We retrospectively reviewed the patients with proven hydatid disease between 2009-2014 in our institution.
From a total of 52 patients,
we selected the images that best defined the typical features of the disease,
in order to describe radiological findings.
Hydatid cysts are most commonly found in liver (up to 80% of the cases) followed by lungs.
Echinococcal disease in other unusual locations can be a diagnostic challenge.
The WHO / IWG classification proposed by WHO in 2013 (World Health Organization Informal Working Group who/ IWG) guides us about the infection status and its evolution through ultrasound characteristics.
According to this classification we can identidy:
ACTIVE STATE INFECTION
• Unilocular cystic lesion,
anechoic content,
without clearly visible wall.
The aetiology can be diverse and undistinguishable. If it was a hydatid cyst,
it would be an early stage and it wouldn't be productive,
because it hasn't got scolex in spite of the stage is active.
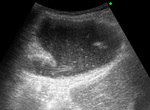
• Hydatid cyst type 1: Unilocular and anechoic lesion with uniform visible wall (double line) and internal echoes ("Snowflakes sign").
The findings are pathognomonic.
(Figure 1).

Fig. 1: US shows an hydatid cyst type 1: Unilocular lesion with internal echoes ("Snowflakes sign").
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia.
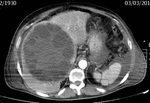
• Hydatid cyst type 2: Multivesicular lesion with visible wall and daughter cysts (honeycomb sign).
Daughter cysts are usually more anechoic that liquid that contains them and they may fill completely or partially the cyst (figure 2). The findings are pathognomonic.

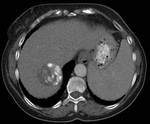
Fig. 2: Contrast-enhanced CT shows an hydatid cyst occupying almost the entire hepatic right lobe with multiple daughter cysts distributed peripherally. Its content are more hypodense that hydatid matrix. Perisplenic and perihepatic fluid is also identified.
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia.
TRANSITIONAL STATE
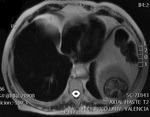
• Hydatid cyst type 3: Detachment of the laminate membrane which floats in the cyst ("Snake sign").
The findings are pathognomonic.
(Figure 3)

Fig. 3: T2 MRI shows a splenic cystic lesion with hypointense wall and release of the hyperintense germinative membrane, which is collapsed and floats inside."Snake sign".
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia.
INACTIVE STATUS
• Hydatid cyst type 4: Hypo or hyperechoic heterogeneous lesion,
with content from degradation cyst.
No daughter vesicles are observed.
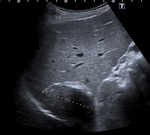
• Hydatid cyst type 5: Thick wall calcification,
particularly of periquiste,
curvilinear or ring morphology,
producing a subsequent acoustic shadow.
The findings are highly suggestive but not pathognomonic.

Fig. 4: US shows an hypoechoic and heterogeneous liver lesion with wall calcifications. Hydatid cyst type 5
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia.

Fig. 5: a) Contrast-enhanced CT demostrates a calcified splenic hydatid cyst wall, with ring morphology. b) Another patient chest x-ray lateral shows an spherical calcification infradiaphragmatic corresponding to a splenic hydatid cyst calcified wall.
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia.
Inactive state is not equivalent to talk about parasite's death.
Death just occurs after the calcification of all components.

Fig. 7: Spleen cystic lesions with wall calcifications and dense calcifications occupe almost the entire cyst.
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia. Spain
EXTRAHEPATIC HIDATIDOSIS
LUNGS
Lungs is the second most affected organ (15%).
It is more common in the lower lobes though. Cysts can be asymptomatic long periods of time and are diagnosed as an incidental finding.
SPLEEN
Spleen is usually the third most common site after liver and lungs.
It develops secondary to systemic or intraperitoneal dissemination as a result of breakage of hepatic hydatid cysts.
The differential diagnosis includes epidermoid cysts,
pseudocysts,
abscess,
hematoma and neoplasms.
DIAPHRAGMA
Diaphragmatic localization is very rare with an incidence of barely 1%. It may occur when the cyst migrates eroding the diaphragm and pleura and is introduced then in the lung (transdiaphragmatic migration).

Fig. 12
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia. Spain
PERITONEUM AND RETROPERITONEUM
Involvement at this level is usually secondary as spontaneous or iatrogenic rupture of a hepatic,
splenic or mesenteric cyst and can be located anywhere in the peritoneum.
When there is only a cyst,
it can not be distinguished from other mesenteric peritoneal cysts including duplication cyst.
BONE AND SOFT TISSUE
The soft tissue involvement is uncommon even in endemic areas,
particularly in absence of prior liver involvement.
The involvement of soft tissues,
including muscle,
stands at 2.3% in endemic areas.
Hydatid cyst growth within the muscle is hindered by the presence of lactic acid and the muscle contraction.
It doesn't exist however,
pericystic formation in bones,
and lesion assumes an irregular morphology in the direction of least resistance from the bone.
It comes as a lytic lesion with soft tissue extension.
Bone involvement is seen most frequently in the spine and pelvis.
It usually appears with the form of osteolytic lesion associated with multilocular,
well-defined cysts,
there may be thinning and cortical erosion extending to adjacent soft tissue.

Fig. 10: Multiple cystic images are seen with hyperintense thick wall that encroach the abdominal wall, extending itself across the transverse and oblique muscles, right iliac fossa and iliopsoas muscle.
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia. Spain

Fig. 11: Welldefined and multiloculated cysts, partially calcified, with expansion of the bone (osteolytic lesion) and extension into the adjacent soft tissue.
References: Servicio de Radiodiagnóstico, Hospital Clínico Universitario de Valencia. Spain
GENITOURINARY TRACT
The affectation is due to hematogenous spread.
Cysts appear most of the times lonely and located in the cortex,
that's why they are difficult to distinguish from simple renal cysts and can become large affectations in the end.
If the collecting system breaks it can simulate a renal colic.
The hidatiduria echinococcal is pathognomonic of renal or urinary tract disease.
The differential diagnosis includes essential cysts and polycystic kidney disease,
in case there are multiple cysts,
with the main difference that polycystic kidney disease affects both kidneys but hidatidosis does not.
If the hydatid cyst density has increased on CT,
or US shows echogenic foci,
it may resemble a renal abscess or complicated cyst.
We also included in the differential diagnosis renal neoplasms with a cystic component.
PANCREAS AND ADRENAL GLANDS
Hydatidosis in these locations is extremely rare. Diagnosis based on imaging tests only is not enough.
COMPLICATIONS
- Rupture: Natural history implies cyst rupture in 50-90% of cases.
Rupture is due to trauma,
host response or cyst degeneration.
It can be focused directly into the peritoneal or pleural cavity, abdominal viscera or affecting communication to the bile duct.
External compression by the cyst also can cause dilated bile duct.
Cyst free fluid circulation can cause anaphylactic reactions.
- Superinfection: A poorly defined margins lesion,
an halo around the lesion which not presented enhancement on constrast-enhanced CT,
patchy areas of diferent density in the rest of the parenchyma in relation to inflammatory changes or fluid levels on CT can suggest superinfection.
The presence of air not always means there is infection,
it can also occur after direct lung cyst rupture or communication with a hollow viscera.
- Transdiaphragmatic direct extension and migration.