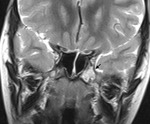
Arrested pneumatization is most frequently observed in relation to sphenoid sinus and is a developmental anomaly observable in normal and/or known accessory pneumatization areas.
It generally manifests itself in the basisphenoid bone and pterygoid process region (1,2),
petrous temporal apex and clivus were also reported areas (3,4).
In fact,
accessory pneumatization areas such as occipital and frontal bones,
as well as maxillary bone have also been defined (1,2).
Whereas in the ethmoid bone,
arrested pneumatization has not been defined likely due to its aeration mechanism (2).
In our cases,
lesions were defined in the sphenoid bone and sphenoid subsites (figure 3) as well as in the temporal bone petrous apexes.
While temporal bone petrous apex had been defined only in one case report previously (3),
with a lesion involving the sphenoid bone,
pterygoid process and petrous apex simultaneously.
Two of our cases differed from other cases in the literature as far as the involvement only for the petrous apex.
Arrested pnuematization has been generally defined as an incidental imaging finding (1,4).
De Jong et al.
reported in their case presentation that for several years the patient suffered headache,
photophobia,
intermittent nausea and vomiting,
and no characteristic was identified in physical,
neurologic and laboratory findings (3).
In our cases the arrested pneumatization was also identified through examinations to diagnosis and pre-diagnosis.
While one case was being examined for reasons of left 6th nerve paralysis and headache,
lesion identification on sphenoid bone led to contrast-enhanced MR assessment but no enhancement was identified.
During patient’s follow-up period of complaint and neurologic findings were seen to regress spontaneously.
Thus,
the symptom was concluded to be unrelated to arrested pneumatization.
Radiologic imaging findings for arrested pneumatization were defined by Welker et al.
as well-circumscribed,
sclerotic margins,
with narrow transition zone,
and curvilinear internal calcification lesions without mass effect and non-expansile in CT examinations.
MR imaging characteristics are in the form of hyperintense appearance,
exhibiting fatty content on T1-weighted images,
no enhancement after gadolinium injection,
and hyperintense appearance on T2-weighted images exhibiting microcytic content.
In light of literature,
in the event of lesions satisfying the defined criteria,
it could be given the diagnosis of arrested pneumatization.
These criteria include presence of lesions in expected pneumatization or known accessory regions,
sclerotic margins,
well-circumscribed and non-expansile,
fatty content,
internal curvilinear calcification shown by CT and normal appearances in any of the related skull base foramens (1).
In differential diagnosis,
fibrous dysplasia,
ossifying fibroma,
chondrosarcoma,
osteomyelitis,
chordoma,
and bone metastases may be considered.
However,
in contrast to the arrested pnuematization,
those lesions do not exhibit fat content and generally have mass effect on surrounding structures (1).
In conclusion,
arrested pnuematization is also observable in the pediatric age group through similar imaging characteristics.
Knowledge of the presence and imaging characteristics of this entity will prevent not only potential confusion in differential diagnoses by radiologists and clinicians,
but also unnecessary advanced investigations and interventions.