We will discuss ovarian masses based on their morphologic appearance (cystic,
mixed or solid) listing the possible histological and their common RM features [1,2,5].
Note that the majority of the tumours belong to more than one morphologic type.
You can review the ovarian tumours classification by histological subtype in (table 1) [4].
It is important to have in mind that approximately 90% of malignant tumours are of epithelial origin.
Serous are the most common subtype followed by mucinous,
endometrioid and clear cell.
Unfortunately,
most patients present with disseminated disease.
Malignant germ-cell tumours occur in younger patients and include dysgerminoma,
endodermal sinus tumour and immature teratoma.
MRI technique: 1-1,5 T.
We recommend administering an antiperistaltic drug intramuscularly or intravenously before the examination.
| T2w TSE in sagital and axial and coronal planes
T1w TSE in axial plane
T1w and T2w axial with a selective chemical fat-suppression technique
T1w FFE in\out phase
DWI
3D GRE- T1W FT
3D GRE- T1W FT dynamics - after paramagnetic intravenous contrast
|
Benign vs malignant mass [5]: contrast-enhanced study is essential
-
An unilocular/simple cyst is a benign mass.
-
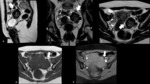
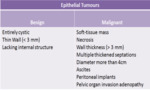
A malignant mass is highly suspected when primary or ancillary criteria are present (Fig.1)(table 2) [6].
When used,
the sensitivity for classifying as malignancy is 91-100% and specificity is 91-92%[7].
-
A cystic and solid mass is malignant unless it is a mature teratoma.
-
If a mass is not an unilocular cyst or does not have primary or ancillary criteria for malignancy,
nothing can be said about the benignity or malignancy of the mass (Fig.2).
Differential diagnosis by morphologic appearance [1,2]:
-
Unilocular cyst (table 3)
1.1 Functional cyst:
-
women of reproductive age or up to 5 years after menopause
-
generally regress after 2-3 months,
so that if still present in 2-3 month follow-up can be excluded
-
size: from 3 to 8 cm
-
may bleed--> classic presentation of acute abominal pain,
however can be asymptomatic.
Pitfall: haemorrhage automatically includes endometrioma in the differential diagnosis .
1.1.1 Graaf folicle
1.1.2 Corpus luteum cyst
1.2 Paraovaric cyst:
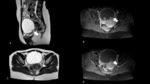
1.3 Hydrosalpinx (Fig.
3):
1.4 Serous cystadenoma :
2.
Multilocular cyst (table 4)
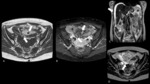
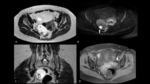
2.1 Endometrioma (Fig.4):
-
Haemorrhagic,
so high signal intensity on T1w images that does not suppress after fat-supressed sequences (versus fat in teratoma); on T2w images it is typically hypointense (due to deoxyhemoglobin and methamoglobin) called “shading sign”
-
T2 “dark spot sign” is specific for chronic haemorrhage
-
Persistence after 6 months confirms endometrioma and excludes haemorrhagic cyst
2.2.
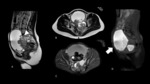
Mucinous cystadenoma (Fig.5-Fig.6):
-
Most commonly unilateral (vs serous cystadenoma)
-
Contains fluid of various viscosity,
due to this reason the loculi of the tumours often show variable signal intensity on both T1 and T2 sequences “stained-glass appearance”
2.3 Borderline mucinous cystic tumours:
2.4 Serous cystadenoma (less common) (Fig.
7)
2.5 Granulosa cell tumours:
-
95% adult-type and most commonly occur in postmenopausal women
-
The most common malignant estrogenic tumour,
so associated uterine enlargement with endometrial hyperplasia may be demonstrated on T2-weighted images.
2.6 Purely cystic atypical mature teratoma
3.
Mixed (solid + cystic) mass (table 5): A mixed mass strongly suggests malignancy,
the notable exception is the mature cystic teratoma
3.1 Epithelial tumours:
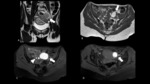
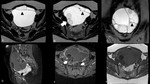
3.1.1Serous cystadenocarcinoma (Fig.8-Fig.9):
-
Peak prevalence 6th-7th decades
-
CA-125 elevated in about 90% of patients
-
Frequent,
but not necessary associated findings: papillary projections,
psammomatous calcification,
bilaterality,
carcinomatosis
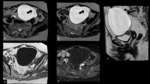
3.1.2 Mucinous cystadenocarcinoma:
-
Variable fluid intensity on both T1 and T2
-
Frequent,
but not necessary associated findings: linear calcifications,
carcinomatosis presents as pseudomyxoma peritonei
-
Pitfall: may mimic metastasis to the ovary from intestinal carcinoma
3.1.3 Endometroid tumour:
3.1.4 Malignant Brenner tumour
3.1.5 Borderline tomours (Fig.10)
3.2 Germ-cell tumours:
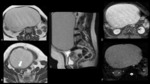
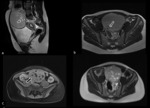
3.2.1 Mature teratoma (Fig.11):
-
Arise in young women (age 10-30 years)
-
Presence of fat is highly specific (use fat-suppressed sequences se to distinguish from endometrioma)
-
Cystic component in most cases is unilocular
-
Associated findings include: areas of low-signal intensity (teeth),
soft-tissue protuberances,
floating debris,
calcifications limited to the mural nodules (vs immature teratoma)
-
May complicate with torsion,
rupture (leading to granulomatous peritonitis) and malignant degeneration
-
Immature teratoma is extremely rare and may be differentiated from mature due to the presence of haemorrhage,
necrosis,
scattered calcifications and perforation of the capsule.
3.2.2 Endodermal sinus tumous
3.3 Granulosa cell tumour
3.4 Metastatic disease:
-
Most commonly bilateral
-
Most commonly from stomach,
colon,
breast,
lung and contralateral ovary
-
Mucinous lesions more frequently metastatic disease than primitive mucinous
4 Solid mass: (table 6) Include benign,
malignant and borderline masses.
4.1 Epithelial ovarian carcinoma
4.2 Metastatic disease
4.3 Granulosa cell tumour
4.4 Dysgerminoma:
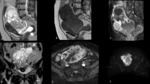
4.5 Fibroma,
fibrotechoma (Fig.
12) and techoma:
-
Belong to the same histologic spectrum
-
Differential diagnosis with non-degenerated subserosal uterine leiomyomas,
flow-void sign indicates leiomyoma (present in 85% of the leiomyomas with more than 7cm)
4.6 Brenner tumours:
4.
7 Mature teratoma

![Table 1: Classification of Ovarian Tumours [4]](https://epos.myesr.org/posterimage/esr/ecr2017/137349/media/689749?maxheight=150&maxwidth=150)

![Table 3: Unilocular cyst [1]](https://epos.myesr.org/posterimage/esr/ecr2017/137349/media/694117?maxheight=150&maxwidth=150)

![Table 4: Multilocular Cyst [1]](https://epos.myesr.org/posterimage/esr/ecr2017/137349/media/694121?maxheight=150&maxwidth=150)
![Table 5: Mixed lesions [1]](https://epos.myesr.org/posterimage/esr/ecr2017/137349/media/694132?maxheight=150&maxwidth=150)
![Table 6: Solid Masses [1]](https://epos.myesr.org/posterimage/esr/ecr2017/137349/media/694134?maxheight=150&maxwidth=150)