Extending the TE echo times from 11 to 22 and 33 ms had a similar ‘whitening effect’.
The RESTORE version of the T1 measurement did not cause any significant increase to the measurement time.
High bandwidths (BW) were selected to produce as few chemical-shift artifacts as possible: 250 Hz/pixel for 1.5T and 450 Hz/pixel for 3T.
Adaptation of a standard T1 sequence: High bandwidth to ensure less chemical shift in the case of 1.5T BW 250 Hz/ pixel (less than 1 pixel shift).
450 Hz/ pixel for 3T BW (approximately 1 pixel shift).
In the Siemens toolbox,
select the RESTORE pulse on the contrast card and offset the TR against the couplings to remain in the 500 to 700 ms TR range for many of the slices (2).
Connecting a -90 degree pulse at the end of the read-out (RESTORE or flip-back pulse) shifts all transverse magnetization back towards the z-direction,
thereby increasing the number of protons available for the next stimulation.
The ‘flip-back pulse’ (known as RESTORE,
DRIVE,
or DEFT,
for example,
by the various manufacturers) was originally intended for T2-weighted measurements,
both to save time and to obtain a light fluid signal in the case of a short TR (3).
As a result,
the synovial fluid obtains a higher signal,
meaning a new contrast is achieved in the structures surrounding the joint: synovia,
capsule,
cartilage,
and periarticular fat.
This allows synovial pathologies and/or disorders with this modified T1 weighting to be displayed without any contrast agents.
T1 RESTORE in rheumatic diagnostic.
35-year-old patient with recurrent swelling and pain in the left knee.
(Fig.
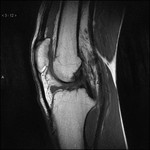
1) Native conventional T1-weighted measurement,
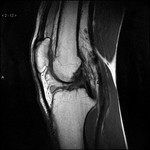
(Fig.
2) T1 RESTORE in the same position and the same slice thickness reveals the synovial fluid in the recessus suprapatellaris,
thereby highlighting a synovia in this case with inhomogenous thickening.
The patient was back to full health after 6 weeks of rheumatic therapy.
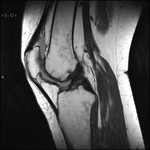
T1 RESTORE in psoriatic arthritis diagnosis.
T1 native comparison: (Fig.
3) Fluid is concealed in the conventional T1-weighted sequence.
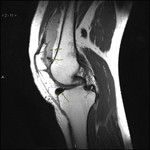
T1 RESTORE (Fig.
4) highlights the synovial fluid and in this case reveals the significantly thickened synovia: Findings indicate psoriatic monoarthritis.
(Fig.
5) In the proton-density-weighted sequence with fat saturation,
the synovia which is thickened to 2 mm is concealed by the high T2 contrast.
(Fig.
6) The synovia is only visible in the T1 FS sequence for a few minutes following the addition of an intravenous contrast agent.
In the later measurements,
the contrast agent is excreted into the joint cavity and blurs the outline of the synovia on the side of the joint once again.
T1 RESTORE in synovia diagnostic.
(Fig.
7) T1 RESTORE highlights fat/synovia/synovial fluid,
whereas (Fig.
8) no contrast between fat/fluid can be detected in the PD-weighted sequence without FS,
i.e.
fat and water are equally light.
Once again,
significant thickening of the synovial membrane can be seen along with an effusion that spreads over the infrapatellar fat pad.
T1 RESTORE in arthrofibrosis diagnostic.
Unlike common PD FS sequences (Fig.
9),
T1 RESTORE (Fig.
10) highlights the severe fibrotic synovial proliferation.
The knee joint is suffering from extreme limitations to its range of flexion/extension consistent with this type of membrane scarring.
Condition after three rounds of arthroscopic surgery (cartilage grinding) and a partial resection of the medial meniscus.
One of the most common causes of this frequently painful scarring,
along with primary inflammatory rheumatic diseases.
T1 RESTORE in synovia diagnostic.
Thanks to its fluid contrast with high spatial resolution,
the T1 RESTORE sequence (Fig.
11,
12) displays conical or even oval-shaped synovial villi,
along with low-signal lesions in the synovia that indicate hemosiderin (blood) or calcium (the latter is easily excluded with an X-ray).
The distribution pattern of the synovial specks is typical of diffuse pigmented villonodular synovitis (PVNS),
which has been histologically confirmed.
T1 RESTORE in cartilage diagnostics.
(Fig.
13) The moderate T1 fluid contrast reveals a one-millimeter-small,
free fragment that can no longer be seen in the sharp PD FS contrast image (Fig.
14).
Furthermore,
the third-degree cartilage lesion – including the reactive accompanying subchondral cortical sclerosis – is illustrated more clearly in the T1 measurement.
The fibrillar protrusion of cartilage on the surface is displayed equally clearly,
if not better.
T1 RESTORE in ligament diagnostics.
Fig.
15,
16
Even capsule pathologies can frequently be examined with significantly greater accuracy (using the moderate fluid contrast).
The extravasation of synovial fluid is particularly clear in the contrast agent study on the right.
The type of capsule lesion (in this case,
atraumatic) and the leakage in the capsule that has been destroyed by inflammation are concealed in the T1 FS post-gadolinium contrast agent.
Fig.
17
The image displays an example of millimeter-thick,
intra-articular ligament and cartilage diagnostics.
A new,
traumatic,
intra-articular ligament rupture resulting in a scaphoradial lunar collapse and chondral defect on the radial side are already visible in the coronary T1 RESTORE measurement