Diagnosis of RPS edema:
Knowledge of the normal RPS anatomy as detailed in the background section should facilitate the diagnosis of abnormal RPS edema.
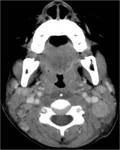
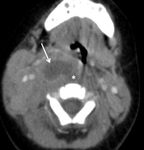
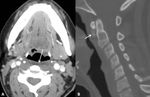
When analyzing cervical spine and neck images radiologist should look for the normal RPS fat (FIG 1),
whenever edema is present instead of fat,
its source should be searched.
Edema should be distinguished from abscess that usually has peripheral enhancement and exert mass effect.
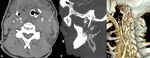
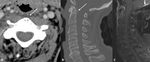
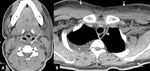
Intrapharyngeal / intra-esophageal fluids that have rounded configuration,
should not be confused with RPS edema (FIG 3).
The presence of a median raphe within the fluids and flattened configuration confirm the diagnosis of RPS edema.
Infection
Infectious disease that cause RPS edema may be secondary to spinal or oropharyngeal infection.
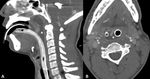
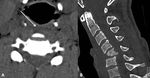
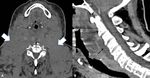
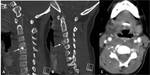
Cervical discitis osteomyelitis (FIG 4) will usually manifest with cervical spine pain and motion restriction.
Signs of myelopathy depend on the degree of spinal cord compression.
MRI is the modality of choice for the diagnosis and delineation of discitis osteomyelitis.
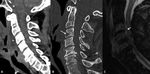
Disc edema and enhancement,
adjacent end-pate erosions and vertebral bodies edema are easily seen on MRI.
The diseased segment might not be in opposite to the edema (FIG 5).
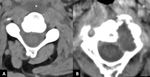
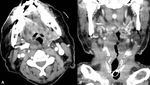
Oropharyngeal infections that cause RPS edema encompass cervical adenitis (FIG 6),
retropharyngeal and tonsilar abscesses (FIG 7) and necrotizing fascitis.
Oral infection might also be accompanied by RPS edema.
Trauma
In blunt trauma scenario RPS edema could result from cervical spine injury or from soft tissue contusion with or without vascular injury (FIG 8,
9).
The edema will be most discernible on soft tissue window images.
Careful inspection of the bony and soft tissue elements is crucial whenever RPS edema is seen in a trauma victim.
In appropriate cases CTA should be performed to exclude vascular injury.
In the presence of RPS edema,
if the CT is unremarkable consider MRI for further evaluation to exclude ligamentous injury.
Neoplasm
Primary neoplasms of the RPS are rare.
Lipoma is the most common mass lesion of the RPS.
Lymph nodes in the suprahyoid RPS may have neoplastic infiltration either from a primary neoplasm or metastases of head and neck malignancies.
RPS edema could accompany head and neck malignancies when there is significant lymph node disease that interfears with fluid resorption (FIG 10).
Inflammation
A verity of inflammatory conditions can cause RPS edema.
Patients may present with non specific symptoms of neck pain and will undergo CT or MRI as part of their evaluation.
The radiologist might be the first to recognize the disease based on appropriate imaging findings.
Acute calcific longus colli tendinitis is an inflammatory disease caused by deposition of calcium hydroxyapatite crystals in the upper most fibers of the longus colli muscle.
It affects adults usually aged 30-60 years and present with neck pain that might progress to odynophagia.
Imaging findings are pathognomonic with amorphous calcifications anterior to C1-2 and RPS edema (FIG 11).
Acute symptomatic intervertebral disc calcification is a rare self-limited childhood disease that may cause neck pain and torticollis.
Anterior disc displacement may result odynophagia and RPS edema (FIG 12).
Crowned dens syndrome refers to CPPD (Calcium PyroPhospahte crystal Deposition disease) deposition around the dens.
It is a rare manifestation of CPPD,
usually present in elderly with severe neck pain and motion restriction.
On imaging calcifications are seen around the dens on CT and there are signs of dens inflammation on MRI.
RPS edema might be present (FIG 13). The term derives from the crown-like density surrounding the odontoid process.
Post radiation edema
RPS edema may appear 4-6 weeks following radiation therapy of head and neck malignancy.
Edema of additional irradiated organs and flattened configuration of the fluids confirms its benignancy.
Peripheral enhancement along the fluid collection should raise the possibility of infection.
Diffuse fluid overload
RPS edema might be a part of systemic fluid overload a seen in congestive heart failure, renal failure or liver failure.
Visualization of systemic fluids accumulation and appropriate medical history should facilitate the diagnosis.