This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Neuroradiology spine, MR-Diffusion/Perfusion, PET-CT, Comparative studies, Decision analysis, Cancer, Metastases
Authors:
H. M. Barragan Campos1, A. Valtierra-Rivera1, J. D. Mondragon1, O. Jiménez-Zarazúa1, J. Ortiz-Retana1, J. Altamirano-Ley2, M. Ávila-Rodríguez2; 1Queretaro/MX, 2Mexico City/MX
DOI:
10.1594/ecr2016/C-1601
Results
From April 2014 to November 2015,
56 patients (100%) were interviewed,
of which 48 (85%) met the inclusion criteria (Table 2).
Six patients (15%) were eliminated from the study due to the following reasons: 2 patients died,
1 patient had a pacemaker,
2 patients had respiratory failure,
and 1 patient did not wish to be included.
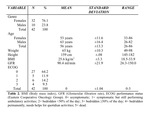
Forty-two patients (75%) were included,
of which 76% were women.
The reported primary cancer was the following: a) breast 64.2%; b) prostate 19%; c) Non-Hodgkin lymphoma 4.7%; d) cervical 4.7%; e) lung 2.3%; f) colon 2.3%; and g) testicular 2.3% (Table 3).
The reasons for inclusion were: a) clinical suspicion of BM [12] (100% of the patients); and b) imaging studies (radiography,
tomography or bone scan) with lesions suggestive of BM in 70%; and c) tumor biomarkers elevation in 14%.
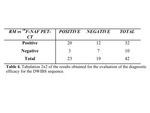
The diagnostic efficacy of DWIBS compared to 18F-NaF PET/CT,
showed sensitivity of 86.9% (CI 95%,
66.4-97.2),
specificity of 36.8% (CI 95%,
16.2-61.6),
positive predictive value (PPV) of 62.5% (CI 95%,
43.6-78.9),
negative predictive value (NPV) of 70.0% (CI 95%,
34.7-93.3),
positive likelihood ratio 1.3 (CI 95%,
0.94-2),
negative likelihood ratio 0.35 (CI 95%,
0.11-1.1) and Prevalence of 54.7% (CI 95%,
38.6-70.1) (Table 4 and 5).
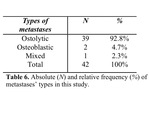
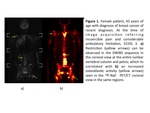
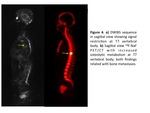
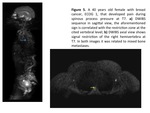
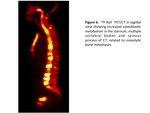
DWIBS sequence is capable of distinguish between osteoblastic (Figures 1 and 2),
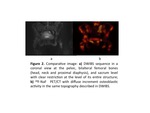
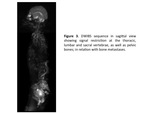
osteolytic (Figures 3,
4 and 6),
and mixed (Figure%)) bone metastases (Table 6).