The most important consideration in any antenatal imaging is to identify presence of or increased risk of fetal anomaly,
additional timely intervention,
decision about continuation/ safe termination of gestation,
planning for safe delivery for the mother and child and post natal care thereafter.
Since several crucial decisions are based on a positive screen,
it is imperative to produce accurate and consistent diagnosis of fetal anomalies.
Key diagnostic features that are close differential diagnosis are provided in a tabular form as an easy comparison tool.
|
Key Diagnostic & Clinical features are explained under the following headings: Please see Table 7,
8,
9 for more information
Ultrasonographic features of each Anterior Abdominal Wall Defect:
- Location of defect
- Presence or absence of covering membrane/ sac
- Umbilical cord and its insertion
- Size and contents of externalized viscera
- Complications
- Associated findings
- Associated structural anomalies
- Fetal mobility
- Top differential diagnosis
Pertinent clinical issues also included:
- Further investigations
- Chromosomal aberrations
- Prognosis
- Management
- Implication for future pregnancies
|
Physiological Gut Herniation,
Omphalocele,
Gastroschisis in antenatal ultrasound are listed in Tables 7(A) and 7(B) to simplify the distinguishing features of closely related entities.
Each diagnosis is then later explained individually.

Table 7: Table 7(A): Imaging features of Physiological herniation, Omphalocele and Gastroschisis
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"

Table 8: Table 7(B): Clinical Implications of Physiological herniation, Omphalocele and Gastroschisis.
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"
Definition:
Midline abdominal wall defect with herniation of abdominal contents into base of umbilical cord.
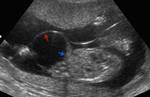
Best diagnostic clue:
Color Doppler shows umbilical cord insertion at the apex of midline anterior wall mass.
| Key Learning Points:
Careful search for other structural anomalies (common)-
- Dedicated fetal echocardiography (Cardiac anomalies are most common associated finding)
Distinction from Gastroschisis is essential in view of associated abnormalities and outcome-
- High resolution ultrasound to evaluate membrane and contents of omphalocele
- Ascites in omphalocele may cause confusion with gastroschisis
- In utero rupture of membranes makes it difficult to distinguish from gastroschisis.
- A chromosome abnormality is more likely if an omphalocele contains only small bowel
|
Mimicks:
- “Pseudo-omphalocele” - can be caused by oblique plane of scan and excessive transducer pressure.
- Cavernous hemangiomas,
blood clots after placental abruption and acardiac monster can also mimic appearance of an omphalocele or gastroschisis [1].
Associated structural abnormalities are common: [8,
9,10,11]
- Cardiac defects: 50% of associated anomalies
Ventricular and atrial septal defects most common
Tetralogy of Fallot
- Gastrointestinal: 40% of associated anomalies
Malrotation always present
Congenital diaphragmatic hernia
Atresias
- Musculoskeletal
- Genitourinary
- Central nervous system
- Umbilical cord cyst

Fig. 1: Figure 1. Syndromes associated with Omphalocele.
*most common.
Definition:
Bowel herniation through a right paramedian abdominal wall defect (rarely reported on the left).
[13]
Best diagnostic clue:
- Free floating extra-abdominal bowel loops
- Does not contain liver
- Colour Doppler shows umbilical cord insertion in normal location
|
Key learning points:
- Bowel related abnormalities are the most common and important complications of gastroschisis.
[14]
- When extra-GI defects are identified,
an alternate diagnosis should be considered.
[15]
- Serial ultrasound for detection of bowel complications and assessment of growth.
- Oligohydramnios suggests fetal distress.
Close follow-up is recommended.
- Polyhydramnios correlates with severe neonatal bowel complications.
- Abnormal waveforms in the umbilical artery associated with obscured bowel and fetal demise.
- Early delivery considered should bowel dilatation worsens (controversial).
|
Bowel complications: [14,
16,
17]
- Bowel ischemia and obstruction
Torsion around narrow vascular pedicle
Compression of mesenteric vessels in small paraumbilical defect
Both intra and extra abdominal loops may be dilated
Large variations exist in literature as to what diameter is "significant" (10-18 mm) [18,19]
Greater dilatation,
poorer prognosis.
[19]
Impact on long term morbidity.
- Perforation
- Bowel wall may become thickened,
echogenic,
matted and nodular.
Secondary to chemical peritonitis from exposure to amniotic fluid
Associated with poor function
- May resorb on follow-up exam ("vanishing gut")
Associated with tight defects
Ischemia causes atresia
Short bowel syndrome
- Oligohydramnios more common than polyhydramnios.
Polyhydramnios is suggestive of associated atresia.
Associated structural anomalies:
- Gastrointestinal:
Mal-rotation or non-rotation of bowel.
Bowel atresia (7-30%) often long segments.
- Low association with non-GI abnormalities (<5%):
Cardiac (most common),
Hypoplastic gall bladder,
Meckel diverticulum,
Hydronephrosis.
____________________________________________________________
In continuation to Table 7,
Tables 8(A) and 8(B) compare closely related diagnosis of Pentalogy of Cantrell,
Limb body wall complex and Amniotic band syndrome.
Each diagnosis is then later explained individually.

Table 9: Table 8(A): Imaging features of Pentalogy of Cantrell, Limb body wall complex and Amniotic band syndrome.
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"

Table 10: Table 8(B): Clinical implications of Pentalogy of Cantrell, Limb body wall complex and Amniotic band syndrome.
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"
| 3.3 PENTALOGY OF CANTRELL (POC): |
Definition:
Pentalogy of Cantrell is a complex malformation with five components:
- Midline anterior abdominal wall defect,
- Anterior diaphragmatic defect with hernia,
- Distal sternal cleft,
- Defect of the apical pericardium with communication into the peritoneum,
- Intra-cardiac defect
Incomplete variant forms can exhibit three or four of these features.
[20,21,22]
Best diagnostic clue: Co-existing ectopia cordis and omphalocele.
Associated structural abnormalities:
- Cardiac anomalieS
Atrial septal defects (50%)
Ventricular septal defects (20%)
Tetralogy of Fallot (10%)
- Cranio-facial and vertebral anomalies
Cleft lip/palate
Exencephaly,
encephalocele
- Chromosomal abnormalities
Trisomies 13,
18
Turner syndrome (45,XO)
- Cystic hygroma
| 3.4 LIMB BODY WALL COMPLEX (LBWC) |
Definition:
Complex array of multiple lethal malformations characterized by an immobile fetus,
attachment of visceral organs to placenta,
with a short or absent umbilical cord.
[23,24]
Two phenotypes described:
- Associated cranio-facial defects (60%)
- No craniofacial defects (40%)
Best diagnostic clue: Grossly distorted fetus with major abdominal wall defect,
severe kypho-scoliosis,
short/ absent umbilical cord and limb abnormalities.
[25]
Associated structural anomalies:
- Scoliosis
Prominent feature- often severe with multiple acute angulations.
- Limb defects
Clubfoot
Absent limbs or digits
Arthrogryposis
Polydactyly
Syndactyly
Abnormal limb positioning
- Cranio-facial defects (60% of LBWD)
Encephalocele or exencephaly
Facial clefts
Neck often extended
- Cardiac
Ectopia cordis
Structural defect
- Renal
Hydronephrosis
Agenesis
Cystic dysplasia
- Gastrointestinal - Bowel atresia
- Congenital diaphragmatic hernia
| 3.5 AMNIOTIC BAND SYNDROME |
Definition:
Formation of fibrous amniotic bands and entrapment of fetal parts by disrupted amnion Resulting anomalies (usually multiple) are:
- Clefts
- Constrictions
- Amputations
- Malformation
- Deformation
Best diagnostic clue:
Variable and asymmetric pattern of defects with amniotic bands seen in contact with the deformity.
Isolated or multiple defects- Cranio-facial deformities are common.
[26,
27]
|
Key learning points:
- POC: Co-existing ectopia with omphalocele.
- LBWC: Distorted fetus.
Malformations are incompatible with life.
- Amniotic band syndrome: Defects have unusual distribution and do not conforming to pattern of developmental defects.
Amniotic bands may be difficult to discern,
especially in setting of oligohydramnios.
|
____________________________________________________________
In continuation to Table 7 and Table 8,
Tables 9(A) and 9(B) compare closely related diagnosis of Bladder Exstrophy,
Bloacal Exstrophy and OEIS syndrome.
Each diagnosis is then later explained individually.

Table 11: Table 9(A): Imaging features of Bladder exstrophy, Cloacal exstrophy and OEIS syndrome.
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"

Table 12: Table 9(B): Clinical Implications of Bladder exstrophy, Cloacal exstrophy and OEIS syndrome.
References: "Diagnostic and Interventional Radiology, Manipal University, Manipal Hospital - Bangalore/IN 2015"
Definition:
Failure of closure of lower abdominal wall resulting in exposed bladder.
Variable severity- ranges from a small vesico-cutaneous fistula and simple epispadias to complete exstrophy with wide diastasis of symphysis pubis and genital defects.
Best diagnostic clue:
Absence of bladder with infra-umbilical solid or complex soft tissue mass seen immediately superior to the fetal genitalia (Best seen in sagittal view).
Color Doppler is useful for identifying umbilical arteries on either side of lower abdominal wall mass.
[28]
Key learning points:
- Prolonged and repeated scans fail to reveal the fetal urinary bladder in presence of normal renal collecting system and ureter and amniotic fluid.
- The externalized soft tissue mass does not contain any large cystic area.
- Important to distinguish from cloacal exstrophy,
which has a worse prognosis
|
Associated structural anomalies:
- Genitourinary anomalies
Epispadias and short penis in males
Mal-descended testes
Cleft clitoris and duplicated vagina in females
- Inguinal hernias
- Spinal dysraphism and scoliosis [29,
30]
Definition:
Spectrum of abnormalities resulting from abnormal development of lower abdominal wall with involvement of urinary and gastrointestinal tracts.
Best diagnostic clue:
Absent bladder with ‘Elephant’s trunk appearance’ (Prolapsed ileum resembles an elephant's trunk and Omphalocele forms upper part of defect.)
Color Doppler: Useful to localize umbilical arteries and cord insertion [31,
32]
Key learning point:
Associated anomalies are common- resulting in poorer prognosis.
|
Associated structural anomalies:
Very common.
- Vertebral (40-90%)
- Myelomeningocele (30-70%)
- Urinary tract (up to 60%) - Leading to oligohydramnios
- Club feet (20-45%)
- Gastrointestinal (50%)
- Polyhydramnios
Definition:
Full complex consists of 4 components:
- Omphalocele
- Exstrophy of bladder
- Imperforate anus
- Spinal deformities
Best diagnostic clue:
Idenitification of 3 out of 4 components on ultrasonography- imperforate anus often not detected in utero.
Key learning point:
Critical to distinguish OEIS from isolated classical bladder exstrophy and isolated neural tube defect.
|
Associated structural anomalies:
- Spinal
Spine bifida
Hemivertebra and segmentation defects
Myelomeningocele
- Pubic diastasis
- Ambiguous genitalia and mullerian defects
- Fistulas
Recto-vesicle
Recto-vaginal
Complex involving rectum,
vagina and bladder
- Renal anomalies
Horseshoe kidney
Renal agenesis
- Limb hypoplasia and aplasia [33]
| 3.9 PRUNE BELLY SYNDROME: |
Definition:
A triad of distinctive features including deficient anterior abdominal wall muscles,
undescended testes,
and urinary tract abnormalities- probably due to severe urethral obstruction in fetal life.
[34]
Best diagnostic clue:
Large abdominal girth with cystic masses that could represent massive dilatation of ureters and upper tracts,
very large bladder and megalourethra.
Key learning points:
- Consider the diagnosis when there is massive dilatation of the entire collecting system with large abdominal girth.
- Deficient abdominal musculature-
Absence of full thickness defect
Absence of externalized viscera
|
Complications:
Early obstructive uropathy with renal failure,
pulmonary hypoplasia,
death in neonatal period.
Associated structural anomalies:
Dysplastic kidneys,
cardiovascular and gastrointestinal malformations,
musculoskeletal defects including limb abnormalities.
Differential diagnosis:
Posterior urethral valves,
megacystis-microcolon.
Management:
Termination of pregnancy can be offered before the age of viability.
____________________________________________________________