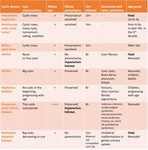
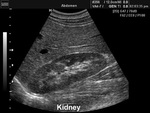
We suggest and describe the following classification of the cystic renal masses in children:
1. Neoplasia (benign and malignant,
both groups present as large abdominal mass)
1.1. Mesoblastic nephroma
1.2. Multilocular Cystic Renal Tumor
1.3. Wilms tumour – cystic form
2. Congenital ciliopathies (genetic) *
2.1. Polycystic renal disease (autosomal dominant and autosomal recessive)
2.2. nephronophthisis - medullary cystic disease complex
3. Dysplastic renal diseases
3.1. Multicystic Dysplastic Kidney
3.2. Glomerulocystic Kidney Disease
4. Multiple Malformation Syndromes with Renal Cysts- tuberous sclerosis,
von Hippel-Lindau disease etc.
5.
cysts- simple and complicated cyst,
acquired cyst
(fig.
1,
table 1)
* (explanation of cilia)
Cilia line the ducts of the kidney and liver and have recently been shown to be integral to proper renal and hepatic development.
The kidneys are the most commonly affected organs in ciliopathies,
with effects ranging from mild urinary concentration defects in normal-appearing kidneys to cystic,
dysplastic kidneys.
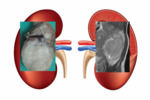
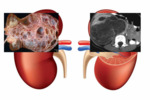
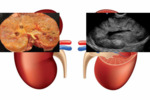
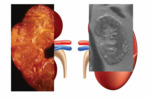
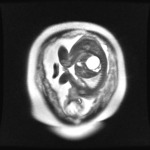
Mesoblastic Nephroma (fig.2)
Mesoblastic nephroma is the most common renal tumor in the fetus and neonate,
diagnosed within the first 3 months of life.
It is a benign hamartoma with excellent prognosis,
becouse nephrectomy is curative.
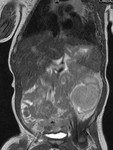
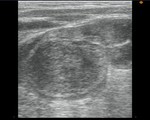
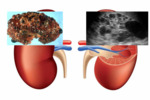
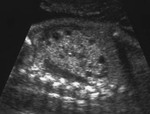
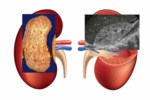
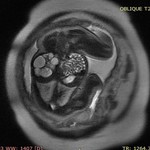
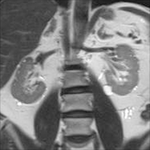
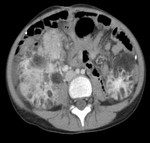
US is the preferred imaging modality.
Regardless of imaging modality,
pitfall is to demonstrate a smooth,
solitary renal mass with a normal adrenal gland.
Lack of hemorrhage,
calcification,
and necrosis are other imaging characteristics.
(fig.
3,
fig.4,
fig.5)
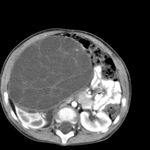
Multilocular Cystic Renal Tumor (fig.6)
cystic nephroma(CN) and cystic partially differentiated nephroblastoma (CPDN)
Multilocular cystic renal tumor refers to two entities that cannot be distinguished on the basis of gross pathology or radiologic findings.
Multilocular cystic renal tumor is a benign lesion composed of multiple noncommunicating cysts separated by septa.
Nephroblastoma is typically a benign lesion; however,
local recurrence after nephrectomy may occur.
The prognosis for these malignancies is better than their corresponding non-cystic tumors (i.e.,
Wilms’ tumor and RCC).
On ultrasound,
the kidney appears as a multiloculated mass with thin septa.
The renal parenchyma can be compressed by the renal mass forming a thin rim of parenchyma (beak sign).
On nonenhanced CT,
multilocular cystic renal tumors appear as sharply circumscribed,
multiseptated renal mass.
The interior of the cysts show attenuation that is consistent with water.
With contrast,
the septations may enhance.
On MRI,
the septa and renal capsule appear as low signal intensity on T1-weighted images.
The septa enhance after gadolinium administration.
On T2-weighted images,
the fluid contents of the cyst display high signal intensity.
(fig.7,
fig.
8)
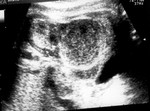
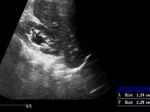
Autosomal Recessive Polycystic Kidney Disease ARPKD (fig.9) is cystic dilation of the renal collecting tubules.
On US the kidneys are hyperechoic and enlarged bilaterally,
with disrupted echotexture due to microcysts (too small to be resolved by US),
with or without some dilatation of collecting system.
Often ARPKD is associated with liver fibrosis.
(fig.10)
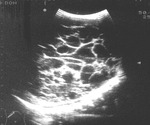
Autosomal Dominant Polycystic Kidney Disease ADPKD (fig.11)
ADPKD present with only a few detectable larger renal cysts that increase with age.
The cysts increase and multiply and replace the parenchyma.
(fig.12)
They are associated with cysts the liver,
with berry- aneurysms in the brain and with hyperplastic polyps in colon.
Nephronophthisis NPHP or Medullary Cystic Disease Complex (fig.
13) is chronic diffuse tubulointerstitial nephritis that progresses to fibrosis and terminal renal failure.
NPHP literally means “disappearance of nephrons,” which alludes to its histopathology,
with interstitial fibrosis and corticomedullary cysts replacing normal renal tissue.
(fig.14)
The disease is bilateral and the kidneys are usually small at the time of diagnosis,
typically in the first decade.
In nephronophthisis US demonstrates kidneys of increased echogenicity with poor corticomedullary differentiation.
Macrocysts are typically seen after the onset.
Renal cysts develop progressively and become more common with advancing age.
Associated presenting signs and symptoms include polyuria,
Fanconi syndrome,
growth retardation,
retinitis pigmentosa.
Multicystic Dysplastic Kidney (fig.
15) is the most common cystic malformation.
Said to originate from severe early upper tract obstruction causing severe cystic dysplasia.
The renal cysts are noncommunicating and there is no functioning parenchyma and no central pelvis in the affected kidney.
Commonly tend to shrink spontaneously; however,
some may grow,
get infected,
cause hypertension or undergo tumorous transformation.
US monitoring is recommended.
Compensatory hypertrophy is seen routinely in the functioning kidney.
Often associated with ipsilateral genital malformations.
Glomerulocystic Kidney Disease (fig.19) is inherited sporadic disorder without familial pattern.
Pathologically it is dilatation of the Bowman’s spaces of the glomeruli.
US imaging findings are similar to polycystic kidney disease.
The kidneys may be normal- sized,
enlarged or hypoplastic.
The predominant imaging finding is small renal cysts with a primarily cortical subcapsular distribution.
The cysts may be difficult to define at US,
and cortical hyperechogenicity may be seen instead of the typical anechoic appearance of simple cysts.
Patients typically present with symptoms of renal failure.
Nonenhanced T2-weighted MR imaging is the preferred imaging modality.
(fig.20)
Glomerulocystic kidneys are major components of heritable syndromes such as tuberous sclerosis,
orofaciodigital syndrome,
brachymesomelia-renal syndrome,
trisomy 13,
and the short rib-polydactyly syndromes.
Many syndromes can present with renal cysts.
Common syndromes encountered with renal cysts are tuberous sclerosis and von Hippel-Lindau disease.
Tuberous sclerosis complex is associated with multiple simple cortical renal cysts (20 % of patients),
renal angiomyolipoma (40–80 %),
and renal cell carcinoma (2 %).
US demonstrates highly echogenic non-shadowing foci,
representing the fatty components in angiomyolipomas.
CT can be useful in demonstrating the presence of fat of angiomyolipoma.
(fig.21)
It has been shown that angiomyolipomas grow in adults and can distort renal architecture,
which compromises function and can lead to hemorrhage.
Cysts – (fig.
22,
fig.23)
• Simple cyst: (isolated/single) uncomplicated cyst (no content/completely anechoic,
smooth margin,
thin wall,
no solid component,
etc.),
localised,
with or without growth.
Rarely seen in neonates and infants.
• Multiple cysts: often associated with parenchymal dysplasia or genetic/inherited cystic kidney disease.
• Complicated cyst: as anywhere else – internal echoes and sedimentation,
septae,
thick wall,
irregular border,
solid/nodular components,
conglomerates of cysts,
large,
irregular shape; vascularised compartments.
- Acquired Cystic Kidney Disease- Number of etiologies occur and exhibit different features: posttraumatic cysts,
postoperative cysts,
acquired cystic kidney disease in renal failure and after transplantation.
Decision-Tree Approach to Renal Cystic Diseases
When there is a suspicion of cystic components within the renal parenchyma,
the evaluation should exclude hydronephrosis at the first place,
then multicystic dysplastic kidneys.
The first step is to rule out obstructive uropathy,
in which there is often dilatation of the collecting system (hydronephrosis).
It can be unilateral or bilateral.
The affected kidneys are of variable size; the cortex is usually hyperechoic,
thinned,
and irregular; and the CMD is absent.
Multicystic displastic kidneys is the second diagnosis to consider.
After exclusion of hydronephrosis and MCDK inherited renal cystic disease should be considered.
Cysts usually have typical pattern.
A typical pattern means all sonographic features have a typical pattern of cysts (size,
location,
number),
appearance of the parenchyma (echogenicity,
CMD),
size of cystic mass (bigger are the neoplastic lesions such as nephroma) and renal size that leads to a specific diagnosis (isolated or associated with other malformations).
(see fig.1)
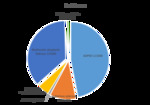
IMAGING MODALITIES
Imaging modalities used in diagnosis of cystic renal masses are (fig.
24) ultrasound US,
magnet-resonance imaging (MRI),
computed tomography (CT) and eventually voiding cystourethrogram (VCUG) and scintigraphy (scinti).
The best imaging modality for cystic masses is US- both prenatal (fetal sonography) and postnatal abdominal US.
All imaging modalities are listed below.
ULTRASOUND
Fetal Kidney should be evaluated during the middle trimester of pregnancy
- Progressive corticomedullary differentiation (CMD) can be visualized as an echogenic cortex and a hypoechoic medulla.
- Renal cortical echogenicity compared with the liver and spleen decreases with progression of pregnancy- in third trimesters it should appear hypoechoic compared with the liver and spleen.
Neonatal Kidney
- The neonatal kidney measures 3.5–4.5 cm in the long axis.
- All neonatal kidneys should have typical CMD.
The cortex is relatively isoechoic or hyperechoic compared with liver and spleen.
Pediatric Kidney
- The kidney grows with age.
- The renal cortex is usually hypoechoic compared with the liver and isoechoic compared with the spleen.
Echogenicity of the Kidney in the Context of Cystic Renal Disease
- Renal cystic diseases have two sonographic patterns: cysts and renal hyperechogenicity,
which can be associated with each other.
- The cysts are anechoic round structures with sharply circumscribed smooth walls and enhanced through-transmission.
They can be tiny/ barely measurable,
or large,
measuring several centimeters.
They can develop anywhere in the kidney.
- Characteristic radiologic findings of cysts include number,
location,
size,
wall thickness,
associated calcifications,
and septations.
- Renal hyperechogenicity is related to the numerous interfaces created by microscopic cysts and dilated tubules.
- A detailed ultrasound examination includes measuring renal size,
defining the echogenicity of the cortex (hyperechoic,
isoechoic,
hypoechoic compared with liver and spleen) and medulla (hypoechoic,
anechoic,
hyperechoic),
assessing the CMD (present,
absent,
reversed),
evaluating for cysts (number,
size,
location) and calcifications,
and assessing the pelvicaliceal system.
Color Doppler assessment is useful in selected cases.
- During pregnancy,
the examination should include a survey of the entire fetus to check for associated malformations.
The liver and genital tract should be evaluated.
MRI
- In some patients,
MRI (prenatal and postnatal) can yield additional important information by showing renal cysts,
associated brain malformation,
and liver abnormalities,
not detectable with ultrasound.
For kidneys and the brain,
T2-weighted sequences are usually sufficient.
CT
- performed in cases where MRI is not available.
- CT urogram is a contrast-enhanced study where iodine contrast material is injected i.v.
and kidneys are scanned 5 to 10 minutes after contrast administration.
Renal excretory function (or the possibility of kidney/ both kidneys to filtrate the urine with contrast media) is shown.
VOIDING CYSTOURETRIGRAM is an X-ray study,
where the bladder is filled with CM trough a catheter.
Imaging is performed during voiding.
We can examine if reflux will occur (vesico-uretheral reflux)
SCINTIGRAPHY is a diagnostic test in nuclear medicine,
helping with additional information about renal function or in cases with ectopic renal remnants.