This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Neuroradiology brain, MR, Education, Haemorrhage, Hyperplasia / Hypertrophy
Authors:
A. Fraino, A. Casas Martín, H. Saenz Acuña, R. E. Correa Soto, F. Ojeda, J. M. Villanueva Rincón; Salamanca/ES
DOI:
10.1594/ecr2016/C-0618
Findings and procedure details
MRI findings
We used a MRI (General Electric® 1.5 T) with a protocol that includes axial,
coronal and sagittal T2WI,
coronal FLAIR,
and axial T1WI,
PD,
and T1WI with contrast.
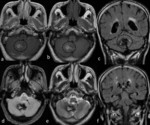
In the initial phase (1-6 months) there is a normal inferior olivary nucleus (ION) on T1WI (no hypertrophy),
but a hyperintense signal on T2WI.
In the later stages (6 months to 3 to 4 years),
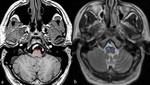
we can find hypertrophy of ION ( Fig. 4 ),
isointense to slightly hypointense to gray matter on T1WI,
and increased signal of ION on T2WI ( Fig. 5 ).
Contralateral cerebellar atrophy can occur,
although this is more commonly seen with involvement of the olivodentate fibers.
Also,
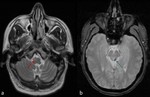
MRI can detect a primary lesion located in ipsilateral central tegmental tract or contralateral dentate nucleus,
for example low signal areas on T2WI gradient echo reveals hemosiderin deposition ( Fig. 6 ).
Hypertrophic olivary degeneration on FLAIR is similar to T2WI,
has high signal intensity on PD,
and does not enhance after intravenous contrast (gadolinium).
Causes of hyperintensity signal on T2WI in the anterior part of Medulla.
Brainstem lesions can be classified as focal or diffuse.
Magnetic resonance imaging is the most suitable imaging modality for evaluating these lesions.
As a rule,
focal lesions are not large and have well-defined margins.
Causes include:
- Demyelination related to multiple sclerosis.
- Tumor (astrocytoma,
metastasis,
lymphoma).
- Lesions that involve corticospinal tract,
as Wallerian degeneration,
adrenoleukodystrophy,
amyotrophic lateral sclerosis.
- Vertebrobasilar perforating artery infarct.
- Infections or inflammatory processes as tuberculosis,
sarcoidosis,
HIV/AIDS,
rhombencephalitis.
Demyelination related to multiple sclerosis is an autoimmune and an inflammatory disease characterized by axonal injury and demyelination with multiple lesions of the CNS (brain,
brainstem and spinal cord),
hyperintense on T2WI,
disseminated over time and space.
Clinically,
it presents most frequently with weakness,
parasthesias,
vertigo,
and visual or urinary disturbances.