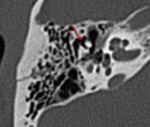
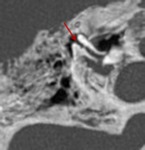
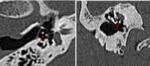
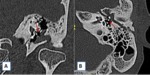
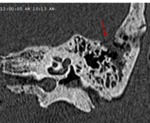
Computed tomography (CT) plays a fundamental role in the evaluation of patients with temporal bone trauma.
The most common mechanism of injury is motor vehicle crashes followed by falls and assaults.
Fractures of the temporal bone are common in patients with severe head trauma associated to skull base fractures.
Patients with temporal bone trauma also frequently have critical intracranial associated lesions such as subarachnoid,
subdural,
and epidural hemorrhage; brain contusions; and cerebral edema.
The clinical signs and symptoms of temporal bone fracture include hemorrhagic otorrhea,
hearing loss,
facial nerve paralysis,
vertigo and nystagmus.
Trauma-related conductive hearing loss can be due tympanic membrane laceration,
hematotympanum or ossicular injury
We could identify the majority of temporal bone fractures and their complications at routine head multidetector CT performed in patients with polytrauma in emergency,
without the need for dedicated temporal bone multidetector CT.
Dedicated temporal bone multidetector CT should be performed every time there is a high degree of suspicion for temporal bone fractures and no fractures are identified at routine head multidetector CT.
Sometimes the fracture line is not seen on multidetector CT but some findings are suggestive of temporal bone fracture.
These findings include opacification of mastoid air cells,
the external ear canal or the middle ear; air-fluid level in the sphenoid sinus; pneumocephalus adjacent to the temporal bone and air in the glenoid fossa of the temporomandibular joint.
It may be more important to describe the vital structures involved (ossicles,
otic capsule,
facial nerve,
tegmen,
external auditory canal,
internal auditory canal,
carotid canal) rather than trying to make the findings “fit” into a classification scheme.
I – Temporal bone anatomy
The temporal bone region is a complex anatomic region that houses many critical structures.
The temporal bone is composed of five distinct osseous components: the squamous,
petrous,
mastoid,
tympanic and styloid portions.
The petrous and mastoid portions of temporal bone are the most frequently involved in case of trauma.
External Ear:
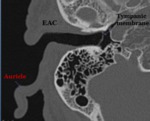
The external ear consists of the auricle and the external auditory canal (EAC),
which is located in the tympanic portion of the temporal bone.
The external auditory canal has a slight S shape; it extends from the auricle to the tympanic membrane which separates the external ear from the tympanic cavity (Fig.2).
The lateral one-third of the canal is fibro cartilaginous whereas the medial two-thirds are osseous and slightly narrower than the lateral third.
The anterior wall of the external auditory canal is composed of the posterior border of the glenoid fossa,
which houses the temporomandibular joint.
The posterior wall of the external auditory canal forms the anterior margin of the mastoid segment of the temporal bone.
Middle Ear and mastoid:
The middle ear is an air-filled cavity located in the petrous portion of the temporal bone.
It contains the ossicular chain and is bounded by the tympanic membrane laterally and lateral attic wall,
the inner ear structures medially,
the tegmen tympani superiorly,
and the jugular floor inferiorly.
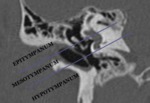
The middle ear is subdivided into the epitympanum,
the mesotympanum and the hypotympanum (Fig.3):
- The epitympanum,
or the attic,
which is superior to the level of the tympanic membrane.
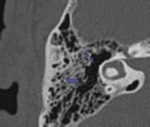
It communicates with the mastoid via the aditus ad antrum (Fig.4).
- The mesotympanum or the tympanic cavity proper,
which is opposite the tympanic membrane and contains the majority of the ossicular chain.
- The hypotympanum,
which is inferior to the level of the tympanic membrane.
It contains the opening to the Eustachian tube,
with the internal carotid artery seen along its medial margin.
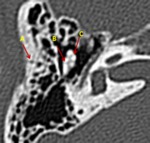
The ossicular chain is composed of three bones: the malleus,
the incus,
and the stapes.
The malleus attaches to the tympanic membrane and consists of the head,
neck,
anterior process,
lateral process,
and manubrium (Fig.5).
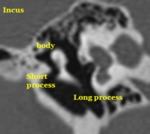
The incus is formed by a body and a long,
short,
and lenticular process (Fig.
6).
The stapes is the most medial ossicle,
consisting of a head,
anterior and posterior crura,
and a footplate (Fig.7).
The manubrium of the malleus is attached to the tympanic membrane.
The head of the malleus articulates with the body of the incus forming the incudomalleal joint,
which constitute the “ice cream cone” configuration on axial sections (Fig.8,
9)
The lenticular process of the incus articulates with the head of the stapes forming the incudostapedial joint (Fig.
9,10) .
The footplate of the stapes is attached to the oval window of the vestibule.
The mastoid is an air-filled cavity divided into numerous compartments by mastoid septations.
The mastoid air-cell size and configuration are highly variable.
Inner ear:
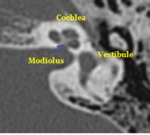
The inner ear lies within the petrous portion of the temporal bone and consists of three structures: the cochlea,
the vestibule,
and the semicircular canals (Fig.11).
The densest portion of the temporal bone that surrounds the osseous labyrinth is termed the otic capsule.
The cochlea contains the end organ for hearing while the vestibule and semicircular canals are involved with balance and equilibrium.
The cochlea is a spiral-shaped structure with 2 ½ to 2 ¾ turns,
including the basal,
middle,
and apical turns,
which are separated by interscalar septae.
It consists of a bony canal wound around a conical central core called the modiolus.
The bony vestibule is an ovoid space located superior and posterior to the cochlea,
which connects to the semicircular canals.
The vestibule is continuous anteriorly with the cochlea and posteriorly with the semicircular canals.
There are three semicircular canals: superior,
posterior,
and lateral which are oriented orthogonal to one another.
4 – Facial Nerve (Cranial Nerve VII)
The facial nerve exits the lateral pons,
traverses the cerebellopontine angle (cisternal segment),
passes through the porus acousticus,
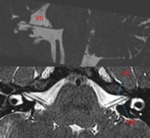
courses through the internal auditory canal (canalicular segment) (Fig.12).
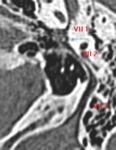
The facial nerve takes a winding path through the petrous bone and its course is divided into three basic segments: the labyrinthine,
the tympanic,
and the mastoid segments (Fig.14).
- The labyrinthine segment of the facial nerve (VII 1) emerges from the anterosuperior aspect of the internal auditory canal,
coursing anterolaterally within its own bony channel,
the fallopian canal.
This segment of the facial nerve is relatively short,
measuring 3–4 mm,
and lies superior to the cochlea.
It makes a subtle anteromedial turn as it courses anteriorly to reach the geniculate ganglion (Fig.13).
From here (anterior or first genu),
the facial nerve turns posteriorly toward the medial aspect of the middle ear cavity (tympanic segment).
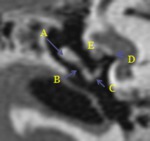
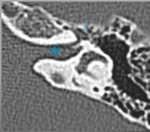
- The tympanic segment of the facial nerve (VII 2) is approximately 12 mm long and extends from the geniculate ganglion to the posterior genu.
It runs inferior to the lateral semicircular canal and superolateral to the oval window (Fig.10).
In the posterior wall of the middle ear cavity adjacent to the facial recess,
the facial nerve turns inferiorly forming the posterior or second genu.
- The mastoid segment of the facial nerve (VII 3) is the longest portion of the intratemporal facial nerve,
measuring approximately 15–20 mm.
It courses through the medial portion of the mastoid bone until it exits the temporal bone through the stylomastoid foramen and enters the parotid gland.
II –Classification of Temporal Bone Fractures:
Classifying temporal bone fractures helps physicians understand and predict associated complications and guide treatment.
The traditional classification system classified temporal bone fractures into two main categories,
transverse or longitudinal,
according to the orientation of the fracture line to the long axis of the petrous portion of the temporal bone.
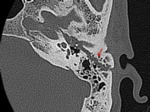
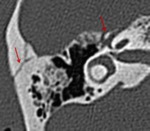
· Longitudinal fracture type:
The longitudinal fracture type is more common (80%–90% of temporal bone fractures) and results from temporo-parietal impact with the line of force extending lateral to medial.
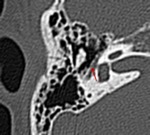
The fracture line is parallel to the longitudinal axis of the petrous portion of the temporal bone (Fig.15).
Involvement of the otic capsule is rare.
Longitudinal fractures typically traverse the middle ear cavity,
with frequent disruption of the ossicles.
The most common complications of longitudinal fractures are ossicular and tympanic membrane injury and hemotympanum with conductive hearing loss.
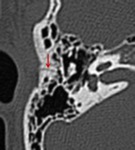
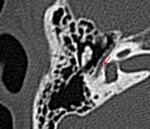
· Transverse Fractures:
The transverse fracture type is less common (10%–20%) and results from fronto-occipital trauma with the line of force extending anterior to posterior.
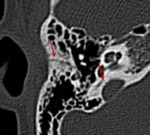
The fracture line is perpendicular to the longitudinal axis of the petrous portion of the temporal bone with variable involvement of the otic capsule (Fig.16).
Facial nerve injury is more common in patients with a transverse fracture
Sensorineural hearing loss is also more common with this type of fracture and may be secondary to injury to the labyrinthine structures or stapes footplate injury,
which results in perilymphatic fistula.
But some temporal bone fractures may not be strictly classified as longitudinal or transverse.
These type of fracture can be defined as mixed or oblique fracture
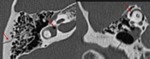
· Mixed Fractures:
Mixed fractures include both longitudinal and transverse elements,
with frequent involvement of the otic capsule.
The traditional classification system does not correlate with clinical findings and prognostic.
Therefore,
newer classification systems have been proposed that describe temporal bone fractures according to the involvement or respect of the petrous apex or otic capsule.
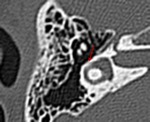
Another system classified fractures into petrous and non petrous types.
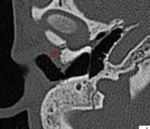
· Petrous fractures involve the petrous apex and otic capsule and are associated with facial nerve injury,
cerebrospinal fluid leak and sensorineural hearing loss.
· Non petrous fractures involve the middle ear and mastoid with an increased frequency of conductive hearing loss due to involvement of the ossicular chain (Fig.17).
There is a newer system that classifies fractures depending on whether the otic capsule is spared (otic capsule–sparing fracture) or violated (otic capsule-violating fracture).
· The otic capsule–sparing fracture is much more common (94%–97%),
results from a temporoparietal blow and has an increased incidence of conductive hearing loss due to ossicular injury.
They are more commonly associated with intracranial injuries.
· The otic capsule–violating fracture (3%–6%) results from an occipital blow and are more commonly associated with complications such facial nerve injury,
sensorineural hearing loss,
otorrhea and cerebrospinal fluid fistula.
On CT images,
the otic capsule–violating fracture line can involve the cochlea,
vestibule,
semicircular canals and facial nerve.
The otic capsule–sparing or otic capsule–violating classification system seems to be the most valuable to help predict clinical outcomes and to tailor the treatment of patients with temporal bone fractures.
III – Identification of Important Structures
Identifying injury to critical structures is more important for guiding management and determining prognosis than simply classifying temporal bone fractures into category.
Indeed; for a proper evaluation of patients with temporal bone trauma,
some structures need to be identified at CT examination; these structures include the external auditory canal,
ossicles,
cochlea,
vestibule,
and semicircular canals facial nerve canal and carotid canal.
1 – External auditory canal:
The external auditory canal and the temporomandibular joint should be adequately evaluated in the axial and coronal MPR planes.
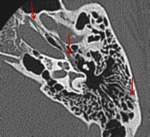
Fracture of the anterior wall of the external wall of the EAC may result from impaction of the condyle into the posterior wall of the temporomandibular joint or be a direct consequence of a fracture line extending into the external auditory canal (Fig.17,18).
Unseen fractures may lead to subsequent canal stenosis.
2 – Ossicular injury:
Ossicular injury is usually seen with longitudinal fractures or otic capsule–sparing fractures of the temporal bone.
High-resolution computed tomography is the method of choice for evaluation of ossicular injury.
However,
the radiologist must have a precise knowledge of normal anatomy of the ossicular chain as seen on axial,
coronal and reformatted CT images to diagnose these injuries.
Ossicular dislocation is more common than ossicular fracture.
There are five types of dislocation: incudostapedial joint separation,
incudomalleolar joint separation,
incus dislocation,
incudomalleal complex dislocation,
and stapediovestibular dislocation.
The incus is the most vulnerable ossicle to injury.
Therefore,
most ossicular dislocations or subluxations involve the incus.
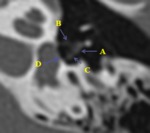
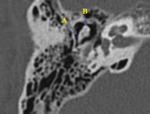
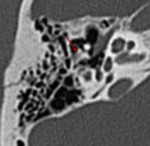
Incudomalleolar joint separation is visualized on axial CT scans as a displacement of the head of the malleus (the scoop of ice cream) from the body and short process of the incus (the cone of the ice cream) (Fig.19,20).
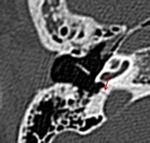
Incudostapedial joint disruption appears,
on axial CT scans or oblique reconstructions,
as a gap between the head of the stapes and the long process of the incus (Fig 21,
22).
But CT findings of ossicular injury may be difficult to evaluate in emercency because of hemotympanum.
Incus dislocation occurs when there is incudomalleal and incudostapedial joint separation concomitantly.
Stapediovestibular dislocation creates a perilymphatic fistula.
Isolated fracture of the malleus,
incus,
or stapes is uncommon (Fig.23).
The long process of the incus is the more likely to be fractured because of its lack of support,
followed by the crura of the stapes (Fig.24).
Fracture of the malleus is rare and usually involves the neck region.
3 – Carotid Canal:
The petrous segment of the internal carotid artery enters the skull through the carotid canal,
medial to the styloid process and anterior to the jugular fossa.
The carotid canal should be evaluated along its length on CT (Fig.25).
Patients with fractures that extend to the carotid canal are more likely to have carotid artery injury.
4 – Venous Injury:
Venous injury should be suspected when the fracture line traverses the sigmoid sinus or the jugular foramen (Fig.26,
27).
CT with contrast should be performed in suspected cases of veinous injury which can manifest as transaction or thrombosis.
5 – Facial nerve:
The facial nerve should be evaluated along its length in the axial plane and reformatted CT imaging.
The facial nerve is more frequently injured in patients with transverse and otic capsule-violating temporal bone fracture.
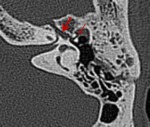
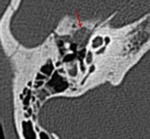
Most injuries occur in the labyrinthine segment,
in the region of the geniculate ganglion (Fig.28,
Fig.
29).
The facial nerve must be evaluated with care to identify osseous fragments or hematomas that may compress the facial nerve (Fig30,
31).
6 – Cochlea and vestibule:
In addition to axial images,
MPR images are useful in identifying injury cochlea or vestibule (Fig.31).
Injury to the cochlea is associated with sensorineural hearing loss whereas vertigo frequently occurs after temporal bone trauma in case of injury to vestibule.
A Perilymphatic fistula which is an abnormal communication between the middle ear and inner ear may occur with injury to the otic capsule.
Perilymphatic fistula manifests clinically as vertigo and sensorineural hearing loss.
Pneumolabyrinth and opacification of the round window are important CT findings of perilymphatic fistula (Fig.32).
7 – Semicircular Canals:
Each semicircular canal should be evaluated individually in the orthogonal coronal,
axial,
and sagittal planes (Fig.33).
As with vestibular injuries,
trauma to the semicircular canals results in vertigo.
8 – Cerebrospinal fluid (CSF) leak:
CSF leak is seen in temporal bone fractures involving the tegmen and in case of otic capsule-violating fractures (Fig.34).
Clinically,
patients present with otorrhea or rhinorrhea.