This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Infection, Abscess, Abscess delineation, MR, CT, Musculoskeletal soft tissue, Head and neck, Emergency, Inflammation
Authors:
M. Perez1, E. C. MEDINA2, M. Noriega3, M. C. Arango3, V. palacio3; 1Medellin, Antioquia/CO, 2MEDELLIN, AN/CO, 3Medellin/CO
DOI:
10.1594/ecr2017/C-0720
Findings and procedure details
The different methods of diagnostic imaging provide several keys for the diagnosis of pyomyositis.
Noninvasive radiologic methods,
such as ultrasound,
CT,
or MR imaging,
are useful in confirming the diagnosis but is not especifics.
Plain radiographs are not sensitive,
may suggest muscle enlargement,
loss of muscle definition,
obliteration of deep fat planes,
gas in soft tissues,
and reactive changes in adjacent bone.
X ray is more useful excluding differential diagnosis like osteomyelitis or musculoskeletal tumors.
Ultrasound is the initial screening tool,
shows hypoechoic areas with increased muscle bulk.
(Fig.
1)
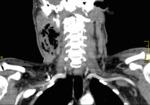
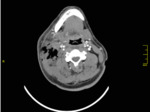
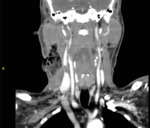
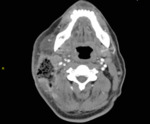
CT can visualize pyomyositis as areas of low attenuation with loss of muscle plain surrounded by a rim of contrast enhancement,
associated with swelling of fascial planes.
(Fig.
2 - 5)
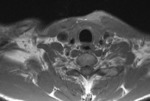
MR imaging is more specific and sensitive compared with CT.
It usually presents as illdefined muscle enlargement with hyperintensity on T2-weighted images with abnormal signal intensity of the nearby bone,
or fluid in the joint.
If there are fluid collection within the muscle may be visible as hyperintense on T2-weighted images and isointense to hypointense on T1- weighted images.
Postcontrast T1-weighted imaging study shows rim enhancement,
suggesting an abscess along with uniform enhancement of the involved muscles,
similar to CT.
Diffusion-weighted imaging (DWI) has been reported to help in differentiating abscess from tumor in the neck; but in pyomyositis is not clear the specific features (Fig.
6)