COMMON ULTRASOUND FINDINGS IN MUSCULOSKELETAL PATHOLOGY
ACHILLES TENDON
Although Achilles tendon (AT) is the strongest tendon in the human body,
it is among the most frequently injured ankle tendon.
A relative avascular zone,
located 2-6 cms from the calcaneal insertion,
is typically the site of pathologic findings,
followed by the musculotendinous junction.
Pathology can be acute or chronic and range from mild peritenonitis to full-thickness tendon rupture.
AT conditions are common and often come to clinical attention as acute lesions.
ANATOMY
- Achilles tendon (AT) extends from the musculotendinous junctions of medial,
lateral heads of the gastrocnemius and soleus muscles,
to the site of its insertion in the posterior surface of the calcaneus.
The two heads of the gastrocnemius muscle mix together approximately 15 cm above the calcaneus,
forming the AT as they descend.
- The tendon of the Soleus muscle fuses with the gastrocnemius component of the Achilles approximately 5-6 cm above the calcaneal insertion.
- An important aspect of AT is that it has no synovial sheet,
being instead encased in a connective tissue membrane (paratenon or peritenon) that aids tendon glide and supports vasculature.
Proximally,
the paratenon continues with the fascia of the gastrocnemius muscle.
SONOGRAPHIC ANATOMY
- Well defined fibrillary tendon pattern
- Average thickness is 6mm; it can be thicker in men and in tall patients.
- AT gets broader and flatter distally,near its insertion on the calcaneus.
- AT size is related to body mass.
So the bigger the body mass,
the biggert the AT.
- AT its outlined by a hypoechoic border (paratenon).
- No Color Doppler Flow in normal tendon and paratenon.
- Normal movement of AT con be demonstrated using dynamic examination.
- On axial images AT has a typical punctuated pattern.
ACHILLES TENDON LESION
PARTIAL TEAR
- Enlargement of AT (>1 cm) in the anterior-posterior dimension.
- Intrinsic tendon abnormalities,
like hypoechoic or anechoic areas,
with associated tendinosis of adjacent fibers.
- Discontinuity in one portion of the tendon fibers.
- Focal thinning of the tendon.
- Focal increased Doppler signal
- Dynamic examination demonstrates continuity of the tendon.
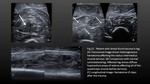
FULL THICKNESS TEARS Fig. 2,Fig. 3,
Fig. 4,
Fig. 5,
Fig. 6
- Complete tendon fibre disruption
- Separation and retraction of the torn ends,
with tension loss of the tendon and a gap formation.
- Herniation of the Kager's fat (pre Achilles fat pad) into the gap.
- Refraction artifact,
with posterior shadowing from the torn ends
- Fluid collection filling the gap in acute-subacute phases (hematoma).
- In sub-acute and chronic phases,
the gap may be filled with debris and organizing hematoma that may have variable ultrasound appearance.
- The plantaris muscle tendon can occupy the resulting gap in a complete AT rupture,
leading to misinterpretation of a complete AT tear as a partial tear.
Therefore identification of the plantaris tendon is of importance while evaluating AT tears.
PRE TREATMENT APPROACH
- Estimate the size of the gap and determine the exact level of the tear; most surgeons would elect not to repair a rupture within the musculotendinous junction.
- Identification the plantaris tendon that may be used as a graft in some of the surgical procedures.
PATELLAR TENDON
NORMAL ANATOMY Fig. 7
· The extensor mechanism of the knee is composed by:
- Quadriceps muscle
- Quadriceps tendon
- Medial and lateral retinaculum
- Patella
- Patellar tendon
- Tibial tuberosity
- Patellar tendon is part of the extensor mechanism of the knee,
and goes from the inferior pole of the patella to the tibial tuberosity·
- It appears on sonography as a cylindric structure with homogeneous,
low to moderate echogenicity.
- Its insertions are easily located by bony acoustic shadowing.
- The sonographic appearance of the tendon may vary because of anisotropy.
- Normal tendon measures vary from 3-6 mm in anteroposterior thickness,
and 10-15 mm in lateral dimensions.
PATELLAR TENDON TEAR Fig. 8, Fig. 9
- Patellar tendon (PT) rupture is a relatively infrequent injury,
seen in younger patients (less than 40 years of age).
- Indirect mechanism is the most common,
and is the result from forced flexion with a contracted cuadriceps.
- Predisposing factors include:
- Chronic tendinopathy (repetitive microtrauma to the patellar tendon),
also known as jumper’s knee.
Most ruptures occur over degenerated tendons.
- Steroids injection
- Associated systemic illness (systemic lupus erythemtosus,
renal failure,
diabetes mellitus,
rheumatoid arthritis)
- It can occur at either the patellar or tibial insertion of the patellar tendon.
- The superior attachment to the inferior pole of the patella is the most frequent place of lesion.
- Intra substance tears are common in patients with associated systemic illness
- Small avulsion fractures are common.
PRE TREATMENT APPROACH
- Non surgical treatment has limited role in the management of patellar tendon ruptures.
- Prognosis is better if the repair is performed early after the injury,
so accurate sonographic diagnose is important.
- Sonography can asses alterations in adjacent anatomical structures,
like foreign bodies,
bursitis and hematomas.
- Patients who undergo delayed repair have greater risk of loss of full knee flexion and decreased quadriceps strength.
QUADRICEPS TENDON OF THE KNEE
NORMAL ANATOMY Fig. 10
- Part of the extensor mechanism
- Composed of tendinous contributions from four separate muscle bellies which join in the midline:
- The three vastus muscles (medialis,
lateralis and intermedius).
- Rectus femoris
- QT inserts onto the superior pole of the patella.
- The normal tendon has a hyperechoic,
organized fibrillar appearance that can be easily followed from the musculotendinous junction of the quadriceps to the superior pole of the patella
- Normal diameter of the QT usually ranges from 6 to 11mm thick.
QUADRICEPS TENDON RUPTURE Fig. 11, Fig. 12
- Ultrasound has a high sensitivity and specificity to determine the exact location of a tear,
and can distinguish between partial and complete ruptures.
- Because of its cost,
MR should be reserved for complicated cases in which other diagnostic methods have failed to give accurate information.
- Rupture of the quadriceps tendon is more common in the elderly and patients with systemic disease,
as opposed to patellar tendon rupture,
which is more common in younger patients (sports-related lesion).
- QT ruptures can be traumatic,
idiopathic or associated to systemic diseases.
- Complete rupture of the QT can often be diagnosed clinically (loss of active leg extension and a suprapatellar depression).
- Partial tears are more difficult to detect since function can be maintained.
- Misdiagnosis can be as high as 50%,
because the physical examination is often limited by pain and swelling,
and partial ruptures can be missed.
- Differentiation between partial and complete tears is crucial to plan treatment; partial tears usually don’t require surgery,
whereas complete tears do.
- Ultrasound can differentiate complete from partial tears.
COMPLETE TEAR
- Complete discontinuity of tendon fibers with formation of an anechoic-hipoechoycic gap (hematoma) and retraction of the tendon ends.
- Longitudinal plane is useful to assess tendon discontinuity,
gap diameter and retraction.
- Associated patellar upper pole fracture is not infrequent and bone fragments can be seen as hyperechogenic structures with posterior shadowing.
PRE TREATMENT APPROACH
- Incomplete tears are usually treated conservatively,
and treatment should be started immediately after a complete tear has been discarded.
- Conservative treatment of complete ruptures has poor results,
with progressive weakness and disability; therefore,
complete tears must be identified as fast as possible.
- Ultrasound can give an accurate and fast diagnosis,
allowing an early surgical treatment.
- If surgery is delayed,
the repair procedure is complicated,
and results may be less satisfactory.
DISTAL BICEPS TENDON
NORMAL ANATOMY
- The biceps tendon forms about 7 cms above the elbow,
and descends as a flat structure.
- Unlike other tendons,
biceps tendon has a long segment that is not surrounded by muscle,
making it more susceptible to injury.
- It inserts on the radial tuberosity,
expanding at its attachment.
- It also attach to the bicipital aponeurosis (or lacertus fibrosus),
a fibrous membrane that helps the tendon keeping its normal position.
DISTAL BICEPS TENDON RUPTURE Fig. 13, Fig. 14
- Distal biceps tendon rupture is the most common tendon tear of the elbow.
- However,
it is an uncommon injury,
representing 3 % of all biceps ruptures.
- Complete tears are usually in relation with a traumatic event with forced extension against an elbow in midflexion,
like when lifting a heavy object.
- Preexisting degeneration in the tendon may precipitate ruptures associated with minor trauma or without trauma at all.
- Typically,
the tendon tears from its attachment on the radial tuberosity,
but can be found anywhere along the tendon.
Most tears occur 1-2 cms above the radius,
in an area of relative hypovascularity.
- Less common sites of rupture include muscle belly and musculotendinous junction
- If bicipital aponeurosis remains intact,
clinical diagnoses is difficult since flexion strength may be preserved.
- Sonographic findings of complete tears include:
- Absence of the tendon in its normal location,
coursing distally to the radial tuberosity.
- Fluid filled tendon gap,
with retracted ends.
- Mass in the antecubital fossa (tendon stump).
- Dynamic imaging can be used to confirm continuity of the tendon.
- Partial tears may show increase in the caliber of the tendon and an abnormal contour.
- Peritendinous fluid as an isolated finding is not a reliable sign,
since it can be secondary to tenosynovitis alone.
PRE TREATMENT APPROACH
- Early surgical repair is the treatment of choice for complete ruptures
- In complete tears,
ultrasound can show tendon localization,
gap size and fluid collections,
and it might be the only imaging technique needed to plan surgery.
- MRI can be preserved as a second examination in cases in wich sonographic findings are doubtful or visualization is suboptimal.
- Partial tears are usually treated conservatively,
and local steroid or analgesics injections can relief symptoms.
PLANTAR PLATE
NORMAL ANATOMY Fig. 15
- Fibrocartilaginous structure located on the plantar aspects of the metatarsophalangeal joint,
just under the metatarsal head.
- Distally the plantar plate inserts into the bone of the proximal phalanx
- Plantar plate principal functions are:
- It is the main structure for the MTP joint stability.
- Resist hyperextension of the metatarsophalangeal joint,
and provides support during ambulation.
- Reduces load on MTP joints.
- Serves as a point of attachment for distal part of plantar fascia.
- Plantar plate thickness varies from 2-5mm and its width from 8-13mm.
PLANTAR PLATE RUPTURE Fig. 16, Fig. 17
- The second metatarsophalangeal joint is the most vulnerable place for plantar plate lesions (largest plantar plate) although it can occur in any of the MTP joints.
- Repetitive microtrauma can lead to chronic plantar plate disruption.
- Plantar plate rupture can be a cause of acute matatarsalgia.
Acute injury tends to occur from sudden and excessive upwards motion of the toe,
with sudden pain and inflammation.
- If not treated,
toe deformation can develop.
- Predisposing factors include:
- Use of high heels that shift the body’s weight onto MTP joints
- Narrow shoes
- Hallux valgus deformity
- Long second ray
- Athletes
- Subluxation of the MTP joint may be seen at physical examination,
and patients may refer sensation of instability.
- Intense pain on palpation in the plantar area of the metatarsal head is suggestive of acute degeneration of the plantar plate.
- Most tears occur at the distal insertion in the proximal phalanx
MAIN FINDINGS
- Plantar plate discontinuity
- Loss of normal hyperechoic appearance,
with focal hypo or anechoic defects.
- Plantar plate may appear thickened,
as a sign of degeneration.
- Flexor tendon may be dislocated (if full-thickness tear)
- MRI findings
- Increased signal intensity on T2-weighted images.
- Discontinuity of the plate
- MTP joint synovitis
- Hyperextension of the proximal phalanx.
TREATMENT APPROACH
- Conservative treatment is made with relative rest,
padding and protection of specific pressure points,
orthoses and special stiff soled shoes.
- Surgery is indicated if conservative therapy fails to improve symptoms.
- Early diagnosis is important to initiate proper treatment,
whereas is conservative or surgery.
ROTATOR CUFF
- Acute/subacute trauma is an important cause of rotator cuff lesions.
- Other causes include chronic and repetitive trauma,
subacromial impingement and tendon degeneration.
ROTATOR CUFF COMPONENTS
- Tendons
-
- Supraspinatus
- Infraspinatus

- Teres minor
- Subscapularis
- Joint capsule
- Coracohumeral ligamnet
- Glenohumeral ligaments
Ultrasound examination of the shoulder must have an order not to miss any structure:
- Long head of the biceps tendon (not part of the rotator cuff)
- Supraspinatus tendon
- Infraspinatus tendon
- Subscapularis
- Glenohumeral and acromioclavicular joint
ANATOMY
LONG HEAD OF THE BICEPS TENDON
- The bicipital tendon can be identified using the lesser and greater tuberosities as landmarks; it is seen as a hyperechogenic structure in the bicipital groove (axial plane).
- There can be a minimal physiologic amount of fluid surrounding the tendon.
- It originates in the superior glenoid labrum,
and goes through the rotator interval.
SUBSCAPULARIS TENDON
- It originates in the anterior aspect of the scapular bone (subscapularis fossa).
- Inserts in the lesser tubercle of the humerus.
- Best seen with the shoulder externally rotated.
- It is seen as a fibrillar hyperechoic structure.
- Interposed muscle fibers can be seen as hypoechoic clefts (mainly in axial plane) that can be mistaken for areas of tendinosis.
SUPRAESPINATUS TENDON Fig. 18
- It originates from the suprascapular fossa,
and inserts in the greater tuberosity.
- Best seen with the shoulder internally rotated (hand behind back position).
- The fibrillar hyperechogenic structure of the tendon is seen under the subacromial bursa.
- It appears as a uniformly echogenic structure and sharpens until its insertion in the greater tuberosity.
- The humeral head is visible below the tendon (hyperchoic structure with posterior bony shadow),
covered by the articular cartilage (hypoechoic layer).
INFRASPINATUS TENDON
- Infraspinatus originates (along with teres minor) from the dorsal aspect of the scapular bone,
inferior to its spine.
- It inserts in the greater tuberosity of the humerus.
- Best seen from the posterior aspect of the shoulder,
with the hand resting on the opposite shoulder.
- The spine of the scapula can be used as a land mark to differentiate the infraspinous fossa.
- The tendon is seen as a beak shaped hyperechogenic structure located under the deltoid muscle,
and running over the posterior humeral head.
ROTATOR CUFF LESIONS Fig. 19, Fig. 20, Fig. 21
TENDINOSIS
- Rotator cuff tendinosis is more frequent in the supraspinatus tendon.
- Normal tendon has a homogeneous appearance.
- Abnormal tendon may appear with heterogeneous echotexture · Thickening or thinning of the tendon may be seen.
PARTIAL THICKNESS TEARS
·
- Signs of partial tear include hypoechoic or anechoic defects and tendon flattening ·
- Can be classified into bursal surface,
articular surface and intra substance tears.
·
- Articular surface tears are more common,
and can associate irregularities of the underlying cortical bone.
- Partial tears can be seen as focal thinning or bursal depressions.
- Continuous fibers can be seen inserting in the greater tuberosity.
FULL THICKNESS TEARS
- The main finding in a full thickness tear is a defect that extends from the joint side to the bursal side of the tendon,
visualized in both,
short and long axis.
- If filled by fluid,
the defect can be easily identified.
- The anterior third of the supraspinatus tendon is the most affected location,
due to the presence of a relatively hypovascular area.
- Full thickness and full width tears are known as complete tears.
- Complete and massive tears can produce tendon retraction,
leaving the humeral head and grater tuberosity naked (non visualization of the rotator cuff).
- Indirect signs of complete tear include:
- Fluid in the subdeltoid bursa and gleno-humeral joint.
- Tuberosity hyperostosis (tendon enthesis abnormalities).
- Clear visualization of the cartilage beneath due to sound attenuation through the tear (uncovered cartilage sign).
- Alterations on the contour of the tendon are not particularly useful,
but can help in the diagnosis of a full thickness tear (upper concavity at the level of the tear).
- Massive tears affect the supraspinatus tendon,
extending to the subscapularis and the infraspinatus tendons.
ACUTE VS CHRONIC TEARS
- Small percentage of patients.
- Acute onset of symptoms,
usually with history of a traumatic event.
- If physical examination and plain radiographs are not clear about the cronicity of the tear,
ultrasound can help differentiate acute from chronic tears.
- Midsubstance location of the tear suggests an acute tear.
- Joint and bursal fluid is more common in acute tears.
- Non visualization of the rotator cuff is most frequently associated with chronic tears.
- Acute tears have more delimitated ends,
so the size of the tear can be measured more accurately.
- Acute tear is an indication for early surgical procedure; chronic changes make repair more technically difficult.
PROXIMAL BICEPS TENDON
- Small amounts of fluid surrounding the tendon can be a normal finding.
- Large amounts of fluid,
in association with thickening of the tendon can be in relation with tendinosis.
It may also indicate a rotator cuff tear.
- Non visualization of the tendon in the grove:
- Ruptured tendon with retraction of its borders o
- Medial dislocation of the tendon.
- Medial luxation may coexist with a subscapularis tendon tear.
- Physical examination is very important to asses a long head of the biceps tendon rupture.
- The most common site of rupture is its superior labrum attachment.
- Associated rotator cuff tears are common in chronic ruptures.
- Acute ruptures can be seen in traumatic events.
OTHER CONDITIONS
MUSCULAR TRAUMA
- Normal skeletal muscle is organized into fascicles contained within a sheet of connective tissue.
This gives the normal ultrasound appearance of muscle,
with hypoechoic and hyperechoic stripes.
- Muscle injuries are usually the result of sports related trauma.
- Ultrasound findings include:
- Disruption and discontinuity of muscle fascicles.
- Hypervascularity of the muscle surrounding a tear or hematoma.
- Hematomas can appear as echogenic masses on acute traumas.
Fig. 22
- In the subacute setting,
hematomas can be heterogeneous,
with hyperechoic debris.
- Muscle bellies may appear with hyperechoic edematous areas.
- Ultrasound guided aspiration can be perform,
and can result in faster recovery.
- If complete disruption of muscle belly occurs,
there usually is some degree of muscle retraction.
COLLATERAL LIGAMENTS OF THE THUMB Fig. 23, Fig. 24
- Ulnar collateral ligament is visualized as a compact structure in the ulnar aspect of the thumb.
- When injured,
the ligament may appear thickened and elongated.
- There can be associated avulsion fractures.
The bony cortex should be evaluated.
- Stener lesion is characterized by interposition of the aponeurosis of the adductor pollicis muscle between the ruptured ulnar collateral ligament of the thumb and its site of insertion at the base of the proximal phalanx.
This prevents healing,
and is an indication of surgical repair.
- Radial collateral ligament tear ussually does not require surgical treatment.
FINGER TENDON INJURIES Fig. 25, Fig. 26
- Injuries to finger tendons are common emergency.
- Acute injuries are difficult to diagnose clinically due to pain and swelling.
- Ultrasound can help determine if there is a complete tear of flexor or extensor tendons.
MUSCULAR HERNIAS Fig. 27
- Muscular hernias are usually found in lower extremities.
- There is a facial defect with protrusion is the muscle trough the defect.
- Muscle hernias are usually asymptomatic,
but can produce pain during activity.
- Ultrasound is the modality of choice for evaluating this hernias.
- Ultrasound findings include:
- Focal thinning and subtle elevation of the fascia.
- Clear fascial defect with protruding muscle.
The protruded muscle adopts a mushroom like appearance
- Muscle herniation can be intermittent.
- Ultrasound findings of muscular hernias can be very subtle,
and is important not to apply much pressure to avoid reduction of the hernia.
FRACTURES Fig. 28, Fig. 36
- Fractures are common lesions,
especially in children.
- Ultrasound has emerged as a new modality for fractures diagnoses.
- Intact bone appears a smooth and uniform hyperechoic structure.
- Bones should be imaged in both long and short axes.
- Fractures appear as a cortical defect in ultrasound images.
- Numerous studies have shown very good results in ultrasound diagnosed fractures,
especially in children.
- There appear to be a better rib fracture diagnoses with ultrasound than with plain radiographs.
INFECTIOUS PATOLOGY
- Infections are common in medical practice.
- Early treatment is very important in order to prevent sequelae; hence the importance of a fast diagnosis.
- Ultrasound is very sensitive in the detection of joint and extracapsular fluid collections.
- It can be used to perform guided aspirations,
confirming in real time changes in effusion changes.
- Ultraosund is very cost-effective,
and it’s widely available.
PYOMYOSITIS Fig. 29, Fig. 30
- Rare infection of the muscle.
- Common in tropical regions.
- Immunosuppressed patients have higher risk of develop this kind of infection.
- Staphylococcus aureus is the most common micro-organism involved.
- Ultrasound findings include:
- Intramuscular abscess formation visualized as a fluid collection.
It may appear hypo,
hyper or isoechoic.
- Altered muscle echogenicity with hypoechoic areas of edema peripheral to the abscess.
- Air presence within the edematous muscle or abscess is suggestive of anaerobic bacteria infection.
OSTEOMYELITIS Fig. 31, Fig. 32
- Acute osteomyeilitis with haematogenous origin most commonly occurs in children and older persons.
- Staphylococus aureus is the most common organism involved.
- Ultrasound is frequently used for the diagnosis of osteomyelitis,
specially in children.
- A negative ultrasound does not exclude the diagnosis; ultrasound cannot see beyond bone cortex.
- Ultrasound findings of osteomyelitis usually precede radiographic manifestations,
and include:
- Periosteal thickening; elevation of the periosteum greater than 2mm is indicative of subperiosteal abscess formation.
It usually appears as a spindle shaped fluid collection adjacent to the bone cortex.
- Swelling of adjacent muscle and subcutaneous tissue.
- In more advanced stages,
cortical defects may be seen.
- Hyperemia may be identified with color Doppler flow as soon as 4 days after onset of symptoms.
- Ultrasound can be perform for monitoring progression of articular and soft tissue changes.
- Depending on age,
manifestations of osteomyelitis may vary:
- Epiphyseal infections are more common in infants,
since diaphyseal blood vessels traverse the growth plate.
- Metaphyseal involvement is more common in older children.
- Periosteal elevation is more common in children than adults.
SEPTIC BURSITIS Fig. 33
- Clinical presentation of septic bursitis can be similar to septic arthritis,
with joint pain and swelling.
- Staphylococcus aereus is the most common organism involved.
- Septic bursitis has nonspecific ultrasound findings,
including:
- Fluid filled affected bursa.
The fluid can be hypoechoic or anechoic with hyperechoic internal debris.
- Thickened bursal walls.
- Hyperemia with increased Color Doppler flow in the walls of the fluid collection.
- Ultrasound appearance of the fluid is nonspecific,
and cannot determine reactive versus infectious etiology,
therefore,
aspiration is usually needed to determine the diagnosis.
SEPTIC ARTHRITIS Fig. 34
- The most common form of infectious arthritis.
- It can occur in all ages,
but is more common in chidren.
- The most common mechanism is hematogenous seeding.
- It can also occur after penetrating trauma.
- Bacterial arthiritis can result in joint loss; it needs to be diagnosed and treated as fast as possible.
- S.
aureus is the most common etiologic agent.
- The most affected joint is the knee,
followed by the hip.
- Over 90% of cases are monoarticular.
- Conventional radiographs may be normal or show joint space widening.
- Ultrasound is very sensitive for detecting joint effusion,
but sonographic findings are nonspecific; infected joint effusion cannot be distinguished from simple effusion based on ultrasound characteristics.
- US can be used to guide needle aspiration.
- The ultrasound appearance of the fluid usually is hypoechoic with hyperechoic debris.
- Synovial thickening may be seen.
- Color Doppler flow may be present in the joint capsule,
representing hyperemia.
- MRI images may show altered signal in the adjacent bone marrow.
- Septic arthritis is a surgical emergency; delayed treatment may lead to joint functional loss.
CELLULITIS Fig. 35
- Cellulitis is a diffuse inflammation of the skin and subcutaneous tissue.
- Patients usually present painful and swollen erythema in affected area.
- Ultrasound shows thickened subcutaneous tissue with increased echogenicity.
- Diagnosis is generally based in clinical findings; ultrasound is helpful in follow up,
when patients do not improve with treatment.
- Usual ultrasound findings include:
- Diffuse thickening of skin and subcutaneous tissue.
- Cobblestone appearance with anechoic stripes.
- Hyperemia with increased Color Doppler flow.