At the present,
mammography,
ultrasonography and magnetic resonance imaging are the imaging modalities used in the detection,
evaluation and staging of breast cancers [1].
All of them have specific indications and each modality has its own advantages and limitations.
ILC is characterized by its polymorphism on both,
mammography and ultrasound.
One particularity of ILC is that it can be easily missed on mammographic examination,
since it is commonly not seen on either of the two standard views [1].
The rate of false-negative results was reported in the range of 19-43% [6].
Most frequently,
on mammography ILC appears as an area of increased density or an asymmetric density,
with spiculated or ill-defined margins [1,7].
Round and circumscribed masses are less common.
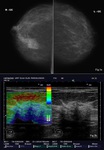
A subtle distortion of parenchyma architecture is the second most common manifestation (Fig.3a) [1].
Microcalcifications are a rare feature in this type of breast cancer [1,7,8].
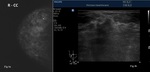
Also,
there are situations when ILC can pass unnoticed,
mainly in the dense breast (Fig.4a) [1].
Compared to mammography,
ultrasound (US) has a higher sensitivity in the detection of ILC.
It is also superior to mammography in identifying multicentricity and multifocality and reflects more accurately the size of a mass than does mammography or clinical examination [1].
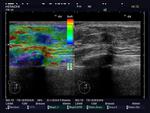
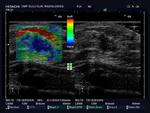
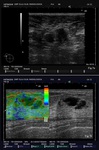
On US,
ILC appears as an irregular mass with hypoechoic and heterogeneous internal echoes,
with ill-defined or spiculated margins and posterior acoustic shadowing (Fig.1,
Fig.2,
Fig.4b,
Fig.5).
Less common it appears as a circumscribed lesion,
as a focal shadowing without a distinct mass (Fig.3b) or it can be sonographically occult [1,8].
Elastography increases the sensitivity and specificity of the diagnosis in the cases where ILC appears as a probably benign lesion,
or in which the findings are subtle or nonspecific.
In these cases,
based on the elastic tissue properties,
elastography allows a more precise characterization of suspicious areas,
a better differential diagnosis and a better management of the patients.
Elastography,
like any other examination,
has a rate of false positive and false negative results (Fig.5).
The elastographic score alone is only a descriptor as any other characteristics described when analyzing a breast lesion (borders,
growth pattern,
structure,
etc),
and should be constantly interpreted together with the B-mode and Doppler ultrasound findings.
The final assessment and management of the cases should be based on the most suspicious findings.