I. Procedure details: imaging approach and technique:
Assessment of patients referred to us with groin pain relied on a multitechnique approach.
1. Radiographs:
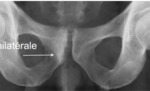
Frontal pelvic radiographs is used in the first line.
Although often normal,
radiographic assessment allows evaluation of symphyseal alignment and screening of the hips,
sacroiliac joints,
and lower lumbar spine for any disorders,
which if detected,
may initiate more advanced imaging of the relevant region.
Focal osseous lesions of the pelvis as well as arthropathy may be detected.
The early signs of origin of common adductor–rectus abdominis’ enthesopathy can be seen.
This appears as ill definition of the cortical bone at the origin of either muscle,
which,
if severe enough,
may form distinct erosion.
Also signs of osteitis pubis can be distinguished ,
characterized by the presence of erosions or osteosclerosis centered at the subchondral bone on either side of the symphysis.
2.
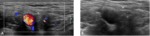
Ultrasonography:
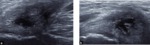
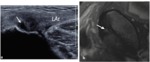
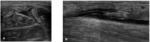
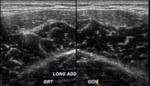
Sonography is a primordial technique in evaluating the groin.
It has the ability to assess the common adductor–rectus abdominis origin in detail.
Careful pressure with the probe further increases the specificity of the examination should the patient complain of pain in this region.
Dynamic sonography with Valsava’s maneuvers may reveal helpful to exclude a hernia or inguinal wall deficiency with great confidence.
Overall,
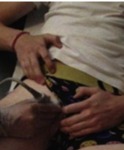
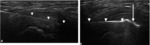
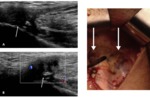
sonography may also be used for performing imaging guided intervention,
such as PRP-injection of the common adductor–rectus abdominis origin for the treatment of tendinosis or partial-thickness tears Fig. 6 Fig. 7
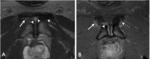
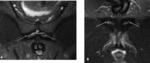
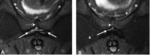
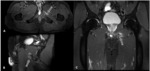
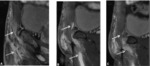
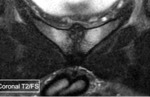
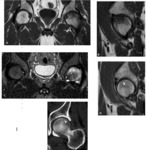
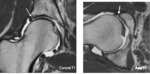
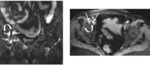
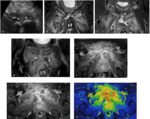
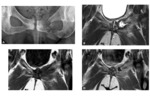
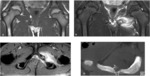
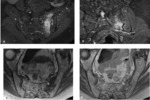
3. MRI:
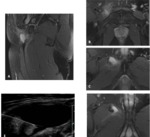
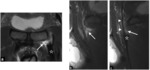
MR imaging may be performed if ultrasound is inconclusive or for presurgical assessment.
It is performed in a comfortable supine position to avoid motion artifacts with an empty bladder and a surface coil.
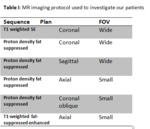
We started with assessment of wide field-of-view (FOV) to visualize the whole pelvis and first exclude various differential diagnoses (tumors, coxo-femoral disorders) .
Smaller FOV sequences and 40°oblique axial slices are then used to assess how the symphysis interacts with adjacent musculotendinous structures .
Injection of gadolinium-based contrast agent is performed to enhance inflammatory tissue or for post-operative assessment .
Table 1
4.
CT:
CT scan rarely IS used to investigate groin pain in our cases. Osteitis pubis is sometimes randomly found when performing a CT scan for other causes.
II.
Findings:
To categorize groin pain etiologies,
we followed recent Doha consensus terminology and which is based on patient history and physical examination,
and that is particularly suitable for clinical practice.
We divided findings into 5 major categories: adductor-related,
iliopsoas-related,
inguinal-related,
pubic-related groin pain and Hip-related groin pain.
A.
Adductor-related groin pain:
1.
Adductor muscle tendon dysfunction:
a)Acute tears and muscle strains:
Acute tears may also involve the proximal musculotendinous junction of the adductor muscles,
most commonly the adductor longus.
If severe enough,
an acute injury may result in full-thickness disruption of the adductor longus and secondary retraction of the tendon distally,
resulting in loss of the moustache appearance of the common adductor origin.
Sonography allows a satisfying assessment of muscle injuries.
MRI is nevertheless considered as the imaging of choice in this field,
and is used to target the location,
and to accurately assess the severity and the extent of the strain.
It is also crucial for monitoring complications and for evaluating treatment response objectively.
Muscle strains (grade 1 or 2) occur most commonly at the anteriorly located musculotendinous junction of the adductor longus; however,
strains may also affect other surrounding muscles in isolation,
such as the pectineus muscle.
If an episode of trauma is severe enough,
multiple muscles may be injured.
Fig. 9 Fig. 10 Fig. 11 Fig. 12 Fig. 13 Fig. 14 Fig. 15 Fig. 16
b)Tendinosis:
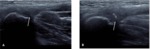
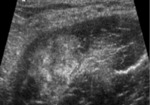
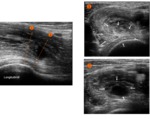
Sonography is able to assess adductor tendinosis.
Areas of decreased echogenicity tendon origin may be noted, which is the hallmark sonographic finding of tendinosis.
Discrete anechoic clefts are consistent with partial-thickness tears.
Erosions of pubic body may also be shown as areas of interruption of the smooth hyperechoic line of the cortex of either the superior or the inferior pubic ramus.
Care should be taken when assessing erosions.
In fact,
they may be revealing:
- Pubic symphysis arthritis,
which is a common finding in athletes with pubalgia.
- Late fusion of secondary ossification centers of pubic rami that may last till the age of 26 year-old.
Tendinosis without any tear is pretty uncommon and may be seen at MR imaging as a diffuse increased signal intensity of the tendon.
Although IV gadolinium was rarely used,
enhancement after its administration at the proximal enthesis and anterior pubic region correlates strongly with the clinically symptomatic side.
Fig. 17 Fig. 18 Fig. 19
The “secondary cleft” is indicative of chronic micro avulsion injury of the tendon fibers and possibly the inferior pubic ligament.
It may be shown MRI and has a high correlation with the side of reported pain
Fig. 20 Fig. 21
c)Other adductor muscles injuries:
Fig. 22 Fig. 23 Fig. 24
2.
Rectus abdominis Strain:
Acute tears may also involve the rectus abdominis and are classically seen in tennis players,
where asymmetric hypertrophy of the rectus abdominis muscle contralateral to the serving arm occurs. Isolated injury to the rectus abdominis origin occurs in 27% of cases ,with combined common adductor–rectus abdominis origin injury occurring in 15–30% of case.
Fig. 25 Fig. 26 Fig. 27
B.
Pubic related groin pain:
Osteitis pubis is,
condition of the pubic symphysis secondary to repetitive microtrauma that induces inflammatory mediated inappropriate osteoclastic activity , ultimately resulting in osseous resorption .
Radiographic changes include irregularity of the subchondral bone plate, erosions, fragmentation, and areas of alternating osteopenia and sclerosis. If severe enough,
the resorptive process may result in joint space widening (> 7 mm).
With time,
the symphysis may undergo accelerated degenerative changes, known as premature symphyseal degeneration.
The CT findings of osteitis pubis mirror the radiographic manifestation but may be detected earlier because of the cross-sectional nature of CT.
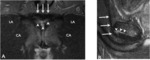
Pubic bone marrow edema, the earliest manifestation of osteitis pubis, is shown on MRI as an area of subchondral marrow hyperintensity on fluid-sensitive sequences.
It can also be considered as an indirect sign of enthesopathy.
Pubic bone marrow edema may be subcortical,
involve entire pubic body or diffuse if superior to 2cm.
- Grade I: < 2cm area at the pubic symphysis
- Grade II: >2cm area at the pubic symphysis
- Grade III: both rami of the pubic symphysis.
If osteitis pubis is allowed to progress with ongoing athletic activity,
subchondral cysts and erosions may occur .
The hypointense subchondral bone plate may become irregular or completely disappear, resulting in symphyseal irregularity,
joint widening,
and an effusion .
Fig. 28 Fig. 29 Fig. 30 Fig. 31
C.
Hip–related groin pain:
A wide variety of hip disorders account for anterior groin pain.
A thorough patient history should be taken,
including incidence of trauma and exercise frequency.
MR imaging as well as CT scan are complementary in the diagnostic process.
Hip-related groin pain causes are mainly represented by coxarthrosis that can also involve young adults.
Avascular femoral head necrosis along with femoro-acetabular impingement have been increasingly recognized as a potential precursor and an important contributor to hip pain.
These etiologies,
if non or misdiagnosed ,
will ineluctably lead to severe osteoarthritis.
Fig. 32 Fig. 33
D.
Inguinal-related groin pain:
Acquired inguinal wall deficiency is an overuse phenomenon occurring in approximately 15% of athletes with groin.
It is best conceptualized simplistically,
involving either the anterior inguinal wall (external oblique muscle and aponeurosis),
the posterior inguinal wall (transversus abdominis and internal oblique muscles),
or both
The advantage of MRI is that it allows direct visual comparison of the contralateral side; however,
findings should be interpreted with caution because of the possibility of bilateral abnormalities.
Treatment is the same as for anterior inguinal wall deficiency.
E.
Ilio-psoas related groin pain:
1.
Post traumatic iliopsoas muscle injuries: Fig. 36
2.
Snapping iliopsoas tendon :
Ultrasound may demonstrate a psoas tendon sunden jerking when investigating patient with lateralized groin pain that may occur when walking or when practicing sports especially those involving large amplitude movements (Dance,
Karate).
This jerking can be sometimes secondary to coxofemoral pathology (osteochondromatosis,
labral cyst).It generally engages psoas tendon and the medial head of iliac muscle.
Jerking movement of the tendon in dynamic sonography is synchronous with the patient's pain and often accompanied by an audible snap.
3.
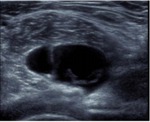
Iliopsoas bursitis :
It generally occurs in patients with moderate coxarthrosis.
Diagnosis can be made by either ultrasonography or MRI.
Fig. 37 Fig. 38
F.
Other conditions causing groin pain:
1.
Infectious causes :
- Septic arthritis:
The predisposing factor are the same as those of spondylitis: a complication of interventions mainly urologic,
contiguous spread of regional septic process ,
septic dissemination following blood transfusion or intravenous drug use,
and during the postpartum period.
- Prostatitis Fig. 39
2.
Stress fracture:
They are believed to reflect abnormal chronic repetitive stress that outstrips the bone’s ability to remodel itself.
The most common pelvic site of stress fractures is the inferior pubic ramus; however,
stress fractures of the femoral neck are more common and also may cause groin pain.
Fig. 40 Fig. 41
Parasymphyseal stress fractures are less commonly encountered but usually are oriented parallel to the articular surface.
They frequently occur with sacral stress fractures.
Parasymphyseal fractures may mimic a neoplasm or infection,
with areas of fragmentation or osteolysis.
3.
Insufficiency fracture:
Fig. 42
4.
Referred pain:
Always remember that groin pain may be referred from other regions,
such as compression of upper lumbar nerves,
sacroiliitis ,
knee pain and thus further imaging may be necessary if no local abnormality is shown.