With increasing in the aging population and due to lifestyle habits,
the incidence of stroke is on the rise.
Stroke occurs when there is abrupt interruption of blood flow to part of the brain,
either due to an emboli or thrombosis.
Even though it is common,
diagnosing stroke is not always easy.
Stroke mimics { Todd's paresis etc}can behave like stroke,
making clinical diagnosis difficult. Often,
imaging is the only way of diagnosing or excluding stroke.
Up to 30% of stroke mimics are misdiagnosed by physicians in hospitals.
The clinical presentation of stroke varies,
however,
sudden onset of neurological deficit in a vascular distribution associated with hemiparesis,
facial weakness and aphasia is likely to be stroke.
Clinical history is important and helps in distinguishing stroke from mimics.
Rapid diagnosis and recognition of stroke is important for quick clinical management and better patient outcome. Late presentation at the clinics or hospital can be challenging,
for the clinicians as well as for the Radiologists.
A large number of disorders can mimic stroke accounting for 20-25 % of stroke presentations,
and the results can be serious for the patient.
Careful history taking and neurological examination is mandatory.
Stroke mimics are manifestations of nonvascular disease when a stroke-like clinical presentation is noted.
Presentation resembles or even be indistinguishable from a vascular stroke. Mimics can be within the central nervous system or systemic events. Studies have shown that initial diagnosis of stroke is inaccurate in approximately 12% of patients.
CEREBROVASCULAR SUBTYPES
1.
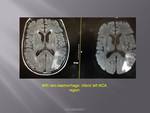
Ischaemic Stroke
2.
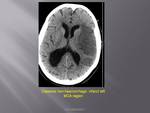
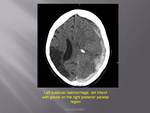
Haemorrhagic stroke
3.
Lacunar infarct
4.
Intra cerebral haemorrhage
5.
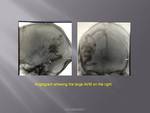
Arteriovenous malformations {AVM}
6.
Venous thrombosis
7.
Arteritis
8.
Arterial dissections
HYPOGLYCAEMIA:
Normally presents with autonomic symptoms,
however it can present with focal neurological symptoms.
Transient hypoglycaemia may produce picture of hemiplegia and aphasia.
Hypoglycaemia occurs when the blood glucose level is less than 45mg/dl.
Causes include medications{ insulin,
sulphonylureas},
alcohol,
insulinoma,
starvation.
Blood sugar should always be checked in diabetics and in elderly.
The hemiplegia may resolve immediately with the administration of intravenous glucose but can take longer
SEIZURES:
Post seizure paresis is sometimes difficult to differentiate from stroke,
accounting for 20% of the mimics.
History is important in such cases,
though not often available.
MRI imaging is the best option in such presentations.
Seizure may also present as a complication of stroke or develop in a patient with a history of stroke
SEPSIS
12% of stroke mimics is due to sepsis.
Raised inflammatory markers,
high fever,
changes on Chest Radiographs could represent sepsis.
It should be noted that sepsis due the hypercoagulable state can a risk factor for stroke.
MIGRAINE/HEADACHES
Headache is common,
some stroke patients develop headache and can mislead the examining physician.
Normal CT and MRI imaging in most cases
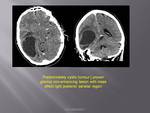
TUMOURS
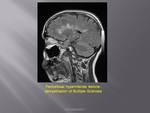
Primary or secondary tumours usually cause progressive neurological deficit.
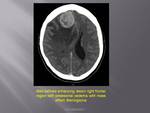
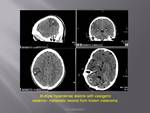
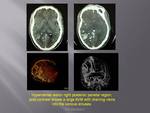
Acute presentation could be secondary to haemorrhage into the lesion,
extrinsic compression of vasculature due to oedema,
hydrocephalus.
PSYCHIATRIC/FUNCTIONAL
Functional disorders and feigned stroke manifest as acute sensory disturbance and weakness/ Signs and symptoms are inconsistent,
imaging not usually indicated