Image findings
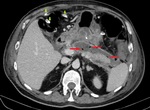
Interstitial edematous pancreatitis (IEP) - the most common form of acute pancreatitis
- diffuse pancreatic parenchyma enlargement (occasionally localised) due to inflammation
- homogeneous enhancement by intravenous contrast agent (i.e.
no areas of pancreatic necrosis)
- mild peripancreatic fat stranding or haziness
- with or without peripancreatic fluid collections (with no solid component)
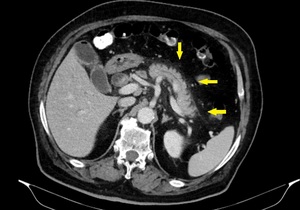
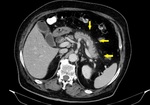
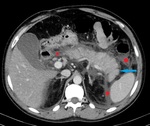
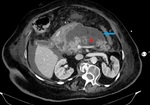
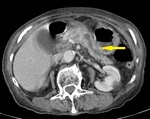
Fig. 1: IEP in a 77-year-old man with gallstone-related pancreatitis. Axial contrast-enhanced CT image shows wispy peripancreatic inflammation (yellow arrows) with normal pancreatic enhancement and no collections.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
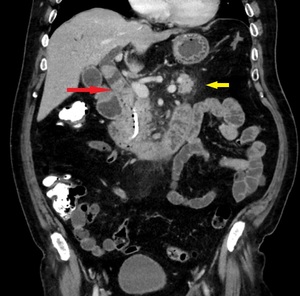
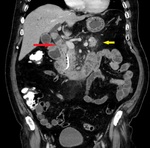
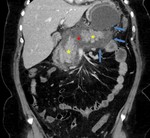
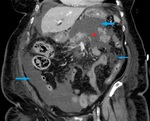
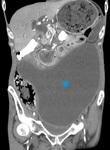
Fig. 2: Same patient as in Fig. 1. Coronal image shows the choledocholithiasis (red arrow) and peripancreatic haziness (yellow arrow).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
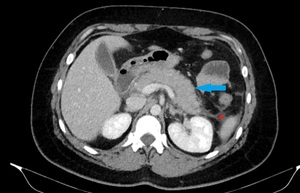
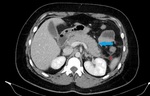
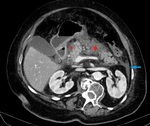
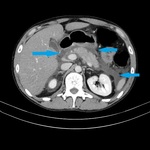
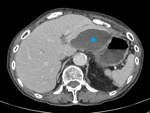
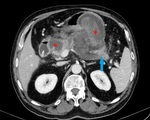
Fig. 3: IEP in a 30-year-old woman. Axial contrast-enhanced CT image shows enlargement with normal pancreas enhancement (blue arrow) and minimal peripancreatic fluid collection (red star).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
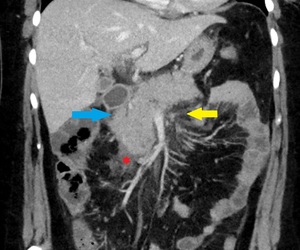
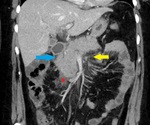
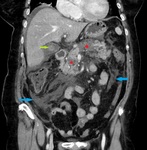
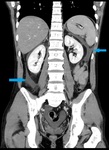
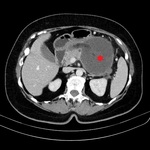
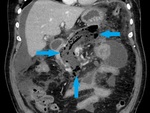
Fig. 4: Same patient as in Fig. 3. Fat stranding (yellow arrow). Enlargement of the pancreas with normal enhancement (blue arrow) and minimal peripancreatic fluid collection (red star).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
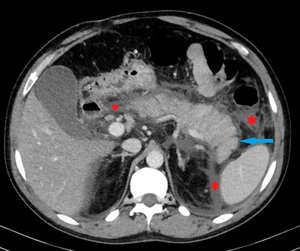
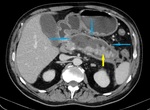
Fig. 5: IEP in a 41-year-old man. Axial contrast-enhanced CT image shows normal enhancement of the pancreas with focal enlargement (blue arrow) and homogeneous fluid-attenuation collections adjacent to the pancreas, anterior to the left pararenal fascia and in the left paracolic gutter space (red stars), findings that are consistent with APFCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
Necrotising pancreatitis
There are three forms of necrotising pancreatitis,
depending on location: pancreatic parenchymal necrosis alone,
peripancreatic necrosis alone and pancreatic parenchymal necrosis with peripancreatic necrosis (in 75% of patients with acute necrotising pancreatitis) [11].
- Pancreatic parenchymal necrosis is defined as a lack of enhancement by intravenous contrast agent (the extent should be reported as <30% or >30%)
- Peripancreatic necrosis is defined as heterogeneous areas of enhancement that contain non-liquefied components,
commonly located in the retroperitoneum or lesser sac.
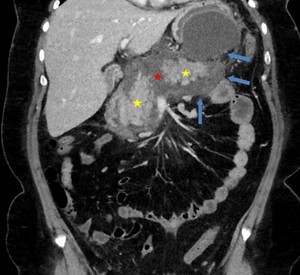
Fig. 6: Necrotising pancreatitis in a 37-year-old woman. Coronal contrast-enhanced CT image shows an area of nonenhancement in the neck of the pancreas (red star), normal enhancement of the head and body (yellow stars) and peripancreatic heterogeneous collection (blue arrows), a finding consistent with ANC.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
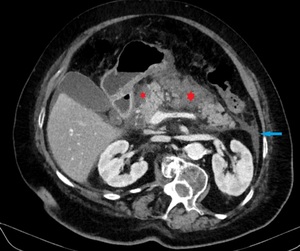
Fig. 7: Necrotising pancreatitis in a 79-year- old woman. Axial CECT image shows multiple areas of abnormal pancreatic parenchymal enhancement (red stars) and a collection in the left anterior pararenal space (blue arrow).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
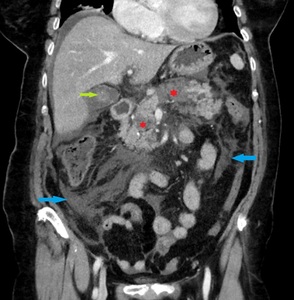
Fig. 8: Same patient as in Fig. 7. Multiple areas of abnormal pancreatic enhancement (red stars), collections distributed in the entire abdomen (blue arrows) and the presence of a gallstone (green arrow).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
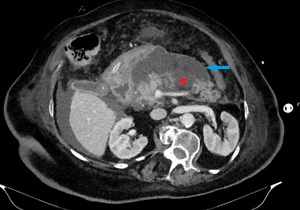
Fig. 9: Same patient as in Fig. 7. Image acquired after 2 weeks shows the progression of the parenchymal necrosis (red star) and a heterogeneous collection containing both fluid and non-fluid densities (blue arrow), a finding that is consistent with ANC.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
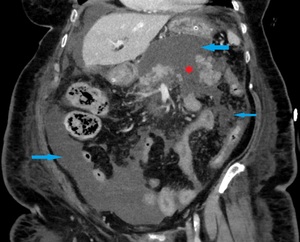
Fig. 10: Same patient as in Fig. 7. Coronal image acquired after 2 weeks shows the progression of the parenchymal necrosis (red star) and heterogeneous collections containing both fluid and non-fluid densities (blue arrows), a finding that is consistent with ANCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
Pancreatic and Peripancreatic Collections
The morphological description of these local complications provides an accurate diagnosis.
It includes location (pancreatic,
peripancreatic,
other),
content nature (fluid,
non-liquefied material,
gas) and wall thickness,
if any (thin or thick) [2].
The wall usually develops after 4 weeks,
thus collections seen within the first 4 weeks after onset are categorised as acute collections.
All of these collections can be sterile or infected,
but collections that contain non-liquefied material are much more likely to become infected.
The distinction is important because treatment and prognosis are different [12].
IEP can be associated with acute peripancreatic fluid collections (APFCs) and pancreatic pseudocysts.
APFC
- peripancreatic homogeneous collection with fluid-attenuation density (without non-liquefied components) arising within the first 4 weeks after onset
- confined by normal peripancreatic fascial planes and without intrapancreatic extension
- without a definable encapsulating wall
*A fluid collection within the pancreatic parenchyma should not be labelled as APFC but as ANC.

Fig. 5: IEP in a 41-year-old man. Axial contrast-enhanced CT image shows normal enhancement of the pancreas with focal enlargement (blue arrow) and homogeneous fluid-attenuation collections adjacent to the pancreas, anterior to the left pararenal fascia and in the left paracolic gutter space (red stars), findings that are consistent with APFCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
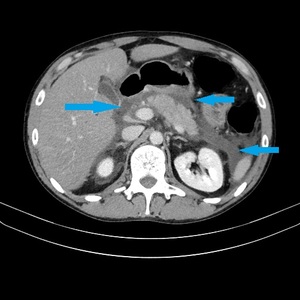
Fig. 11: IEP in a 26-year-old man. Axial contrast-enhanced CT image shows homogeneous pancreatic enhancement and several collections with fluid-attenuation densities (blue arrows), marks of APFCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
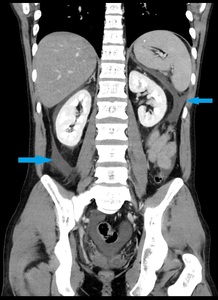
Fig. 12: Same patient as in Fig. 11. Coronal contrast-enhanced CT image shows collections with fluid-attenuation densities (blue arrows) that are confined by the normal anatomical fascial planes. These findings are consistent with APFCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
Pseudocyst
- well-circumscribed collection seen >4 weeks after onset
- well-defined inflammatory wall
- homogeneous fluid density content
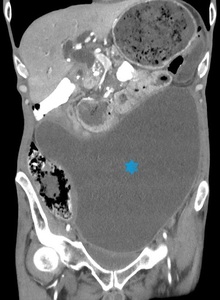
Fig. 13: Pseudocyst in a 50-year-old man with recurring pancreatitis. The fluid collection is homogeneous and presents a well-defined wall (blue star).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
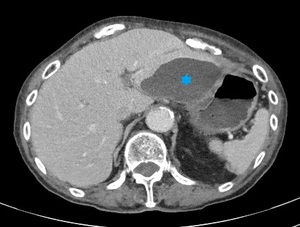
Fig. 14: Pseudocyst (blue star) in an 87-year-old woman with recurring pancreatitis.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
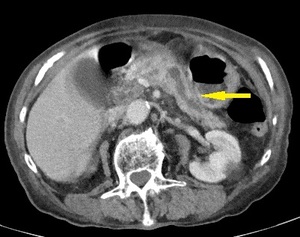
Fig. 15: Same patient as in Fig. 14. Dilatation and strictures of the main duct (yellow arrow), markers of recurring pancreatitis.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
Necrotising pancreatitis is associated with acute necrotic collections (ANCs) and walled-off necrosis (WON).
ANC
- heterogeneous collection containing both liquid and non-liquid attenuation densities (some appear homogeneous in the early phase) arising within the first 4 weeks after onset
- involving the pancreatic parenchyma and/or the peripancreatic tissues
- without a definable encapsulating wall

Fig. 6: Necrotising pancreatitis in a 37-year-old woman. Coronal contrast-enhanced CT image shows an area of nonenhancement in the neck of the pancreas (red star), normal enhancement of the head and body (yellow stars) and peripancreatic heterogeneous collection (blue arrows), a finding consistent with ANC.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016

Fig. 10: Same patient as in Fig. 7. Coronal image acquired after 2 weeks shows the progression of the parenchymal necrosis (red star) and heterogeneous collections containing both fluid and non-fluid densities (blue arrows), a finding that is consistent with ANCs.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
WON
- well-circumscribed collection seen >4 weeks after onset
- well-defined inflammatory wall
- heterogeneous liquid and non-liquid attenuation densities content
- involving the pancreatic parenchyma and/or the peripancreatic tissues
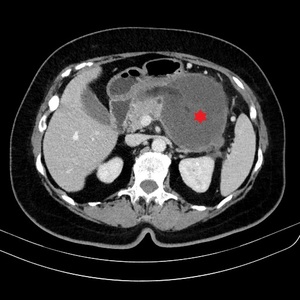
Fig. 16: WON in a 65-year-old woman with necrotising pancreatitis. Axial CECT image shows an encapsulated collection with mixed fluid and non-fluid attenuation densities (red star).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
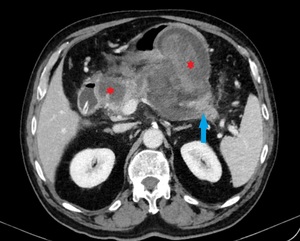
Fig. 17: WON in an 80-year-old man with pancreatic parenchyma necrosis greater than 30% (enhancing remainder highlighted by blue arrow) and several heterogeneous collections containing non-liquefied debris (red stars).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
The presence of gas within a collection indicates the presence of infection.
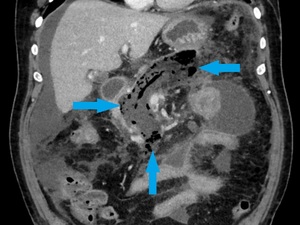
Fig. 18: Infected WON in a 63-year-old man. Coronal image shows the infected WON replacing the pancreatic parenchyma (blue arrows).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
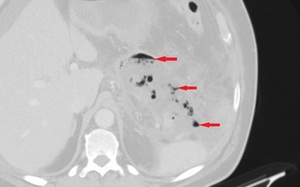
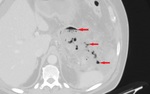
Fig. 19: Axial image of the same patient as in Fig. 18. Lung window highlights the gas bubbles (red arrows), markers of gas-producing bacteria.
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
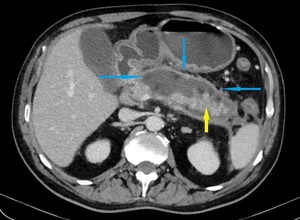
Fig. 20: Complications in a 64-year-old man with necrotising pancreatitis.
Axial CECT image shows a peripancreatic and pancreatic heterogeneous collection with fluid and non-fluid (fat spots) attenuation densities (blue arrows) and an enhancing remainder of pancreatic parenchyma (yellow arrow).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
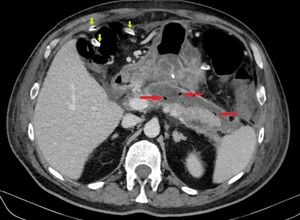
Fig. 21: Same patient as in Fig. 20, after 2 weeks. ANC infection (gas bubbles – red arrows) and percutaneous drainage catheters (green arrows).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016
Splenic artery pseudoaneurysm is another possible complication (Fig. 22).
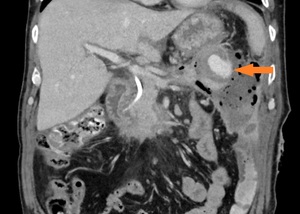
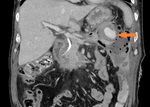
Fig. 22: Same patient as in Fig. 20, after another 5 weeks. Coronal CECT image shows a ruptured splenic pseudoaneurysm (orange arrow).
References: Department of Radiology, Regional Institute of Gastroenterology and Hepatology, Cluj-Napoca/Romania 2016