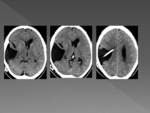
RADIOLOGICAL DIAGNOSIS:
Computed tomography (CT) is the gold standard for diagnosis.
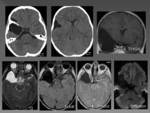
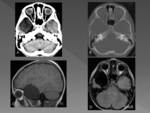
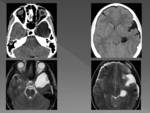
CT imaging of an AC will show a noncalcified homogeneous extra-axial cystic lesion,
similar to LCR attenuation that does not enhance with contrast administration and produces remodeling of adjacent bone structures.
MRI is a useful tool for diagnostic complementation.
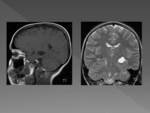
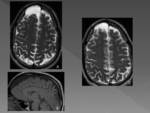
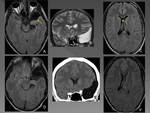
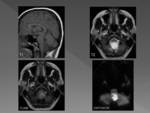
On MRI AC has the same signal intensity as CSF at all sequences.
AC will suppress completely on fluid attenuated inversion recovery (FLAIR) imaging and will not demonstrate restriction on diffusion-weighted images,
therefore are hypointense on these sequences Fig. 3 Intracystic bleeding or high concentrations of proteins may change the signal intensity.
AC displace adjacent nerves and cranial vessels rather than engulf them.
The use of phase-contrast (PC) cine MR imaging allows for observation of the CSF flow between the subarachnoid space to the interior of the cyst.
On the PC cine MRI to observe hyperitense or hypointense areas within the AC means that the cyst and the subarachnoid space are communicated.
Differentiation of communicating cysts and noncommunicating ones can be useful for surgical planning.
CLINICAL MANIFESTATIONS
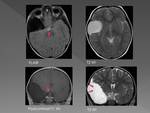
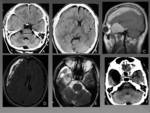
The clinical manifestations will depend on the size of the cyst and its location Fig. 4 .
Small cysts are often incidental findings Fig. 5,
while large cysts are usually symptomatic.
When they are too large can cause raised intracranial pressure and / or direct compression of cranial structures.
They can cause bone remodeling,
in young children may produce macrocrania and / or cranial asymmetry Fig. 6 .
The AC have also been associated with delayed psychomotor development.
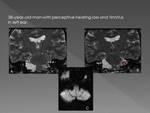
In older children the predominant symptom is headache Fig. 7 ,
and up to 25% of cases may be associated with seizures Fig. 8
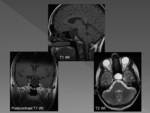
Cysts in the chiasmatic region can produce visual disturbances and endocrine disorders due to compromise of the hypothalamus-pituitary.
Fig. 9.
The AC can produce hydrocephalus by compression of the third ventricle and the fourth ventricle when they are located in the posterior fossa.
COMPLICATIONS:
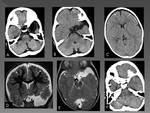
Complications are rare but potentially serious,
among these include subdural hematoma Fig. 10,
intracystic hemorrhage,
acute cyst expansion and subdural hygroma Fig. 11,
Fig. 12 and Fig. 13.
DIFFERENTIAL DIAGNOSIS
The main differential diagnosis will do with epidermoid cysts,
which look identical to CSF on CT and MRI,
but epidermoids cysts do not supress completely on FLAIR sequences and they restrict on diffusion -weighted images.
Fig. 14
TREATMENT
Surgical treatment,
either by craniotomy,
endoscopic fenestration,
needle aspiration or cystoperitoneal shunting Fig. 15 is reserved for cases of large cysts,
symptomatic or complicated. Expectant management is recommended for patients with small and asymptomatic cysts.