Acute mediastinitis refers to inflammation of the tissues that surround the mediastinal structures.
According to their most frequent etiology,
it can be divided into three entities: postoperative,
esophageal perforation and descending necrotizing mediastintis.
Mediatinitis suspicion is based on various clinical criteria: chest pain,
fever-sepsis,
purulent secretion from the sternal injury for postoperative patients, leucocytosis or neck swelling.
The initial radiological test includes radiographic studies.
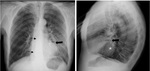
Radiological findings in conventional radiology can guide us and confirm the suspicion of mediastinitis,
and include the widening of the mediastinum, neumomediastino, aditional pleural findings,
soft tissue mass,
air-fluid level (Fig 1 and 2) and broken or displaced sternotomy sutures in postoperative patients.
But CT techniques are generally required and are highly sensitive to confirm the diagnosis,
evaluation of the site and extent of mediastinal involvement and the probable etiology.
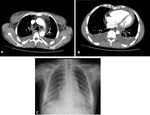
The most frequent signs of mediastinitis in CT are: localized mediastinal fluid, pneumomediastinum, mediastinal edema with infiltrative region of soft-tissue attenuation which obliterates normal mediastinal fat planes and encases or invades adjacent structures, lymphadenopathy,
pleural effusion,
or a sternal or lung abnormality (Fig.
1).
POSTOPERATIVE MEDIASTINITIS
It is the most frequent etiology of mediastinitis,
mainly after sternotomy following cardiac revascularization surgery with both internal mammary arteries,
with an incidence of 0.4% to 5% and a mortality of 16.5% to 47%.
The radiological findings that suggest this etiology are sternal dehiscence, peristernal abnormalities such as edema of soft tissues,
separation of sternal segments with marginal bone resorption,
sclerosis and osteomyelitis.
ESOPHAGEAL PERFORATION
It is the second most frequent cause of acute mediastinitis,
produced by oropharingeal flora,
with a mortality of 20% to 60%,
depending on the time of diagnosis.
Most of esophageal perforations are iatrogenic and most of these occur during endoscopy.
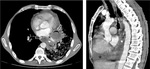
The signs that can guide us to the etiology are the thickening of the wall, periesophageal fluid collections,
pneumothorax or hydropneumothorax and especially the extravasation of contrast after an oral administration (Fig.
2 and 3).
DESCENDING NECROTIZING MEDIASTINITIS
The most common etiology is odontogenic infection,
followed by retropharyngeal and peritonsillar abscess,
less frequent cervical injuries,
neck surgery,
trauma, parotitis, thyroiditis and clavicular osteomyelitis.
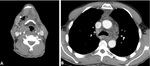
CT can reveals subcutaneous emphysema,
pleural empyema and pericardial effusion (Fig.
4).