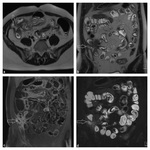
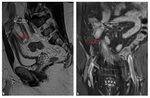
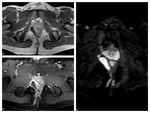
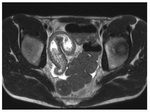
We have retrospectively reviewed MRE examinations performed in years 2012-2014 at our Department and further selected those of 128 patients with CD confirmed with histopathological examination.
All examinations have been performed in a 1.5-T scanner,
using a phased array surface coil.
The recipe for optimal MRE includes adequate bowel distention,
fast sequences,
use of a large field-of-view surface coil and administration of an intravenous contrast agent.
Adequate bowel distention. Several types of enteric contrast agents (CA) may be used to study the small bowel with MR imaging - see Table 1.
At our institution we administer 3% mannitol solution in 1-1,5 l.
of water at regular intervals over a 40 to 60 minute period prior to examination in adults patients.
In paediatric population the volume of oral contrast medium is adjusted according to the weight of the patient.
It may also be helpful to administer 10 - 20 mg of hyoscine butylbromide intravenously prior to the examination or prior to contrast-enhanced sequences,
depending on the inclusion of cine sequences in the imaging protocol,
if otherwise not contra-indicated (e.g.
history of cardiac arythmia,
glaucoma) to decrease bowel motility.
Alternatively you can administer 1 mg glucagon intravenously or intramuscular if applicable.
Contra-indications to glucagon administration include a known hypersensitivity to glucagon or a history of pheochromocytoma.
It is advised that patients fast for 4 to 6 hours prior the examination as it not only helps to decrease the amount of food residue but also facilitates tolerance for the necessary intake of large volume of enteric contrast.
|
Table 1.
Enteric contrast agents (CA) in MRE (after Allen et al.
2014 with alterations).
|
|
Type of CA
|
Negative CA
|
Positive CA
|
Biphasic CA
|
|
Signal intensity on
T1-weighted images.
|
Low.
|
High.
|
Low.
|
|
Signal intensity on
T2-weighted images.
|
Low.
|
High.
|
High.
|
|
|
Ferumoxil oral suspension.
|
Based on gadolinium chelates and manganese.
Blueberry juice,
milk.
|
Water,
polyethylene glycol,
diatrizoate meglumine,
mannitol,
locust bean gum solutions,
methylcellulose,
low-density barium suspensions.
|
|
Remarks
|
Provide ability to visualize higher signal intensity bowel wall against dark contents in the lumen.
|
Can mask bowel wall abnormalities.
Allow assessment of enteric contrast progression though the bowel.
|
Provide optimal contrast between the bowel lumen and its wall without obscuring bowel wall enhancement on T1-weighted images.
|
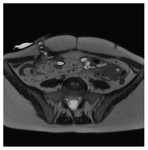
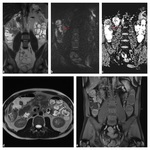
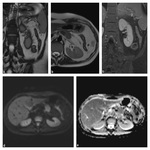
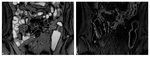
MRE imaging protocol. Patients are imaged in the supine or prone position (if no stoma is present) using a phased array surface coil - see Fig.
1.
Coronal sequences are faster to perform in the prone position due to thinner volume of tissue to imagine.
Both positions,
however,
are equivalent in detection and characterization of bowel lesions.
With the exception of diffusion weighted sequences (DWI) all scans are performed at breath-hold.
MRE protocol includes sequences post intravenous administration of 0.1 mmol/kg gadolinium-based contrast agent at 2ml/s followed by a 20 ml saline flush,
both dynamic and delayed.
Table 2 displays the list of sequences used in our MRE protocol as well as their order and rationale.
At times we extend our imaging protocol during the examination if we find it necessary for stating the correct diagnosis.
|
Table 2.
MRE imaging protocol applied in our institution.
|
|
|
Sequence
|
Remarks and Rationale
|
|
1
|
T1 FL2d Cor1 mbh2
|
Encompasses the whole abdomen and pelvis.
Provides anatomic overview and preliminary assessment of bowel distention.
|
|
2
|
T1 FL2d FS3 Cor mbh
|
Provides anatomic overview and preliminary assessment of bowels,
incl.
bowel walls.
|
|
3
|
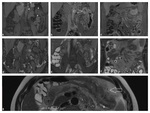
T2 HASTE4 Cor mbh
|
Localization of findings.
Susceptible to artifacts - bulk motions of intraluminal fluid may simulate filling defects.
See: Fig.
2.
|
|
4
|
T2 HASTE STIR5 Cor mbh
|
Useful in evaluation of bowel wall oedema and intra-abdominal fluid collections.
The use of fat saturation in one of T2-weighted sequences allows differentiation between submucosal fat and oedema,
both bright on T2-weighted images.
|
|
5
|
T2 Trufi6 Cor bh7
|
Chemical shift artifacts result in a “black boundary” effect around structures what makes mesenteric nodes and vessels more conspicuous but may simulate bowel wall thickening.
See: Fig.
3b.
Provides good delineation between the bowel and the mesentery.
|
|
6
|
T2 HASTE Tra8 mbh
|
Allows multiplanar correlation.
|
|
7
|
DWI9 Cor
(b 0 50 500 800)
|
Displays areas of diffusion restriction in case of active inflammatory lesions and abscesses.
Facilitates detection of lymph nodes.
|
|
8
|
T1 FL2d Tra mbh
|
Pre-contrast sequence.
|
|
|
9
|
T1 Vibe10 FS Cor dyn11 mbh (CM dynamic)
|
Performed in the arterial (30 s) and portal venous (60-70s) phases using a bolus triggering once contrast reaches descending aorta.
Subtracted images are obtained as well.
Slice thickness 1.6 mm.
|
|
10
|
T1 Vibe FS Cor mbh
(CM delayed)
|
Post-contrast delayed sequence.
Facilitates to demonstrate extraluminal abnormalities such as fistulas.
Slice thickness 1.6 mm.
|
|
11
|
T1 FL2d Tra mbh (CM)
|
Allows multiplanar correlation and facilitates to demonstrate extraluminal abnormalities such as fistulas.
|
|
Examinations are performed in a 1.5-T scanner with the use of a phased array surface coil.
1 Cor - coronal plane,
2 mbh - multiple breath hold,
3 FS - fat saturation,
4 HASTE - half-Fourier acquisition single-shot turbo spin-echo,
5 STIR - short tau inversion recovery,
6 Trufi - true fast imaging with steady-state free precession,
7 bh - breath hold,
8 Tra - transverse plane,
9 DWI - diffusion weighted imaging,
10Vibe - volumetric interpolated breath-hold examination,
11 dyn - dynamic imaging post intravenous contrast agent administration.
|
Interpretation of MRE images requires familiarity with the normal anatomy as well as imaging signs of active and chronic bowel inflammation.
Normal appearance of bowels in MRE. The small intestine is most commonly affected by CD.
Work by Cronin et at.,
who retrospectively evaluated 65 subjects with no underlying small bowel disease followed up over a period of three years,
established that the mean diameters of the duodenum,
jejunum,
proximal ileum,
distal ileum and terminal ileum measure 25 mm,
24.5 mm,
19.5 mm,
19 mm and 19 mm respectively.
The bowel wall thickness is similar throughout the length of the small bowel,
measuring 1.5+/-0.5mm.
The number of folds per 2.5 cm decreases from 4.6 in the jejunum to 1.5 in the terminal ileum and the fold thickness varies from 2.1 - 1.8 mm.
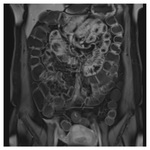
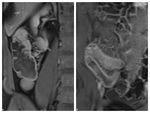
Due to increased surface area,
the jejunum enhances more than the ileum - Fig.
4.
Normal large bowel wall thickness should not exceed 3 mm,
when adequately distended.
The maximum enhancement of the bowel wall is observed between 70 and 85 seconds after intravenous contrast agent administration.
Imaging findings/pathology. Crohn’s disease is classified as primarily active inflammatory,
penetrating or fibrostenotic disease.
Penetrating disease is characterized by presence of fistulas and/or abscesses while in fibrostenotic disease stricturing is seen.
It is most crucial to remember,
that multiple stages of the disease may coexist in the same patient or even in the same bowel segment.
Diagnostic criteria of active inflammation include:
1.
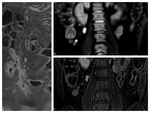
Wall thickening-submucosal oedema.
Wall thickening (between 3 to 12 mm) is usually associated with luminal stenosis.
See: Fig.
3,
Fig.
5 and Fig.
6. Remember: use of fat saturation in one of T2-weighted sequences allows differentiation between submucosal fat and oedema,
both bright on T2-weighted images.
2.
Mucosal hyperenhancement on T1-weighted post-contrast images in reference to adjacent bowel loops,
with or without wall thickening.
See: Fig.
3d,
Fig.
5cg,
Fig.
6e.
3.
Stratified (layered) appearance of active inflammatory lesions on fat-suppressed T1-weighted post-contrast images due to mucosal and serosal hyperenhancement accompanied by submucosal oedema.
According to some authors transmural enhancement without stratification is more common in early stages of CD and in paediatric population whereas the stratified appearance is associated with long-standing disease.
See: Fig.
7.
4.
Mural diffusion restriction.
Persistent high signal on DWI with corresponding low signal on ADC map.
See: Fig.
3ef,
Fig.
5ef,
Fig.
6bc.
5.
Increased mesenteric vascularity adjacent to the inflamed bowel loop - “comb sign” - resulting from engorged vasa recta.
See: Fig.
8.
6.
Mesenteric lymphadenopathy.
Prominent reactive enhancing mesenteric nodes up to 8 mm in short axis diameter may be present.
See: Fig.
9.
7.
Signs of penetrating disease:
- Transmural inflammation.
See: Fig.
7cf.
- Formation of fistulas between an actively inflamed segment of the bowel and other loops of both small and large intestine,
the urinary bladder and/or the skin.
A stellate arrangement of small bowel loops is often seen in case of enteroenteric fistulas - “star sign” - Fig.
10.
An enterovesical fistula is characterized by focal urinary bladder wall thickening at the site of the contact with the inflamed bowel loop - Fig.
11; gas may be present in the bladder.
In up to 36% of patients with CD anal and perinanal fistulas may be encountered - Fig.
12.
Remember: in case of an obstructing stricture distal to a fistula,
the latter is unlikely to close as long as the stricture persists.
- Presence of abscesses.
Abscesses are typically located adjacent to the inflamed bowel loop or are connected to it by a sinus tract.
See: Fig.
10.
Restriction of diffusion in seen in DWI sequences and on Apparent Diffusion Coefficient (ADC) maps.
8.
Mesenteric fibrofatty proliferation - “creeping fat”.
A mass effect caused by proliferation of mesenteric fat resulting in displacement of intra-abdominal viscerae or vascular structures,
usually asymmetric.
See: Fig.7g.
9.
Additional secondary findings: oedema,
free fluid (Fig.
13) and
enhancement in the surrounding soft tissues (Fig.
7c).
Diagnostic signs of chronic inflammation - fibrostenotic disease (Fig.
14),
include:
1.
Mural fibrosis.
See: Fig 14 ab.
2.
Stricture formation - fixed segments of narrowing that may be accompanied by mural thickening show low signal intensity on both T1- and T2-weighted images,
lack of oedema and hyperaemia,
enhance less than active inflammatory lesions.
See: Fig.
15.
Pre-stenotic bowel dilatation (small bowel diameter > 30 mm) may indicate pending obstruction.
With asymmetric bowel wall involvement,
pseudosacculation can occur.
Table 3 compares diagnostic features of active and chronic disease in MRE.
|
Table 3.
Comparison of diagnostic signs of active and chronic disease in MRE
(adapted from Griffin et al.
2012 with alterations).
|
|
Sign
|
Active inflammation
(including penetrating disease)
|
Fibrostenotic disease
|
|
Increase in wall thickness.
|
Moderate to big.
|
Mild.
|
|
Wall enhancement.
|
Strong.
|
Mild.
|
|
Stratified mural enhancement.
|
May be present.
|
Variable.
|
|
Mural oedema.
|
Present.
|
Mild/absent.
|
|
Increased mesenteric vascularity - “comb sign”
|
Present.
|
Absent.
|
|
Mesenteric lymphadenopathy.
|
Present.
|
Absent.
|
|
Phlegmon / abscess.
|
Present in penetrating disease.
|
Absent.
|
|
Formation of fistulas.
|
Present in penetrating disease.
|
Sometimes present.
|
|
Restricted diffusion.
|
Present.
|
Less likely.
|
How to optimize you report?
Obtain relevant,
vast clinical data from the referring physician - remember that not all thickened,
hyperenhancing small bowel loops account for CD.
Differential diagnosis for Crohn’s Disease includes: normal collapsed bowel,
which may appear thickened and hyperenhancing,
infectious and ischemic enteritis,
radiation-induced enteritis and vasculitis.
Include the following information in your report: length and location of involved bowel loops,
type of encountered lesions - signs of active inflammation,
penetrating or fibrostenotis disease with focus on presence/absence of bowel obstruction and extramural complications (fistulas/abscesses).