These lesions can be classified as:
1.
Normal variants
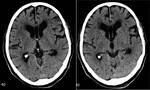
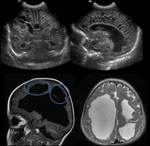
Cavum septi pellucidi: The septum pellucidum consists of two thin sheets of white matter surrounded by gray matter.
The persistence of this septum after birth is called cavum septi pellucidi.
(Fig 1)
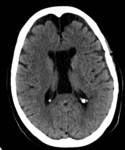
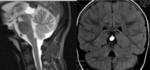
Cavum veli interpositi: An anatomic variant that may appear as a cyst in the pineal region observed in neonatal ultrasound studies,
the internal cerebral veins flows inferiorly.
(Fig 2)
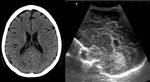
Cavum vergae: Consists of the permanence of the liquid cavity between the two layers of the septum pellucidum extending posteriorly between the fornices.
(Fig 3)
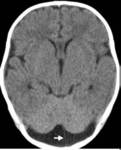
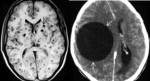
Mega cisterna magna: It has an incidence of 1%.
It is considered megacisterna magna over 10mm when measured in the sagittal plane without involvement of the cerebellar hemispheres.
(Fig 4)
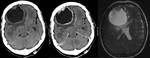
Dandy-Walker malformation: This is a congenital anomaly characterized by the classic triad of hydrocephalus,
absence or agenesis of the cerebellar vermis and posterior fossa cyst communicated with the fourth ventricle.
Secondarily can cause hydrocephalus and intracranial hypertension.
(Fig 5-7)
2.
Cystic lesions of development
Periventricular leukomalacia: periventricular leukomalacia is necrosis of white matter with a characteristic distribution external to the lateral ventricles involving the centrum semiovale that occurs in preterm infants less than 32 weeks.
In ultrasound is displayed first periventricular this being more sensitive to ischemia region hyperechoic areas.
The ultrasound monitoring reveals the formation of cystic lesions.
(Fig 8)
Schizencephaly: Characterized by the presence of slots extending through the whole cerebral hemisphere,
from the ependymal surface to the cortex.
These grooves are lined by dysplastic gray matter.
They can be open or closed.
If they are open,
cerebrospinal fluid (CSF) fills the path between the ventricle and the subarachnoid space of the convexity.
If it is closed,
an indentation is seen in the ventricular wall.
Ventriculomegaly: Consists in dilation of the ventricles due to hydrocephalus,
it may mimic cystic structures.
Linear ultrasound imaging transducer may be useful in identifying the thinned cortical hydrocephalus present and absent in the hydrancephaly.
(Fig 9)
3.
Benign Lesions
Epidermoid cyst: Unlike dermoid cysts,
it contains skin,
epidermal tissue and hair inside.
A common location is in the cerebellopontine angle.
The radiographic appearance is similar to arachnoid cysts being its distinguishable characteristics which would slightly hyperintense on FLAIR and diffusion-restricted.
(Fig.
10)
Dermoid cyst: They represent 0.5% of all intracranial tumors.
The majority are asymptomatic,
symptoms only appear if mass effect and breakage.
Locations vary according to the publications.
The characteristics that differentiate it from the rest is its fat content observed at hypodense (fat density) on CT.
In RM displayed hyperintense on both T1 and T2 by the fat content.
The differential diagnosis must be made with intracranial lipomas and teratoma.
(Fig.
11)
Neural cyst: These are rare,
accounting for 1% of intracranial cysts,
may occur at any location.
The most characteristic finding is a cyst that behaves like the LCR.
The differential diagnosis must be made with arachnoid cysts and Virchow-Robin spaces dilated.
(Fig.
12)
Dilated Virchow-Robin spaces: They are filled with fluid and pial lining,
which accompany the arteries and perforating veins interstitial structures.
Do not communicate directly with the subarachnoid space and are common incidental findings.
Their common sites are the nodes of the lower base,
around the anterior commissure and around the lenticulostriate arteries.
At present cystic RM behavior in all sequences (such as CSF) and do not alter the adjacent parenchyma.
They have no boost or restricted diffusion.
The differential diagnosis must be done with lacunar infarcts
Colloid cyst: Cysts filled with mucin which gives a characteristic typical image.
Almost 100% are nestled in the foramen of Monro.
.
The radiographic appearance is pathognomonic CT is a well-defined hyperdense mass lesion.
Are hyperintense on T1 and T2 isointense the brain parenchyma.
(Fig.
14)
Arachnoid cyst: Arachnoid cysts are cerebrospinal fluid-filled lesions therefore have the same intensity in MRI,
which do not communicate with the ventricular space.
Most are still frequent supratentorial prior to the temporal lobes and posterior fossa.
In extra-axial image shows a well-defined cyst,
scalloping of adjacent bone is a common finding is observed.
(Fig.
15 Fig.
16)
Choroid plexus cyst: These cysts appears in the choroid plexus epithelium.
The majority are asymptomatic and incidental findings.
On unenhanced CT images is isointense to CSF and can show if contrast enhancement,
a finding that should not be confused with mass lesions in this location is given.
In RM are hyperintense on T2 and 2/3 restricted diffusion.
(Fig.
17)
Porencephalic Cyst: These are cavities caused after infection,
ischemic stroke,
or surgery in the brain parenchyma containing LCR behaving similarly to the way the different MRI sequences.
(Fig.
18)
Subependymal cyst: These are rare,
benign,
more frequent in the lateral ventricles or yuxtaventricular region of frontal and temporoparietal lobe.
Most are incidental,
if symptoms can appear,
headache,
seizures or obstructive hydrocephalus.
The diagnostic clue is a cyst content LCR thin wall without enhancement.
(Fig.
19)
Cyst of the anterior commissure: Are neural cysts,
typically receive their name to appear in this location.
The anterior commissure is a fiber tract connecting the two frontal lobes in its basal part.
(Fig.
20)
Choroidal fissure cyst: This is well-defined nodular lesions typically located on the choroidal fissure (between the fimbria of the hippocampus and diencephalon) In RM behave the same signal as CSF,
without restriction or enhancement.
(Fig.
21)
Pineal cyst: They appear in 10% of cases as a unilocular cyst located in the pineal gland which attenuation varies according to content.
Observed T1 FLAIR hyperintense while they may not be completely hypointense.
After administration of contrast may show nodular or ring enhancement.
The differential diagnosis is made with pineocytoma,
imaging may be indistinguishable.
(Fig.
22)
Cyst of Rathke's pouch: These cysts arising from embryonic remnants of Rathke's cleft.
The best imaging clue is a suprasellar cyst with a small intracystic nodule.
MRI features are variable in T1 and hyperintense on T2.
The differential diagnosis includes lesions such as craniopharyngioma location.
(Fig.
23)
Meningocele: Meningocele of the petrous apex is a rare injury.
Pathologically corresponds to a herniation of the subarachnoid space from the posterolateral portion of Meckel's cave to the petrous apex.
It is well defined hypodense lesions on CT and T2 hiperintesas.
The distinctive radiographic appearance of the cystic lesion of the petrous apex allows the radiologist to pose a high degree of diagnostic certainty (Fig.
24)
Cystic hygroma: This is a wall filled lesion with CSF appears secondary to a subdural hematoma.
In image behaves with the same characteristics as the LCR.
The knowledge of the previous history gives us the diagnosis.
(Fig.
25)
4.
Infectious lesions
Neurocysticercosis: Most neurocysticercosis cysts are in the subarachnoid space,
typically on another common basal cisterns being located in the periventricular white matter.
Radiographic findings vary chronologically in early or vesicular phase is characterized by fine cysts and smooth walls.
When the cyst degenerates and initiates the inflammatory response and enhance the perilesional edema appears.
In residual phase is characterized by calcified nodules.
(Fig.
26)
Echinococcosis: The most common site is the brain parenchyma supplied by middle cerebral artery.
A single,
large cyst,
well-defined non-enhancing density similar to CSF may be seen in the CT,
calcifications were observed.
(Fig.
26)
Abscesses: Clinical patient is especially useful for diagnosis.
Abscesses are characterized by low signal intensity on T1 and hyperintense on T2 and FLAIR with peripheral ring enhancement and restricted diffusion.
The differential diagnosis in the absence of infectious clinic,
is with primary tumor.
(Fig.
27)
5.
Tumoral lesions
Cystic component is commonly found in some types of brain tumors.
In posterior fossa cerebellar hemangioblastoma,
pilocytic astrocytoma,
ependymoma and medulloblastoma is common.
A supratentorial level we can find cystic-necrotic degeneration in tumors such as meningioma,
glioblastoma multiforme,
brain metastases,
cystic tumors prolactinoma while others show main characteristic cystic degeneration (central neurocytoma,
craniopharyngioma)
Hemangioblastoma: is a vascular tumor that occurs in patients with syndrome of Von-Hippel-Lindau.
Typically occurs in young patients in posterior fossa (95%).
On CT and MRI,
a cystic lesion with a mural nodule observed that enhances after contrast.
(Fig.
28)
Pilocytic astrocytoma: It most often occurs in young and located in the brainstem and cerebellar patients.
It has a strong association with neurofibromatosis type 1 localized in these cases the optic nerve.
TC radiologically large cyst with a mural nodule that enhances after contrast while RM is iso-hypointense to brain parenchyma on T1 and hyperintense on T2 is observed.
(Fig.
29 Fig.
30)
Central neurocytoma: A high percentage of these tumors are intraventricular located mostly in the lateral ventricles.
The main feature is cystic regions with the what are hypointense on FLAIR.
Calcification is common in about half of cases.
(Fig.
31)
Craniopharyngioma: It has a bimodal incidence peaks at age 12 and another in middle-aged adults.
Its typical location suprasellar cystic component and calcification help us with the diagnosis.
(Fig.
32)
Cystic meningioma: Between 10-20% of meningioma undergo cystic degeneration.
The tumor has the same radiological features as meningioma,
slightly hyperdense calcifications (20%) with intense and homogeneous enhancement after administration of contrast CT with dural tail.
In RM behaves partly cystic hyperintense on T2.
The differential diagnosis if they are in the cerebellopontine angle is done with schwannomas.
(Fig.
33)