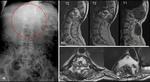
RADIOLOGICAL FINDINGS
Hydatid disease primarily affects the liver and typically demonstrates characteristic imaging findings depending on the stage of cyst growth (whether the cyst is unilocular,
multilocular containing daughter vesicles,
or if partially or completely calcified [dead]).
In radiologic studies the typical findings of hydatid disease are well known,
but unusual imaging characteristics related with its rare complications are less frequently documented in the literature.
It is expected that a complicated hydatid cyst is associated with higher morbidity and mortality.
Therefore,
familiarity with atypical radiological features is very important to prevent misdiagnosis and improper therapeutical management.
Although the liver (75%) and lung (15%) are the most commonly involved organs,
the disease can be seen anywhere in the body (10%)
Unusual locations of hydatid cysts support the hypothesis that beside portal circulation,
the echinococcus embryos can spread via other routes,
such as the lymphatic system,
the biliary tract and/or by dissemination of daughter cysts into peritoneal or other cavities with the rupture of the primary cyst.
Furthermore,
secondary involvement due to hematogenous dissemination may be seen in almost any anatomic location (eg,
lung,
kidney,
spleen,
bone,
brain).
However,
there are many potential local or distant complications (eg,
intrahepatic complications,
exophytic growth,
transdiaphragmatic thoracic involvement,
perforation into hollow viscera,
peritoneal seeding,
biliary communication,
portal vein involvement,
abdominal wall invasion,...).
The diagnosis of hepatic hydatid cysts complications may be established by US,
CT or MRI,
that permit the distinction between intact cysts and those presenting with contained rupture,
as demonstrated by a collapsed endocyst or a globally echogenic appearance.
CT and MR imaging may demonstrate cyst wall discontinuity as well as the passage of contents through the defect.
CT is the modality of choice in peritoneal seeding.
The diagnosis of HHC perforation into the main biliary tree is usually made by detection of a discontinuity in the cyst wall and/or the presence of hydatid material within the biliary system.
Similarly,
direct HHC rupture into different thoracoabdominal spaces is diagnosed by demonstrating cyst wall discontinuity and the presence of hydatid material within these spaces.
Indirect signs of biliary communication include increased echogenicity at US and fluid levels and signal intensity changes at MR imaging.
CT allows precise assessment of osseous lesions,
whereas MR imaging is superior in demonstrating neural involvement.
COMPLICATIONS
In order to classify the complications and atypical manifestations observed in our center,
we will consider on one hand exclusive liver involvement and on the other hand the extension from the liver to other anatomical locations.
Complications of hydatid disease confined to the liver itself (intrahepatic),
will contemplate; superinfection of the cyst, contained rupture of the cyst,
communication with the biliary tree and direct vascular invasion of the portal vein.
For extrahepatic extension,
we consider direct communication to adjacent visceral structures (gallbladder,
colon,
stomach,
right kidney,
lung),
retroperitoneal and peritoneal dissemination (omental,
pouch of Douglas,
...),
and finally hematogenous spread (spleen,
pancreas,
pulmonary artery,
bone,...).
1- INTRAHEPATIC COMPLICATIONS (LOCAL COMPLICATIONS)
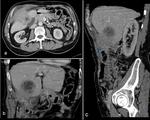
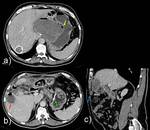
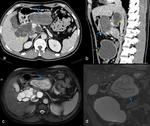
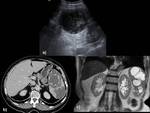
1a) Superinfection of hydatid cyst (Fig. 3)
Previous reports have shown a rate of superinfection in cystic hydatidosis of 1–8%.
The superinfection probably occurs from sites next to the hydatid cyst (e.g.,
biliary tree) or as a complication of bacteriemia of any cause.
Thus,
a small rupture on the cyst's wall could induce infection.
The presence of a thickening of the wall,
significant peripheral enhancement,
air bubbles or fluid levels within the cyst can support the diagnosis of infection,
although these findings are not specific.
In selected cases fine needle aspiration can confirm the diagnosis.
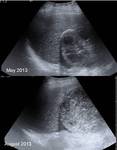
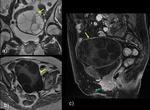
1b) Contained rupture of the cyst ( Fig. 4 ,
Fig. 5 ,
Fig. 6 ).
It occurs when only the endocyst is torn and cyst contents are confined within the surrounding layer of host reactive tissue,
the pencyst.
Endocyst detachment is seen at cross-sectional imaging as floating membranes within the cyst.
Contained rupture may be related to degeneration,
trauma,
infection or response to therapy.
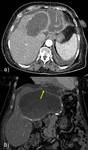
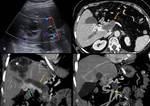
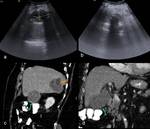
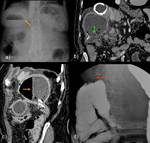
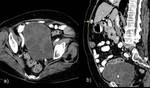
1c) Communication between cyst and biliary tree ( Fig. 7 ,
Fig. 8 ,
Fig. 9 )
Communication of hydatid disease with the biliary tree can be explained by the fact that during cyst growth,
small biliary radicles are incorporated into the pericyst.
Frank rupture into the biliary tree occurs in only 5%-15%of cases.
Jaundice,
fever,
and chills are the most frequent symptoms related to biliary obstruction and cholangitis.
In imaging studies these alterations are usually manifested as hepatic cysts with irregular wall and presence of slightly echogenic or dense material,
associated with bile duct dilatation.
The presence of material with increased viscosity inside the bile ducts may lead to complications such as biliary obstructive syndrome,
acute suppurative cholangitis and even secondary acute pancreatitis ( Fig. 8 ).
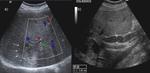
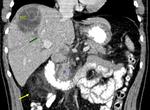
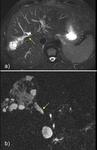
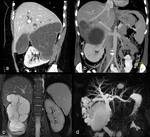
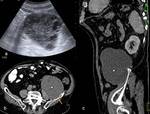
1d) Direct vascular invasion of the portal vein ( Fig. 10 and Fig. 11 )
Direct portal invasion by hydatid cyst contents is an extremely rare complication.
The mechanism usually involves compression of the portal vein and thrombosis with secondary cavernomatosis caused by cysts located in the caudate lobe and hepatic bifurcation The latter phenomenon could be explained by an inflammatory response of the vessel wall caused by external compression of the cyst,
facilitating the creation of a fistula,
allowing passage of vesicles through the vascular wall to the portal lumen.
2- EXTRAHEPATIC COMPLICATIONS (EXTRAHEPATIC EXTENSION OF THE DISEASE)
Direct rupture occurs when both pericyst and endocyst are torn,
allowing free spillage of hydatid material into the surrounding adjacent organs,
or free body cavities.
Hydatid cyst rupture occurs due to degeneration of parasitic membranes caused by aging,
chemical reactions,
or a host defense mechanism.
Hydatid lesions can appear at any abdominal visceral location. When cystic lesions appear in these locations with the typicall characteristics described (multivesicular,
internal membranes,
calcifications,...) hydatid disease should be suspected.
2a) Direct communication to adjacent visceral structures
2a1) Extension to gallbladder ( Fig. 12 )
Because of the small number of cases reported,
opinions about the pathogenesis of the primary gallbladder hydatid cysts are divided depending on the location of the cyst: in the lumen of the gallbladder or on the external surface.
Cysts inside the gallbladder are described as a result of brood capsules dissemination through the biliary tract.
When it grows extramucosally is more likely to have occurred by lymphatic circulation as a result of transport of oncospheres from the intestine to the gallbladder However,
that should be confirmed in a larger number of patients.
2a2) Extension to stomach ( Fig. 13 )
That is a very uncommom complication of hydatid disease.
Ruptured cysts into the stomach derive most commonly from the liver.
Long standing cysts seem to erode adjacent hollow viscera due to compression and resulting ischaemia.
The site of communication may rarely be demonstrated at imaging studies such as computed tomography.
An indirect sign may also be the presence of air-fluid levels,
with or without hydatid membranes within the cyst.
2a3) Extension to colon ( Fig. 14 )
Perforation of an hydatid cyst into the right colon may be either secondary to infection of the cyst or to primary pathology of the perforated organ.
The content of the cyst can drain into the large bowel through the fistula,
and also can allow gas from the large bowel to penetrate into the cyst.
Spontaneous rupture of the cyst into hollow viscera is an extremely rare complication with an estimated frequency of 0.5%.
This complication may be accompanied by clinical findings of hydatidorrhea.
Typically,
the communication is not discovered until surgery,
although in some cases it is found at radiology.
CT may demonstrate a cyst with an air-fluid level or orally administered contrast material inside the cavity.
2a4) Extension to kidney ( Fig. 15 )
Involvement of the kidney is rare (3% of cases).
Renal HCs are usually located in the upper or lower pole.
HCs are frequently solitary and located in the cortex,
and they may reach 10 cm in diameter before any clinical symptoms are noted.
Complications of renal HCs include infection and rupture,
in either the renal sinus or the perinephritic tissues.
A unilocular HC can mimic necrotic renal cell carcinoma,
and the presence of calcification does not help distinguish HC from renal cell carcinoma due to the concomitant presence of calcification in the latter.
Multilocular HCs can be misdiagnosed as simple renal cysts,
cystic nephroma,
and cystic variants of renal cell carcinoma.
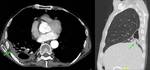
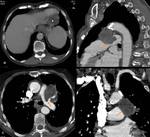
2a5) Extension to lung (transdiaphragmatc migration) ( Fig. 16 )
Involvement of the diaphragm and thoracic cavity occurs in 0.6%–15% of cases of hepatic hydatid disease.
Transdiaphragmatic migration of hydatid disease from the posterior segments of the right hepatic lobe has been reported to be a common complication and is probably related to their proximity to the diaphragm, specially the bare area of the liver.
This may be due to the lack of peritoneal covering in this particular area,
resulting in decreased resistance to cyst growth. Transdiaphragmatic migration varies from simple adherence to the diaphragm to rupture into the pleural cavity,
seeding in the pulmonary parenchyma,
and chronic bronchial fistula
2b) Peritoneal seeding:
Omental ( Fig. 17 ),
Douglas pouch ( Fig. 18 ,
Fig. 18 Fig. 19 ).
Peritoneal hydatid dissemination has a prevalence of about 13% of cases and is almost always secondary to hepatic hydatid disease. Multiple cystic lesions can be observed anywhere in the peritoneal cavity.
Peritoneal echinococcosis usually goes undetected until cysts are large enough to produce symptoms.
The differential diagnosis can be made easily owing to the characteristic appearance of daughter cysts but sometimes it can be difficult to differentiate from mesenteric cysts or intestinal duplication cysts.
2c) Retroperitoneal spread ( Fig. 20 ).
Hidatid cysts at this location are extremely rare with an estimated frequency of 0.8%.
One of the postulated hypothesis is hematogenous spread,
where the embryos once in circulation would not pass the liver and/or lungs and would be implemented elsewhere.
Another possible route could be lymphatic spread from the intestine into the thoracic channels and then to other body sites.
It has also been suggested that the embryo could be maintained in the rectal ampulla and migrates through the hemorrhoidal vessels eventually reaching a pre-rectal or retro-bladder location.
2d) Hematogenous dissemination
2d1) Spleen hydatidosis ( Fig. 21 )
Splenic hydatid disease has been reported to constitute up to 4% of cases of abdominal hydatid disease. The imaging characteristics of splenic hydatid cysts are similar to those of hydatid cysts: calcification of the cyst wall,
the presence of daughter cysts and membrane detachment.
The differential diagnosis includes other splenic cystic lesions such as epidermoid cysts,
pseudocysts,
splenic abscesses,
hematomas and cystic neoplasms of the spleen. Owing to the risk of spontaneous or traumatic rupture,
splenic hydatid cysts are usually treated surgically.
2d2) Extension to pancreas ( Fig. 22 )
Primary HC of the pancreas is very rare,
with a reported prevalence of 0.25% The cyst may easily be confused with a pseudocyst of the pancreas.
However,
the presence of a thickened and more laminated wall than a simple cyst and a thin layer of calcification within the lesion associated with liver HC may suggest a hydatid cyst.
The differential diagnosis includes pseudocyst,
serous cystadenoma,
and mucinous cystic neoplasm.
2d3) Pulmonary artery involvment ( Fig. 23 ).
Hydatid disease is a rare cause of pulmonary embolism.
This uncommon complication is sometimes seen when there is embolisation of infectious particles (intravascular thrombus containing microorganisms) through the pulmonary arterial system or when direct invasion of vena cava occurs.
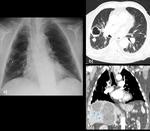
2d2) Lung hydatid disease ( Fig. 24 ).
The lung is the second most common site of involvement of E.granulosus in adults (10-30% of cases). The coexistence of liver and lung disease is present in only 6% of patients.
Most cysts are acquired in childhood,
remain asymptomatic for a long period of time,
and are later diagnosed incidentally at chest radiography.
Uncomplicated cysts appear as well-defined masses that may vary from 1 to 20 cm. Cysts are multiple in 30% of cases,
bilateral in 20%,
and located in the lower lobes in 60%.
Cyst growth produces erosions in the bronchioles that are included in the pericyst,
and as a result,
air is introduced between the pericyst and the laminated membrane.
This air collection appears as a thin,
radiolucent crescent in the upper part of the cyst and is known as the crescent sign or meniscus sign.
If the content is only partially evacuated,
a waterline image appears,
commonly referred to as the "water-lily or camalote sign".
Sudden coughing attacks,
hemoptysis,
and chest pain are the most common clinical symptoms.
After cyst rupture,
expectoration of cyst fluid,
membranes,
and scolices may occur.
Rupture into the pleural cavity may also occur.
Although allergic episodes may develop,
fatal anaphylaxis is uncommon.
Bacterial infection of the cyst is the most serious complication after rupture.
2d4) Bone involvement ( Fig. 25 ).
The frequency of osseous involvement in hydatid disease is 0.5%–4%
In bone involvement,
pericyst formation does not occur,
thereby allowing aggressive proliferation along trabecular bone.
The parasite replaces the osseous tissue between trabeculae due to slow growth of multiple vesicles.
With time,
the parasite destroys the cortex,
with subsequent spread of the disease thtough surrounding tissues.
Extraosseous cysts may calcify,
whereas intraosseous disease rarely demonstrates calcification.
The most common form of bone involvement is spinal hydatid disease,
accounting for more than 50% of cases.
It is usually difficult to distinguish from tuberculous spondylitis or chronic osteomyelitis.
Although CT allows precise assessment of osseous lesions and clearly depicts hydatid cyst calcification,
MR is superior in demonstrating neural involvement.
TREATMENT
The definitive treatment of complicated hydatid disease is surgery with removal of the cyst and instillation of escolicides solutions such as hypertonic saline or ethanol,
but in recent years due to the development of techniques for liver resection,
pericysto-resection or even hepatectomy have been performed,
and thereby obtained a low rate of morbidity and shortening of the postoperative period.
Also adjuvant treatment is recommended with albendazole,
starting at least 4 days prior to removal and staying for more than 4 weeks.
Sometimes as recurrences after surgery,
in inoperable patients or those who refuse to surgery, a percutaneous aspiration can de done,
with infusion of escolicide agents and re-aspiration (PAIR technique) by ultrasound control.
Recent studies have shown that this technique achieves cure rates equivalent to those achieved with surgery recurrence,
but with lower perioperative morbidity and a shorter hospital stay.
However more studies to specify the indications for this technique are needed.