This study was approved by the institutional review board and informed consent was obtained from all of the patients after providing the study’s details,
including information on the additional radiation dose.
Patient Population and Study Design
Between February and May 2013,
336 consecutive patients who were suspected of having urolithiasis and scheduled to undergo non-enhanced CT were enrolled in this study.
Instead of using specific eligibility criteria,
we relied on the assessments carried out by the outpatient or emergency room physicians that led to the clinical suspicion of urolithiasis.
Before the exam,
we informed the patients about this prospective study and acquired consent.
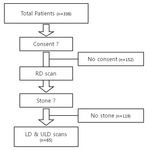
Patients who did not want to undergo additional scans or didn’t have urolithiasis were excluded (Figure 1).
CT Protocol
All studies were performed with a 256-MDCT scanner (Brilliance iCT,
Philips Healthcare,
Cleveland,
OH,
USA).
First,
all patients underwent a regular dose (RD) protocol scan from the proximal aspect of the T12 vertebra to the distal aspect of symphysis pubis in the supine position.
If the patient had a urolithiasis in the RD scan and consented to this study,
additional scans using the low dose (LD) and ultralow dose (ULD) protocols were performed.
The scan range of LD protocol was the same as the RD protocol,
but that of the ULD protocol was limited to the area where the urinary stones were expected.
To minimize positional differences,
the time between each scan was kept to a minimum.
The RD and LD protocols were acquired at manually fixed peak tube voltage of 120 kVp and 100 kVp,
respectively,
with automated Z-axis dose modulation by the scout image (DoseRight,
Philips Healthcare,
Cleveland,
OH,
USA).
The maximal tube current of the RD and LD protocols was limited to 150 mAs and 100 mAs,
respectively.
The ULD protocol was acquired at manually fixed peak tube voltage and tube current of 100 kVp and 20 mAs.
The remaining scanning parameters were as follows: detector configuration,
128x0.625; pitch,
0.915; beam collimation,
80 mm; rotation time,
0.4 sec; and helical acquisition.
Image Reconstruction
The raw data of RD protocol was reconstructed into axial and coronal images using the FBP algorithm and that of LD protocol was reconstructed using iDose level 5 (Philips Medical Systems,
Best,
the Netherlands) which is a commercial statistical IR algorithm.
The raw data of the ULD protocol was reconstructed to another three axial images using FBP,
iDose level 5,
and iterative model reconstruction (IMR) Soft Tissue level 3 which is a pre-released knowledge-based IR prototype system.
All reconstructed section thicknesses and intervals were 3mm.
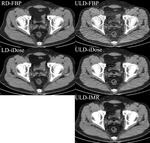
Thus five reconstructed imaging data sets were ultimately obtained: RD-FBP,
LD-iDose,
ULD-FBP,
ULD-iDose and ULD-IMR (Figure 2).
Radiation Dose
To evaluate the radiation dose,
the effective radiation doses of each protocol were calculated as mSv from the recorded dose-length product (DLP) reported by the CT scanner with the conversion factor (0.015) [16].
The effective radiation dose of a full scan range in the ULD protocol was assumed by the number of slices compared to the RD and LD scans because of the limited scan range in its protocol.
The reduction in radiation dose was compared between the three scans.
Image Quality Assessment
Objective image noise assessment
During the objective noise measurement,
the radiology resident (one of the two reviewers of diagnostic performance) recorded the standard deviation (SD) of Hounsfield units (HU) by placing a circular region of interest (ROI) of 80–110 mm2 in the skeletal muscle and the subcutaneous fat area at the same level where the largest urinary stone was present.
The objective image noise was reflected by the SD of attenuation in the circular ROI.
Subjective image assessment
To evaluate the subjective image,
the staff radiologist (one of the two reviewers of diagnostic performance) who was blinded to the detailed technical scanning parameters used and subjectively graded the image’s quality,
noise,
and the reviewer’s confidence in each image set according to the previously reported 3 or 5 point scale [13].
All of the images were displayed in a random fashion and the reviewer was permitted to change the window level and width.
Consequently,
the subjective image quality,
with respect to the depiction of urinary stones,
was rated on a 5-point scale (1 = poor,
not diagnostically acceptable for interpretation; 2 = suboptimal,
worse than acceptable quality; 3 = acceptable,
diagnostic interpretation possible; 4 = good; and 5 = excellent).
Subjective image noise was rated on a 3-point scale using the graininess of the image or pixel to pixel variation (1 = minimal; 2 = acceptable; 3 = excessive,
rendering diagnostic interpretation impossible).
In addition,
the confidence level of radiologist with regard to the stone depiction was rated on a 3-point scale (1 = no confidence; 2 = confidence with reservations; and 3 = highly confident).
Diagnostic Performance and Inter-observer Agreement
All of the reconstructed image data sets were transmitted to the picture archiving and communication system (PACS) for image analysis.
A consensus panel was formed to establish the reference diagnosis of stones based on RD-FBP and consisted of two abdominal staff radiologists who did not evaluate the diagnostic performance in the LD images.
For the diagnostic performance,
two reviewers (a radiology resident,
3rd year and a staff radiologist with 12 years of experience) interpreted the number,
location,
and size (< 3mm or larger) of the urolithiasis independently in LD image sets.
The concordant rate between RD and LD image sets was calculated according to the diagnostic performance of both reviewers,
and the inter-observer agreement was evaluated.
All comparisons were performed after dividing the stones into 3 groups; all sizes,
≥ 3 mm,
and < 3 mm.
Statistical Analysis
Statistical analysis was performed using IBM SPSS 20 (IBM Software Inc.).
All the recorded data was presented as mean ± SD.
For the radiation dose and objective image noise,
a paired-t test was performed to compare each image set.
The subjective image quality was compared by using the Wilcoxon signed rank test.
Inter-observer agreement between the radiology resident and staff radiologist for urolithiasis in LD image set was calculated using Cohen’s kappa values and all kappa values were interpreted according to following: poor for a k value of 0.19 or lower; fair for a k value of 0.20–0.39; moderate for a k value of 0.40–0.59; substantial for a k value of 0.60–0.79; and almost perfect for a k value of 0.80–1.00.
The p value < 0.05 was considered to show a statistically significant difference.