RESULTS
A total of 11 patients with 7 FNSs and 4 FNVMs were reviewed.
The mean patient age at time of initial imaging evaluation of FNSs and FNVMs was 39 years (range 14–63) and 47 years (range 39–57 years) respectively.
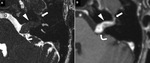
FNS commonly extended over more than one segments of the intratemporal FN (Figure 1) and had propensity to involve the geniculate ganglion (2/7,
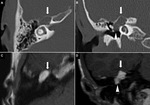
29%) (Figure 2) and mastoid segment (3/7,
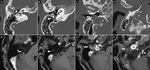
43%) (Figure 3 and 4).
In contrast,
FNVMs most commonly occurred at the geniculate ganglion (3/4,
75%) with no case found at the mastoid segment.
All cases of FNSs demonstrated smooth expansion of the bony canal with larger lesions showing bony thinning or dehiscence.
In contrast,
FNVMs demonstrated amorphous (2/4,
50%) or a "honeycomb" (2/2,
50%) (Figure 5) pattern of bone reaction with sclerotic foci seen in 3/4 (75%) cases.
MRI signal for FNSs are iso/hypointense on T1WI and hyperintense on T2WI.
FNVMs appear isointense on T1WI and hyperintense on T2WI.
In addition,
tiny hypointense foci maybe seen in FNVMs likely attributed to presence of sclerotic matrix (Figure 5).
Both FNSs and FNVMs show avid enhancement on gadolinium enhanced T1WI.
Ten patients were managed surgically (10/11) with histopathology analysis of the specimen.
One patient (1/11) was managed via stereotactic radiosurgery.
Available final histopathology results were concordant with the pe-operative imaging diagnosis in nine patients (9/11),
however both readers were uncertain for the diagnosis in one patient (1/11) (Figure 6) and eventual histopathology analysis confirms the diagnosis of FNVM.
Only one patient (1/11) was managed via stereotactic radiosurgery.
Although no histopathology was available,
the pre-operative imaging finding is typical of a FNS (Figure 1).
HISTOPATHOLOGY
Macroscopically,
FNSs are well encapsulated benign tumors composed of bundles of Schwann cells.
The cellular architecture comprises dense cellular areas (Antonio A) in a background of loose myxomatous stroma (Antonio B).
Intratumoral cystic degereneration were oberved in 2 cases of mastoid segement FNSs.
FNVMs were formerly incorrectly termed hemangiomas,
a term that should be reserved for vascular neoplasms that arise by cellular hyperplasia.
Histologically FNVMs composed of dilated and irregular vascular channels surrounded by a thin layer of smooth muscle but lacking an elastic laminae.
The ossifying subtype of FNVMs contains spicules of lamellated bone.
The endothelial cells are non-mitotic.
FNVMs stain negative for GLUT1 (a hemangioma marker) and podoplanin (lymphatic differentiation) [5].
DISCUSSION
FNSs commonly involved more than one segment of the intratemporal facial nerve with propensity toward the mastoid segment or geniculate ganglion.
Although skip lesions have been described in the literature,
this was not observed in our patient cohort [1].
On temporal bone HRCT,
FNSs demonstrate FN canal thinning,
scalloping in smaller lesions and dehiscence in larger lesions,
compatible with the slow growth of these tumors [2].
The morphologic appearance of FNSs are specific to the segment of the FN involved.
Canalicular FNSs are typically fusiform and can be indistinguishable from the more common vestibular schwannoma.
However,
when canalicular FNSs demonstrate contiguous involvement of the adjacent labyrinthine segment,
the diagnosis of FNS can can be made with confidence (Figure 1).
FNSs can also extend distally into the geniculate ganglion.
Geniculate ganglion FNSs have been reported to be capable of extension anteromedially along the greater superficial petrosal nerve,
however this has not been reported in our cohort [2].
Tympanic segment FNSs can cause dehiscence of the thin bony cortex of the tympanic canal and when large protrude into the middle ear cavity (Figure 2) and uncommonly erosion of the adjacent lateral semicircular canal [2].
Morphology of mastoid segment FNSs depend on the individual variation of mastoid pneumatization.
In individuals with well penumatized mastoid septations,
gradual expansion of mastoid segment FNSs results in trabecular breakdown and may protude through weak point anterolaterally into the external auditory canal or extends beneath the skullbase causing smooth enlargement the stylomastoid foramen [2] (Figure 3 and 4).
FNSs are typically iso to hypointense to gray matter on T1WI and hyperintense on T2WI [2].
Larger lesions tend to demonstrate greater signal heterogeneity and intratumoral cyst degeneration [2] (Figure 4).
Postcontrast enhanced MR images demonstrate homogeneous enhancement.
MRI provides superior resolution to determine segment FN involvement via enhancement pattern and FN thickening in small size lesions prior to prominent bony remodelling.
Geniculate ganglion FNSs when large can cause tegmen tympani dehiscence and MRI provides detailed pre-operative assessment of the intracranial extension.
FNVMs most commonly occur at the geniculate ganglion as seen in our cases series.
On temporal bone HRCT,
FNVMs are seen as a poorly marginated lesion which can extend into the adjacent labyrinthine or tympanic FN segment [4].
Larger lesions display an amorphous “honeycomb” appearance and may contain distinct calcified or mineralised matrix [4] (Figure 5).
This “honeycomb” appearance is diagnostic of geniculate ganglion FNVMs.
However,
when FNVMs are of small size they may be indistinguishable from FNS (Figure 6).
On MRI FNVMs is of mixed signal intensity on T1WI and hyperintense on T2WI.
Foci of low signal intensity maybe observed in both T1WI and T2WI likely attributed to calcified/mineralised internal matrix [4] (Figure 5).
FNVMs show avid enhancement on post contrast T1WI.