INTRODUCTION:
Scoliosis is a common problem with an incidence of 3% of the population (reviewed in 1,
2) and is important both functionally and cosmetically.
Pulmonary function may be affected in severe scoliosis.
A variety of surgical interventions are utilised and radiologists have an important role in detecting complications following surgical correction of scoliosis.
The term scoliosis was first used by Hippocrates around 4BC,
from the Greek 'σκολιοσ',
meaning ‘crooked’.
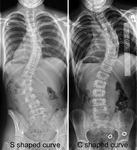
Scoliosis is defined as one or more lateral rotatory curves of the spine in the coronal plain,
resulting in an S- or C-shaped spine ( Fig. 1 ).
Although there are many causes for scoliosis (Table 1),
80% of patients have idiopathic scoliosis,
which can be subdivided depending on the age of the patient (Table 2).
Table 1: Causes of scoliosis
| Category |
Examples |
|
Mesodermal
|
Neurofibromatosis
Marfan's syndrome
Osteogenesis imperfecta
Mucopolysaccharidoses
Rheumatoid arthritis
|
|
Neuromuscular
|
Dysraphism,
myelomeningocele,
syringomyelia,
diastematomyelia,
Arnold-Chiari malformation,
tethered cord,
muscular dystrophies,
poliomyelitis,
cerebral palsy,
Friedreich's ataxia,
motor neuron disease,
spinal muscular atrophy
|
|
Skeletal dysplasias
|
Spondyloepiphyseal dysplasia
Disatrophic dwarfism
Metatropic dwarfism
Chondrodysplasia congenita
|
|
Developmental vertebral
anomalies
|
Butterfly vertebrae,
hemi-vertebrae
Wedged vertebrae
Fused vertebrae
|
|
Infection
|
Pyogenic osteomyelitis
TB,
Brucellosis
|
|
Neoplasia
|
Osteoid osteoma,
Osteoblastoma
Meningioma,
Astrocytoma,
Ependymoma
Neurofibroma
Metastases
|
|
Miscellaneous
|
Radiation,
trauma
Leg length discrepancy
Metabolic bone disease
Endrocrine bone disease
|
Table 2: Types of idiopathic scoliosis.
|
Idiopathic
|
Age
|
Sex
|
Comments
|
| Infantile |
<4 years |
Boys>girls |
90% left thoracic
Spontaneous resolution
|
|
Juvenile
|
4-9 years |
Girls>boys |
Left lumbar
Progressive
|
|
Adolescent
|
>10 years |
Girls>boys |
Right thoracic |
Painful scoliosis may be caused by osteoid osteoma,
spinal/rib osteoblastoma,
intraspinal tumour or infection.
There may also be associated congenital abnormalities such as urinary tract anomalies,
cardiac anomalies,
undescended scapula and diastematomyelia.
IMAGING SCOLIOSIS:
Imaging is important for the diagnosis and assessment of the spinal deformity,
detecting the cause of the deformity,
detecting associated developmental anomalies,
monitoring progression and determining the effectiveness of conservative and surgical interventions.
Radiographs:
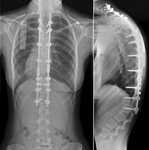
Screening for scoliosis is by a frontal radiograph.
The ACR advises a posterior-anterior (PA) radiograph from cervicocranial junction to the proximal femurs with the patient standing ( Fig. 1 ) (3).
In contrast to standard radiographs, the left side of the patient (the heart) is on the left of the radiograph as though viewing the patient from behind,
as on the surgeon's table.
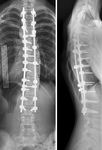
An upright lateral image may be acquired for assessment of kyphosis and spondylolisthesis ( Fig. 2 ) but should not routinely be requested with every screening PA radiograph.
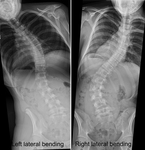
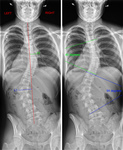
Additional lateral bending views may be acquired to determine whether the scoliosis is postural (actively correctable) or structural (rigid,
not correctible) scoliosis ( Fig. 3 ) and also for pre-operative planning.
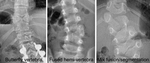
Developmental anomalies of the vertebrae may be identified on the PA radiograph as a cause of the scoliosis ( Fig. 4 ).
Failure of formation may result in wedged vertebrae,
hemi-vertebrae or butterfly vertebrae.
Failure of segmentation may result in fused vertebrae or ribs.
In many case,
there is failure of both formation and segmentation.
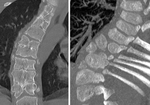
CT:
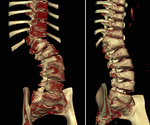
CT may aid further assessment of vertebral rotation and congenital vertebral developmental anomalies ( Fig. 5 ).
3D reconstruction tools may aid understanding of the anatomy ( Fig. 6 ).
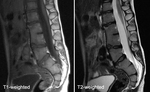
MRI:
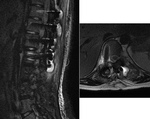
MRI may also aid characterisation of vertebral developmental anomalies ( Fig. 7 ).
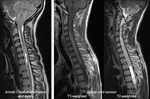
Pre-operative MRI is mandatory in patients undergoing scoliosis surgery to exclude associated spinal lesions,
such as a syrinx,
tethered cord or Chiari malformation which may complicate surgery,
and spinal tumours ( Fig. 8 ).
Bone scintigraphy:
Painful scoliosis,
which may be due to tumour or infection,
may be further investigated by bone scintigraphy.
REPORTING SCOLIOSIS RADIOGRAPHS:
Reports should include:
1.
Side of curve (right or left)
2.
Region of scoliosis (thoracic,
lumbar or thoracolumbar)
3.
Apex of the curve (most deviated from the midline)
4.
Cobb angle
5.
Developmental anomalies
6.
Risser stage
If there are two curves,
the side,
region,
apex and Cobb angle for both curves should be reported.
MEASURING COBB ANGLE
The Cobb angle is measured as the angle between a line parallel to the superior endplate of the most tilted cranial vertebra and a line parallel to the inferior endplate of the most tilted caudal vertebra ( Fig. 11 ) (4).
Scoliosis is diagnosed when the Cobb angle is greater or equal to 10o.
RISSER STAGING
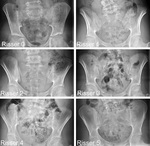
Bone maturation may be assessed by the state of ossification of the iliac crest (5,
6).
The US Risser classification defines stage 0 as no ossification of the iliac crest,
with progression from ossification of the apophyisis <25% (stage 1) to 25-50% (stage 2) to 50-75% (stage 3) to >75% (stage 4) of the iliac crest (FIG 10).
Stage 5 has complete ossification and fusion of the iliac crest apophysis .
MANAGEMENT OF SCOLIOSIS
Conservative treatments such as physiotherapy,
occupational therapy and casting/ bracing may be appropriate for mild curves of 20-40o ( Fig. 11 ).
Surgery is considered in patients with a Cobb angle of >40o,
particularly in those with progression despite bracing.
The role of surgery in idiopathic scoliosis is to prevent curve progression and to improve cosmesis,
and in neuromuscular scoliosis also to maintain balance,
reduce pain,
preserve respiratory and neurologic function and facilitate nursing care.
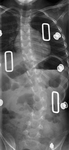
For children under 10 years of age who are still growing,
extendable rods are utilised ( Fig. 12 ).
Traditionally,
these rods were surgically extended at interval operations.
More recently,
magnetically controlled MAGEC rods have been developed that can be extended under external control as an outpatient,
without repeated surgical intervention ( Fig. 13 ).
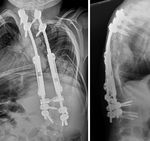
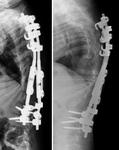
The majority of scoliosis operations involve straightening and fusing the spinal curvature using spinal implants ( Fig. 14 ) (7).
Early systems used a single Harrington rod to distract and elongate the concave curve,
but there was a relatively high revision rate due to chronic lumbar problems.
Current techniques are based around the Cotrel and Dubousset system with segmental instrumentation using pedicle screws and double rods,
resulting in better curve correction,
restoration of sagittal balance and improvement of the rotational deformity.
Post-operative imaging may be required to investigate immediate post-operative complications including pneumothorax,
haemorrhage,
fracture and metalwork mal-positioning.
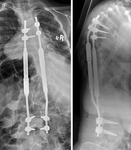
Later post-operative complications identified by imaging include metal-work failure,
pseudoarthrosis,
spinal mal-alignment and infection ( Fig. 15 , Fig. 16 , Fig. 17).