1.
Coronary calcium imaging
Diagnostic Role in symptomatic patients
- CT Calcium mostly used for risk stratification
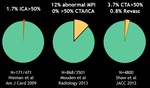
- A negative Calcium score makes obstructive CAD very unlikely and is associated with an excellent prognosis
- CT Calcium detection is a reliable means to exclude obstructive CAD in stable symptomatic patients (Figure 1)
Protocol
Simple,
ECG-triggered CT scan without contrast medium to assess the presence and quantity of calcified coronary plaque.
In patients with a low-intermediate probability of CAD,
the absence of calcium excludes obstructive CAD.
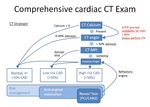
Patients with a positive calcium score (>0) will continue with a CT angiogram (Figure 2).
2.
Coronary CT angiography
Diagnostic performance
- High technical feasibility with current scanners
- CTA accurately rules out CAD (high sensitivity and negative predictive value),
and is regarded an acceptable diagnostic test if probability of CAD is low-intermediate (15-50%)
- CTA can avoid invasive cath after equivocal stress test
- CTA can replace invasive cath to rule out ischemic heart failure
- CTA can exclude prognostically relevant CAD
- CTA overestimates angiographic (and functional) severity of CAD,
particularly in the presence of calcification or other artifacts
Protocol
ECG-triggered,
contrast-enhanced CT scan to image the coronary artery lumen and detect obstructive coronary disease.
If >50% obstructive coronary disease is absent,
the evaluation ends at this point (Figure 2).
3.
Adenosine-stress myocardial perfusion CT imaging
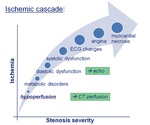
Diagnostic performance
High diagnostic accuracy (sensitivity 83-97,
specificity 78-100) to identify hemodynamically significant CAD,
compensating the modest specificity of CTA
Performing
After identifying a significant stenosis on CTA,
an adenosine-stress myocardial perfusion scan is performed.
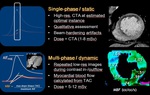
Two types of stress perfusion are possible: single-phase (static) or multi-phase (dynamic) (Figure 4).
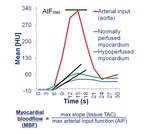
After 3 minutes of coronary vasodilation by adenosine infusion 140 ug/kg/min CT images of the myocardium will be acquired during injection of iodine contrast medium.
Patient selection:
- BMI preferably <30 kg/m2
- No arrhythmia
- Hemodynamically and clinically stable conditions
- No contra-indications to adenosine
- For dynamic stress scan: the ability to perform 30 second breath hold
Evaluating and protocol
Myocardial bloodflow is calculated from the maximum slope (tissue TAC) devided by the maximal arterial input function (AIF) (figure 5).
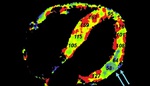
Reduced opacification of myocardium indicates a perfusion defect (<75ml/100ml/min) and indicates myocardial ischemia (Figure 6).
Patients without significant myocardial ischemia will be treated medically.
Patients with substantial myocardial ischemia will be referred for invasive coronary angiography,
in accordance with international guidelines,
and possible revascularization.
4.
Recommendations and considerations of a tiered comprehensive cardiac CT protocol
The cardiac CT exam improves care for patients with possible heart problems:
- More accurate,
faster diagnosis of CAD
- Reliably excluding CAD
- Less unnecessary invasive cath
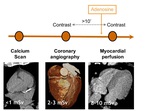
Expansion with CT myocardial perfusion leads to (Figure 7):
- Possibly full diagnostics on one day
- Radiation 10 – 14 mSv
- More efficient and more accurate diagnostics ultimately results in more affordable care
5.
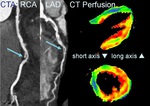
Case example (Figure 8)
53 year old woman with atypical chest pain > Intermediate pre-test probability for obstructive coronary artery disease:
Cardiac CT Exam:
- Ca-imaging: CAC Agatston score: 141
- CTA: a 50-70% stenosis in the mid RCA and mid LAD
- CT perfusion (70kV): shows myocardial ischemia of the anterior and septal wall,
indicating an hemodynamically important LAD lesion.
Total radiation dose:
- Calcium scan: 0,6
- CTA: 2,1
- CT perfusion: 7,2 +
9,9 mSv