Findings and procedure details
Planning prior to ablation is usually made with CT angiogram.
1.- Technique
A.- CT angiogram.
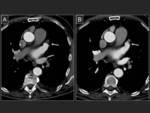
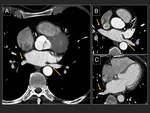
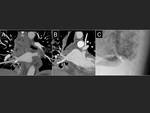
Acquisition for pulmonary veins study can be performed with prospective or retrospective synchronization,
or with no synchronization (8).
The main hindrance to retrospective synchronization is the high radiation dose administered to the patient.
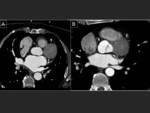
This dose can be reduced by lowering the kilovoltage (5,
9) Fig. 8
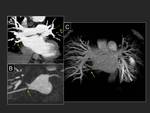
Non-synchronized acquisitions allow less radiation to the patient,
but have limitations of its own (8).
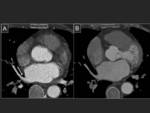
When heart rate is over 100 bpm,
non-synchronized acquisitions can be performed.
Fig. 9
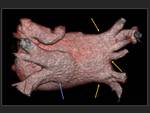
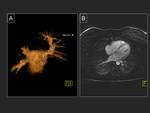
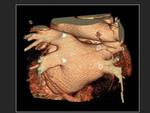
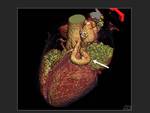
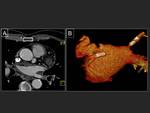
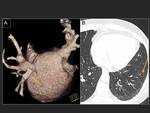
Volume rendering reconstructions are very useful to evaluate the number and position of the pulmonary veins.
Fig. 10 .
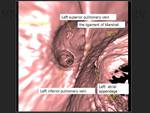
Virtual navigation can also be an useful tool to study the pulmonary veins.
Fig. 11
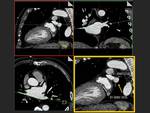
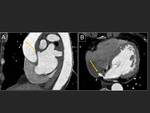
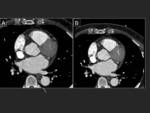
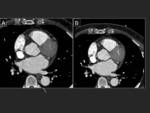
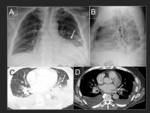
One of the goals of CT is to rule out the presence of thrombi in the left atrium,
especially in the auricle.
A late acquisition can confirm or exclude the presence of a thrombus in the auricle.
Fig. 12
At our center,
we adjust the contrast medium dose to the weight of each patient.
We Use Iomeron 300 mg/ml with a flow of 4-5 ml/s,
and bolus tracking technique.
When we perform retrospective acquisition,
we utilize 80 Kv in patients under 80 Kg,
and 100 Kv in patients over 80 Kg,
according to published data.
(9)
B.
MRI
Pulmonary veins can also be studied with MRI.
However,
many of the patients with AF also carry pacemakers,
which reduces MRI actual use.
(10) Fig. 13
2.- Anatomy.
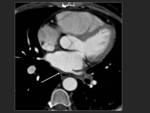
CT or MRI studies prior to the ablation procedure allow to know the anatomy of the pulmonary veins,
identify the location and measure the diameter of the ostia and its proximity to the esophagus.
Fig. 14
This references are valuable afterwards to rule out some complications,
such as venous stenosis or esophagic lesions.
Fig. 15
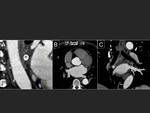
In 60-70% of patients four pulmonary veins are found.
Left pulmonary veins run into a common confluent more often than the right veins (8% vs 0.7 %)(8,11).
Fig. 16
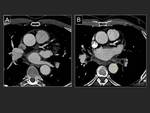
The left inferior pulmonary vein ostium is the smaller one.
This vein grows narrower as it approaches the ostium.
The rest of the pulmonary veins suffer the opposite phenomenon.
Right veins are usually larger than the left ones.
(12) Fig. 17
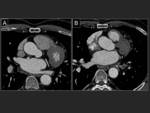
The most frequent variant is the right middle lobe and the right upper lobe running independently,
with two separate ostia .(Fig 10).
(11).
Atrial diverticuli are a variant as frequent in AF patient as in healthy subjects,
and it is not associated with a worse outcome of the ablation.
Nevertheless,
it remains uncertain if around the diverticuli,
like around the veins,
ectopic foci exist.
(8) Fig. 18
One aspect to be taken into account,
is the identification of congenital or acquired anomalies of pulmonary venous drainage.
Fig. 19
Eventually during planification studies some other congenital cardiac or coronary anomalies are discovered,
that may have impact in the procedure planification.
(13) Fig. 20
3.- Complications.
Ablation entails a reduced risk of complications that may be severe in 1.4-6% of studies,
and involve radiologists not familiarized with the procedure.
(6).
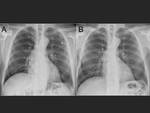
Patient follow-up after the procedure is usually performed in most centers with echocardiogram and plain chest radiographs.
Complications arisen from ablation may involve general radiologists not used to this procedure.
CT is useful when some complications such as pulmonary veins stenosis or atrio-esophageal fistula are suspected.
The most frequently observed complications after the procedure involve the vascular access.
(6).
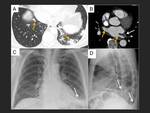
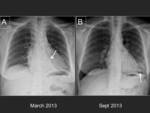
A.- Pulmonary veins stenosis
Its incidence ranges from 1 to 10%.
Symptoms can take months to develop (3).
Fig. 21 .
If severe,
it can produce a complete occlusion of the pulmonary veins.
It can be treated through dilation and stent placement.
The left inferior pulmonary vein requires special attention,
since its usually narrower than the rest.
CT angiogram overestimates the pulmonary veins stenosis.
When a complete occlusion is observed in the CT angiogram,
an angioplasty or stent placement should not be excluded.
( Fig. 22 ,
Fig. 23 ,
Fig. 24 ,
Fig. 25 ,
Fig. 26 ,
Fig. 27 ,
Fig. 28 )(14).
B.-Neural lesions
Gastroparesis secondary to a vagus nerve lesion is an infrequent complication.
Its incidence is low (0,
29%).
(15) Fig. 29 .
Esophageal temperature monitoring can reduce the risk of vagus nerve lesions (15).
The incidence of phrenic nerve lesions in this context is also low (0,
48%) Fig. 30 (3).
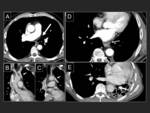
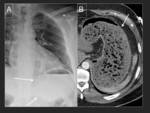
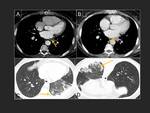
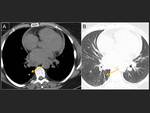
C.-Lung alterations
Pneumonias have been described (16,17) Fig. 31 y Fig. 35 ),
as well as pulmonary haemorrhages (18) and venous infarctions (19) (Figures Fig. 31 ,
Fig. 32 ,
Fig. 33 ,
Fig. 34 ,
Fig. 35 ) as complications after left atrial ablation.
The most severe one is the lung infarction secondary to venous thrombosis.
In patients treated with left atrial ablation,
with a chest radiograph suggestive of pneumonia,
it is convenient to perform a CT angiogram to rule out stenosis,
occlusion or injury of the pulmonary veins.
D.-Esophageal lesions
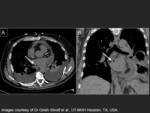
After the ablation the esophagus can suffer tearings,
perforation or an atrio-esophageal fistula.
It is not completely known how the radiofrequency energy propagates to surrounding organs.
Sometimes,
the energy administered to the posterior area of the atrium can cause lethal atrio-esophageal fistulas complication that usually occurs from 2 to 3 weeks after the intervention.
(27).
Fig. 36
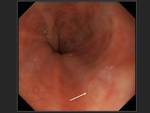
Tearings are described in up to 11% of patients treated with ablation,
and are diagnosed by means of endoscopy.
(22) Fig. 37
The incidence of atrio-esophageal fistula is 0.07% and has a high mortality.
CT is the technique of choice to perform the diagnosis.
The main sign consist in the identification of bubbles within the left atrium.
In the patients studied in our series,
no cases have been reported.
(3,
23)
When esophageal injury occurs,
the alert symptom is dysphagia.
However,
patients may remain without any symptom for weeks.
(3,
23 ).
In some centers,
ice-cold water irrigation is performed during the procedure,
and it seems to relieve the symptoms,
but it has no proven preventive effect on esophageal lesions.
(23)
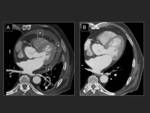
E.-Cardiac lesions
Pericardial effusion after the right atrium ablation can range from mild to cardiac tampone.
Cardiac tampone is the most frequent complication in some series (1.3%) (24).
It can develop during the procedure,
in which case the radiologist doesn’t take any part,
but also delayed up to 45 days after.
(25).
Fig. 38
Cardiac MRI can reveal scars in the left atrium in patients treated with ablation.
(26).
F.-Strokes
The risk of stroke varies between 0,1 and 1,4% in this group of patients.
It is caused by the thrombogenic effect of the electro-catheters,
the damage to the vascular and cardiac endothelium,
and the direct activation of the coagulation and platelet production due to the manipulation of the atrium.
(3).
Luckily we haven’t found any case in our series.
G.- Hematomas
To prevent strokes patients are administered anticoagulants before and after the procedure,
and heparin while it is being carried out the intervention.
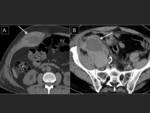
Complications arisen from anticoagulation include intracranial,
retroperitoneal,
muscular and gastro-intestinal bleeding (3) Fig. 39
Other complications are embolization of materials used during the intervention.
Fig. 40