Informed consent was signed by all patients who accepted to participate to this study,
validated by the clinical research center of our institution.
Eight needles in eight patients treated by radiofrequency thermal ablation (RFA) for hepatic tumors were evaluated.
The insertion of a 22G spinal needle in the liver was performed using the CT–ultrasound fusion imaging system (Toshiba,
TUS-A500,
SmartFusion application).
The aim was to put the needle just at the contact of the lesion,
without penetrating it.
Shortly,
a magnetic position sensor was attached to the ultrasound transducer shaft.
A CT scanner was performed just before the procedure and 3D DICOM data sets were used for fusion.
A general anesthesia was performed before the CT scan acquisition and the patient remained in the same position on the CT table during the whole procedure.
Rigid coregistration was performed using one to three anatomical points (portal vein,
coeliac artery,
hepatic veins) to match the two imaging data sets spatially to each other.
To calculate the real coordinates of the needle,
CT scanner was repeated once the spinal needle in its final position.The accuracy of the fusion system was evaluated with the 22 Gauge needle tip position and did not concern the insertion of the final needle used for thermal ablation.
Once the procedure finished,
differences between real (x,
y,
z) and virtual (x’,
y,’ z’) coordinates of the tip of the needle (D for distal point) and of a needle point located 3cm proximally to the tip (P for proximal) were calculated (Figure 2).

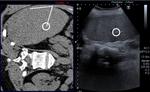
Fig. 2: Virtual CT image (left side) and corresponding real-time US image (right side) used for the insertion of the 22G needle in the liver. Distance between the tip of the needle (white point in the circle on US image) and the liver capsula and angulation between the needle and the tangent of the capsula are calculated on the US image and reported on the CT image.
X,
y and z coordinates correspond to the left-right,
antero-posterior and cranio-caudal axis respectively.
Real coordinates were easily calculated on the control scanner.
To obtain virtual coordinates,
the CT plane seen on the US fusion had to be exactly reproduced using the initial 3D CT volume.
Virtual location of the tip of the needle was then reported on the CT volume and coordinates (x’,y’,z’) of points P and D calculated (Figure 3).

Fig. 3: Reconstruction of the virtual CT plane with the initial CT volume to get virtual coordinates of the tip of the needle (D’(x’, y’, z’)) and a point on the needle 3cm proximally from the tip (P’(x’, y’, z’)). All of the organs seen on the picture have to present the same aspect as on the virtual CT plane (figure 1, left side). Once the good plane obtained, same angulation and distance of the needle in the liver as seen on real US image are reported on the plane and virtual coordinates calculated.
Statistical analysis
A baysian analysis of the data was performed to know the probability of the error to be less or more than 7 mm: this value was considered to be acceptable for an ablation of a hepatic tumor.
It was not possible to obtain p values as the number of patient included was too small.