Arthrography techniques:
We review the anatomical bases and technical principles for arthrography in different articulations of upper and lower limbs.
General technique of arthrography:
Projection of the tip of needle should be surimposed on joint space or ideally on articular recess projection(fig2),
when it buts up against bone,
it is progressively withdrawn with a simoultanous injection test of an anaesthetic agent.
Intra-articular location is presumed when a decrease in resistance is felt.
Then,
a contrast subtance is used to confirm intra-articular location.
An iodinated contrast medium (at a concentration of 240 mgI/ml or less) for CT arthrography is generally used.
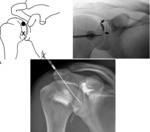
Shoulder: Fig. 1
It can be approched anteriorly or posteriorly.
The most common anterior injection method,
known as Schneider technique, is performed with the patient supine in a straight anteroposterior position with the shoulder slightly externally rotated.
The needle is directed vertically under fluoroscopic control at the junction of the middle and lower thirds of the medial part of the humeral head.
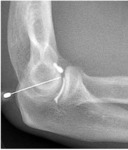
Elbow: Fig. 2
Injection is performed in supine position.Ispsilateral hand is positionned behind the back so that the lateral aspect of the elbow is exposed.
The target is the anterior aspect of the humeroradial compartment.
Alternatively,
the olecranon fossa is targeted in the posterior transtriceps approach.
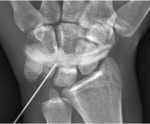
Wrist: Fig. 3,
Fig. 4,
Fig. 5
Single(radiocarpal),
double(radiocarpal and midcarpal or radiocarpal and distal radioulnar),
or triple-compartment(midcarpal,radiocarpal,
and distal radioulnar joint injection techniques can be performed to explore wrist.
A dorsal approach is needed to explore differents join compartments of the wrist .
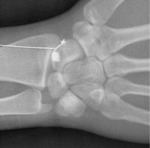
- When we aim to explore the radiocarpal joint ,
the wrist of the patient is positioned prone with mild ulnar deviation to lengthen the scaphoid.
The target is,
in this case,the midportion of the scaphoid.
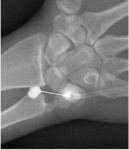
- If the target is radioulnar joint,
the wrist of the patient is positioned prone.
The reference point is the radial and distal aspect of the ulnar head
- When a triple-compartment opacification is required,
the midcarpal joint can be accessed in the space betweenthe lunate,
triquetrum,
capitate and hamate.(fig)
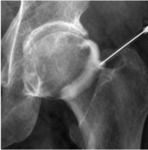
Hip: Fig. 6
The approach for arthrography of the hip necessarily targets the anterior recess(fig).Both medial (fig)and lateral (fig)portions can be targeted.
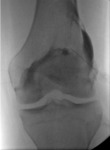
Knee: Fig. 8
The most commonly used technique is the lateral patellofemoral approach.
Arthrography is performed with patient in supine position.
In order to have the articulation in slight flexion,
a small pillow can be placed under the knee.
After lateral subluxationof the patella,the lateral aspect of the suprapatellar recess is punctured.
Any excess of joint effusion should be aspirated before the injection.
Ankle: Fig. 7
Because of the anatomical configuration of the joint,
the approach for arthrography of the ankle can’t be direct and must necessarily target the anterior recess.
Slight plantar flexion is needed.
The entry point is immediately lateral to the tibialis anterior tendon.
The target is just below the joint space.
Cartilage imaging modalities :
The purpose of cartilage imaging is to assess the integrity of the cartilage surface,
the thickness and volume of the cartilage matrix and its relationship with the subchondral bone.
The different imaging techniques have different degrees of accuracy,
sensitivity and specificity.
I. Cartilage:
Articular cartilage is a matrix-reinforced,
gel-like tissue created and maintained by chondrocytes,
its only cellular component.
By weight,
cartilage is predominantly water (80%).
A relatively small population of interspersed chondrocytes produce collagen,
proteoglycans,
and noncollagenous proteins that form the macromolecular matrix that surrounds them.
Much of the water within cartilage is held within this permeable matrix,
and it is the restriction of water movement out of the matrix that allows cartilage to withstand compression. GAG concentration,
is lowest in the superficial zone and highest in the deep zone
II. Indirect Imaging of Cartilage with Radiography and CT
Radiographic evaluation of cartilage is important even though advanced imaging such as MR reveals more detail about cartilage status.
Radiographs of the hip and pelvis are still considered the most appropriate imaging method for the initial evaluation of chronic hip pain by the American College of Radiology.
Because cartilage cannot be radiographically discerned from joint fluid and adjacent tissues of similar density,
macroscopic abnormalities in cartilage cannot be detected directly.
Cartilage pathology must therefore be inferred when secondary signs of advanced disease are present; these include subchondral cysts in areas of full-thickness cartilage loss,
and joint space narrowing once wholesale cartilage thinning has occurred.
Radiographic techniques are limited in their evaluation of cartilage because early disease,
including focal ulcers and fissures,
cannot be detected.
III. Arthro CT scan:
Arthro CT scan allows a much more accurate investigation of the cartilage thickness and to depict chondral anomalies.
Different lesions may be highlighted:
- faint irregularities of the cartilage with abnormal adhesion of the contrast medium
- more or less deep fissures : multiple,
apart or close to the subchondral bone
- larger ulcerations with a thinning of the cartilage,
and sometimes a pediculated flap.
In all cases,
the arthro-CT very satisfactorily assesses the thickness of the cartilage and the subchondral bone.
IV. MRI:
MR imaging can evaluate cartilage directly,
and it can identify macroscopic surface abnormalities including ulcers and fissures visible arthroscopically.
It can also reveal some of the microscopic zonal organization of cartilage that is partially responsible for its unique functional characteristics.
Magnetic resonance (MR) imaging is the most important imaging modality for the evaluation of traumatic or degenerative cartilaginous lesions.
The specific MR imaging techniques used for these purposes can be divided into two broad categories according to their usefulness for morphologic or compositional evaluation.
A. Standard MR evaluation:
To assess the structure of knee cartilage,
standard spin-echo (SE) and gradient-recalled echo (GRE) sequences,
fast SE sequences,
and three-dimensional SE (3D FSE) and GRE (3D SPGR) sequences are available.
These techniques allow the detection of morphologic defects in the articular cartilage and are commonly used in research for semiquantitative and quantitative assessments of cartilage.
T2 and proton-density (PD) weighted FSE sequences provide good contrast between cartilage and fluid21,22 and are the most commonly used sequences in clinical practice .These are workhorse sequences for joint imaging because they are sensitive to both cartilage injury and other intra- and periarticular pathology.
B. MR Arthrography :
Intra-articular fluid provides contrast between the cartilage surfaces and surrounding intra-articular structures and can separate the normally coapted structures.
Synovial fluid is brighter than cartilage on PD-weighted sequences,
although it is rarely enough volume to provide the necessary contrast.
Additional fluid can also be introduced directly via an intraarticular injection (direct MR arthrography [dMRA]) or indirectly after an intravenous injection (indirect MR arthrography [iMRA]). Fat-suppressed T1-weighted sequences are most commonly used to image the hip after intra-articular gadolinium has been administered,
although additional cartilage specific sequences such as double-echo steady state (DESS)16 and 3D IDEAL SPGR VOLUME have also been studied.
C. Pathologic MR Findings in Cartilage:
Relatively few published studies evaluated the performance of MR imaging for the detection of cartilage pathology. Mintz et al in a study of 92 patients found that non contrast FSE intermediate-weighted sequences of the hip were between 88% and 93% sensitive and between 78% and 87% specific for the detection of surgically confirmed cartilage lesions.
dMRA is a widely accepted method to evaluate hip cartilage.
In a recent study showed that the overall sensitivity,
specificity,
and accuracy for the detection of cartilage pathology ranged between 50% and 79%,
77% and 84%,
and 69% and 78%,
respectively.
However,
newer MR techniques are proving that it may be possible to assess the health of cartilage before surface damage is present.
D.
Newer MR evaluation technique:
1. Compositional assessment techniques :
To evaluate the collagen network and proteoglycan content in the knee cartilage matrix:
· Sequences sensitive to collagen concentration :
- T2 mapping
- delayed gadolinium-enhanced MR imaging of cartilage (or dGEMRIC)
· Sequences sensitive to PG concentration:
- T1r imaging,
- sodium imaging
- diffusion-weighted imaging.
· Combined Evaluation of Collagen and Proteoglycan Content:
- Diffusion Tensor Imaging
These techniques may be used in various combinations and at various magnetic field strengths in clinical and research settings to improve the characterization of changes in cartilage.