaped flap surrounding the true lumen,
which allows propagation of intimal dissection.
Fig. 6
- Cowbeb sign: intimal linear strands usually floating within false lumen
- Thrombosed false lumen: a delayed phase is recommended to differentiate between thrombosed false lumen and slow flow.
Fig. 6
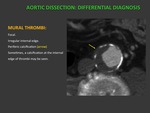
DIFFERENTIAL DIAGNOSIS:
a) INTRAMURAL HEMATOMA:
Difficult differential diagnosis with thrombosed dissection.
Spiral propagation and desplaced clacification are findings that suggest thrombosed false lumen
b) MURAL THROMBI: Fig. 7
Differential diagnosis with thrombosed dissection.
Focal.
Irregular internal edge (dissection usually presents with smooth edges).
Periferic calcification.
Sometimes,
a calcification at the internal edge of thrombi within an aneurysm may be seen:
- Aneurysmatic lumen is usually round shaped.
- True lumen in aortic dissection is usually flattened due to high pressure compression.
c) PENETRATING ATHEROSCLEROTIC ULCER:
No intimal flap.
Focal contrast leak without lumen compression
Severe calcified atheromatosis.
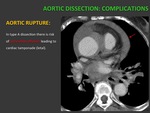
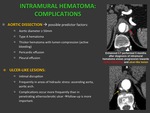
COMPLICATIONS:
a) AORTIC RUPTURE: High mortality.
Rupture is most frequently located at external wall of false lumen.
In type A dissection there is risk of pericardial effusion,
which may lead to cardiac tamponade (poor prognosis). Fig. 8
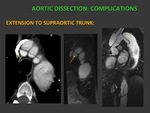
b) SUPRAORTIC TRUNK INVOLVEMENT: May lead to neurological symptoms,
poor outcome.
FFig. 9
c) CORONARY ARTERIES INVOLVEMENT: Requires emergent surgery
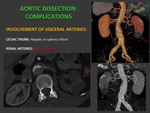
d) INVOLVEMENT OF VISCERAL ARTERIES: 27%.
Secundary alteration of abdominal perfusion.
- CELIAC TRUNK: splenic or hepatic infarction
- MESENTERIC ARTERIES: mesenteric ischemia.
- RENAL ARTERIES: renal ischemia. Fig. 10
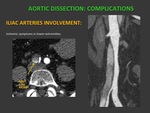
c) ILIAC ARTERIES INVOLVEMENT: Ischemic symptoms in lower extremities. Fig. 11
TECHNICAL CONSIDERATIONS:
- Always include in your CT protocol a unenhanced basal examination of thoracic aorta (thick slices).
- Use high rate injection allowing complete opacification of aorta.
- Injection of contrast material throug right arm circulation: prevents artefacts when imaging aortic arch.
- If percutaneous treatment is possible,
it is important to determine which femoral artery can provide access to true lumen.
- Examination should include the entire aorta:
- 3 cm above aortic arch to include supraaortic vessels.
- Iliac arteries
- EKG-gated CT decreases artefacts due to aortic pulsatile movement,
avoiding false positives.
- Ideal examination: should confirm or rule out the suspected diagnosis,
evaluate the complete lesion extension and identify eventual complications.
WHAT SHOULD BE INCLUDED IN THE RADIOLOGICAL REPORT?
- Type of dissecton: A or B
- Presence of intramural hematoma or penetrating ulcer.
- Involvement of ascending aorta.
- Entry and re-entry points of blood within false lumen.
- Involvement of aortic branches
- Involvement of coronary arteries
- Presence of thrombi or thrombosed false lumen.
- Complications: rupture,
aortic dilatation,
haemorrhage
- False and true lumen diameters at:
- Proximal and distal points to intimal rupture
- Shortest diameter
- Tortuosity of iliac vascularity
2.
INTRAMURAL HEMATOMA:
5-20% of acute aortic syndromes.
20% mortality rate.
PATHOGENESIS: Vasa vasorum haemorrhage within medial layer without intimal tear.
94% spontaneous in hypertensive patients.
May be traumatic.
CLASSIFICATION: Same as aortic dissection.
- TYPE A: Symptoms and risks similar to type A aortic dissection.
Less consensuated treatment: individual evaluation due to variable prognosis and high surgery morbimortality rate.
- TYPE B: medical treatment.
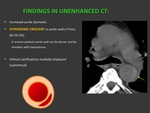
UNENHANCED CT FINDINGS: Fig. 12
- Increased aortic diameter.
- Crescent of high attenuation in aortic wall (>7mm,
60-70 UH).
- In anemic patients aortic wall can be denser and be mistaken with haematoma.
- Intimal curvilinear calcifications displaced towards internal lumen: because this hematoma is subintimal.
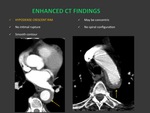
ENHANCED CT FINDINGS: Fig. 13
- Hypodense crescent rim,
smooth contour
- No intimal rupture
- No spiral configuration.
May be concentric.
COMPLICATIONS:
Variable natural history due to weakening of aortic wall.
May progress to:
- Complete resolution (even in 1 month)
- Ulcer-like laceration Fig. 14
- Aortic dissection Fig. 14
- Aneurysmatic dilatation: may evolve into aortic rupture
Complications may present at any stage,
even after hematoma disappears.
Long term follow-up is recommended to avoid fatalities.
a) Progression towards aortic dissection: possible predictor factors:
- Aortic diameter > 50mm
- Type A hematoma
- Thicker hematoma (active bleeding)
- Pericardic effusion
- Pleural effusion
b) Progression towards ulcer-like lesions: frequently in areas of hidraulic stress such as ascending aorta and aortic arch.
c) Progression towards aortic aneurysms: May occur years later,
even with resolved hematoma.
- Saccular
- Fusiform.
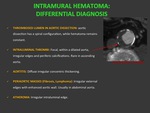
DIFFERENTIAL DIAGNOSIS: Fig. 15
a) THROMBOSED LUMEN IN AORTIC DISSECTION: aortic dissection has a spiral configuration,
while hematoma remains constant.
b) INTRALUMINAL THROMBI: Focal,
within a dilated aorta,
irregular edges and periferic calcifications.
Rare in ascending aorta. Fig. 15
c) AORTITIS: Diffuse irregular concentric thickening.
d) PERIAORTIC MASSES (Fibrosis,
Lymphoma): Irregular external edges with enhanced aortic wall.
Usually in abdominal aorta.
e) ATHEROMA: Irregular intraluminal edge.
TECHNICAL CONSIDERATIONS IN INTRAMURAL HEMATOMA:
It is very important to perform first an unenhanced CT to avoid missing an intramural hematoma in an acute aortic syndrome.
SHOULD BE INCLUDED IN THE RADIOLOGICAL REPORT:
- Maximum aortic diameter
- Maximum thickness of aortic hematoma: measured in axial plane.
- Origin and termination of intramural hematoma
- Transverse diameters (maximum and minimum) of aortic lumen at the level of thickest portion of hematoma.
- Involvement of any aortic branch
- Radiological follow-up is needed even if hematoma resolves or decreases because local complications may be seen later on time.
3.
PENETRATING ATHEROMATOUS ULCER:
Typically in elderly patients with severe atherosclerotic disease.
Frequently located in aortic arch and inferior half of descending thoracic aorta (faster flow in ascending aorta protects from atheromatosis).
Medical treatment if possible because surgical treatment is complex with higher morbility.
Diagnosis may be made only in SYMPTOMATIC patients: penetrating atheromatous ulcer is not a incidental finding.
PATHOGENESIS:
Ulceration of an atheromatous plaque with rupture of internal elastic laminae exposing tunica media to blood flow.
This leads to haemorrhage within aortic wall that originates an intramural hematoma. Fig. 16
COMPLICATIONS:
May occur in 1/3 of patients:
- Aortic rupture: higher risk than in aortic dissection is described in medical literature.
- Aortic dissection
- Pseudoaneurysm
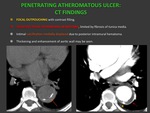
CT FINDINGS: Fig. 17
- Focal outpouching area with contrast filling.
- Adjacent focal intramural hematoma,
limited by fibrosis of tunica media.
- Intimal calcification internally displaced due to posterior intramural hematoma.
- Thickening and enhancement of aortic wall may be seen.
DIFFERENTIAL DIAGNOSIS:
a) NO PENETRATING ATHEROMATOUS ULCER:
- Patient is asymptomatic.
- No deep extension,
with irregular edges
- No contrast extravasation
- No associated intramural hematoma.