This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
CT-Angiography, Arteries / Aorta, Arterial access, Aneurysms
Authors:
V. Markotić1, G. Bogdan1, D. Radančević1, J. Maskovic2; 1Mostar/BA, 2Split/HR
DOI:
10.1594/ecr2016/C-0120
Background
A mycotic aneurysm arising from bacterial infection of the arterial wall.
It can be a common complication of the hematogenous spread of bacterial infection.
William Osler first used the term "mycotic aneurysm" in 1885 to describe a mushroom-shaped aneurysm in a patient with subacute bacterial endocarditis. This may create confusion,
since "mycotic" is typically used to define fungal infections.
The majority of such aneurysms are caused by bacteria and that is reason why Fredric Jarrett proposed term “infected aneurysm’’.
Incidence of mAA is 1% to 2% of all aortic aneurysms.
It occurs mainly in elderly men.
Saccular aneurysms are seen most commonly.
Operative mortality remains high.
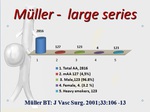
Müller - large series included 2816 patients with aortic aneurysm,
127 (4,5 %) patients diagnosed with mycotic aortic aneurysm.
There were 123 (96,8%) male,
only 4 (3,2%) female and 123 were severe smokers.
The most common cause of an infected aneurysm is direct deposition of circulating bacteria in diseased atherosclerotic,
or traumatized aortic intima after which organisms penetrate the aortic wall through breaches in intimal integrity to cause microbial arteritis.
A septic embolus from bacterial endocarditis had been once the most common etiology but has become rare in the era of efficacious antibiotic treatment of septicemia.
Consistently the most frequently identified organisms are Staphylococcus aureus and Salmonella species.
Aortic infections with unusual organisms include tuberculous mycotic aneurysm,
mycotic aneurysm due to Aspergillus terreus and luetic mycotic pseudoaneurysm.
Today,
mycotic aortic pseudoaneurysm in immunocompromised population is increasingly encountered,
such as HIV - related aortic aneurysms.
Clinical manifestation
Fever occurs in about 70% of the patients.
Back pain or abdominal pain each occur in about third of the cases (30% - 50%).
Leukocytosis and an elevated erythrocyte sedimentation rate in 73% of the cases.
Weight loss is common.
The aneurysm is palpable in 50% to 60% of cases and almost always tender.
The onset is insidious,
and a low-grade fever may be present for several months before diagnosis.
A tender and pulsatile abdominal mass in febrile patient should be considered as an infected aneurysm until proven otherwise.
The natural of infected aortic aneurysms history is expansion and eventual rupture,
with extremely rapid progression.
Rupture may occur in to: retroperitoneal space or peritoneal cavity (56%),
pleural cavity (9%),
duodenum (12%),esophagus (6%) and pericardium (3%).
Salmonella and gram-negative infections have a greater tendency to early rupture and cause death.
Overall mortality from rmAA is over 50% despite advances in therapy.
Blood cultures are helpful in suggesting the diagnosis and identifying the pathogen ,
although there are up to 25% negative cultures.
Diagnosis
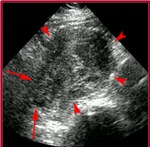
Abdominal ultrasonography is initial method.
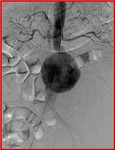
Aortography is generally performed preoperatively to assist in surgical planning or EVAR/TEVAR.
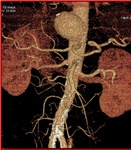
MDCT scanning is superior in demonstrating associated pathological findings suggestive of an infectious etiology.