LUNG CANCER SCREENING PROGRAMME
Elegibility criteria (Fig2):
The eligibility criteria for screening for lung cancer with low dose computed tomography (LDCT) are as follows:
- Asymptomatic (no signs or symptoms of lung cancer)
- 55-75 years.
- Tobacco smoking history of at least 30 pack-years (one pack-year = smoking one pack per day for one year; 1 pack = 20 cigarettes).
- Current smoker or one who has quit smoking within the last 15 years.
CT scan protocol (Fig3):
For a LDCT chest scan an average of 1,5mSv for standard size patients with appropriate reductions in CTDIvol for smaller patients and appropriate increases in CTDIvol for larger patients,
is accepted.
The screening protocol includes a non intravenous contrast CT with slices measuring less than 1,25mm width.
In our hospital a 128 –detector CT scan Siemens SOMATOM Definition Flash integrating a FLASH thorax protocol was used with 128 x 0.6mm collimation and pitch=3.0.
Thanks to the dual source technology and activation of the CARE DOSE kV mode,
high resolution images are obtained allowing very low kV (around 1 mSv) .
Scans were obtained in a cranio-caudal scan direction and full inspiration.
Data sets were derived from images of the lungs with a thickness of 1 mm.
Imaging evaluation:
Images were read on Siemens Singo Via workstations.
The reading is performed by a reader with more than 5 years of experience.
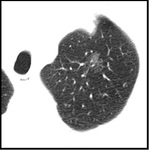
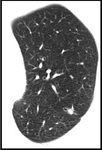
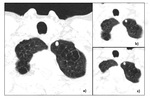
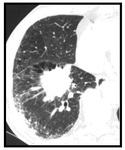
The aim is to identify solitary pulmonary nodule (SPN) that may be solid or subsolid in attenuation (Fig4).
All the nodules are further evaluated.
The diameter of each nodule is calculated based on the maximum axial diameter.
In addition to size,
nodule characteristics such as shape,
attenuation and surface were noted.
Further evaluation of additional findings in the mediastinum,
heart,
soft tissue and bone structures is also reported.
A reporting template sample as utilized in our thoracic department is attached (Fig5).
Management of the nodules was determined based on the highest nodule category found.
LuRADS REPORTING SYSTEM
Establishment of lung cancer screening programs as an additional preventive service benefit is a challenge for radiologists.
Therefore,
a classification system designed as a quality assurance tool to standardize lung cancer screening CT reporting may be very useful.
The Lung Imaging Reporting and Data System (Lung- RADS ™) is the result of the American College of Radiology (ACR) Lung Cancer Screening Committee subgroup.
Making use of a classification system may facilitate communication between professionals and may reduce confusion in CT interpretations.
Therefore it could be of value to provide a framework to the radiological findings,
to facilitate data analysis and may be used as a guide for clinical management.
Version 1.0 of LU-RADS 2014 includes 5 categories (0-4) (Fig6).
The classification is made according to the radiological features of the nodules and their risk of malignancy.
The higher the number in the LU-RADS classification category more risk of malignancy is observed.
Management and outcome monitoring process recommendations are also included within each category.
S and C modifiers may also be added to the 0-4 category.
These depend on whether there are any additional relevant clinical findings other than cancer (S),
or patients with a past history of lung cancer return to the screening programme (C).
A negative screen is defined as categories 1 and 2; a positive screen is defined as categories 3 and 4
· CATEGORY 0 (Fig7 and 8)
· CATEGORY 1 (Fig9,
10 and 11)
· CATEGORY 2 (Fig12,
13 and 14)
· CATEGORY 3 (Fig 15,16 and 17)
· CATEGORY 4A (Fig 18 and 19)
· CATEGORY 4B (Fig 20 and 21)
· CATEGORY 4X (Fig 22)
Important notes for use:
- Negative screen: does not mean that an individual does not have lung cancer.
- Size: nodules should be measured on lung windows and reported as the average diameter rounded to the nearest whole number; for round nodules only a single diameter measurement is necessay.
- Size Thresholds: apply to nodules at first detection, and that grow and reach a higher size category.
- Growth: an increase in size of > 1.5 mm
- Exam Category: each exam should be coded 0-4 based on the nodule(s) with the highest degree of suspicion
- Lung Cancer Diagnosis: Once a patient is diagnosed with lung cancer, further management (including additional imaging such as PET/CT) may be performed for purposes of lung cancer staging; this is no longer screening.
- Nodules with features of an intrapulmonary lymph node should be managed by mean diameter and the 0‐4 numerical category classification.
- Category 3 and 4A nodules that are unchanged on interval CT should be coded as category 2, and individuals returned to screening in 12 month.