Traumatic bowel and mesenteric injuries (TBMI) are uncommon injuries with an incidence approaching 1% in recent series [1-5].
Despite this,
their clinical significance cannot be underestimated because it can be lethal if not detected and treated in a timely manner.
Clinical diagnosis is often a challenge because of the lack of specific findings in most patients and the presence of other associated lesions that may mask clinical manifestations,
in setting of loss of consciousness or head injury,
physical exam only 16% reliable in detecting abdominal injury,
making it difficult to recognize early life-threatening abdominal conditions [11].
Delays in diagnosis of only 8 hours or less are associated with increased morbidity and mortality,
predominantly related to sepsis,
bleeding or perforation [6]
Preservative management is preferred for severe splenic and hepatic trauma,
so the diagnostic challenge is to detect lesions that require surgical management such as intestinal and mesenteric trauma.
Computed tomography (CT) is superior to clinical evaluation and peritoneal lavage to diagnose important surgical lesions in the bowel and mesentery,
but the diagnostic difficulty,
even with CT,
has been widely reflected in the literature[7].
A wide of range of sensitivities and specificities have been reported for CT in diagnosing TBMI,
between 80%-95% and 48%-99%,
respectively [8-10].
Pathophysiology
TBMI are typically classified based on the mechanism of trauma.
According to this classification,
traumatic vascular injury may be caused by blunt or penetrating trauma.
TBMI in blunt trauma occurs as a consequence of three basic mechanisms: shearing injuries caused by deceleration,
crush injuries from direct impacts,
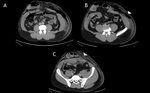
and burst injuries from sudden increases in intraluminal pressure[7] (figure 1).
At least one-half of hollow visceral injuries involve the small bowel,
with colonic,
duodenal,
and gastric injuries occurring in decreasing order of frequency.
The proximal jejunum and distal ileum are particularly susceptible to injuries from blunt traumatic forces.
The points of fixation at these two sites allow shearing forces to injure the more mobile loops.
Penetrating injuries result from projectile (gun) and non-projectile devices.
Penetrating projectiles strikes and deforms tissue and radiates out laterally,
propagating tissue damage.
The lethality of a projectile is related significantly and directly to its deformability and the degree of fragmentation it undergoes in the target (figure 2).
Non-projectile devices include knives and other sharp implements such as screwdrivers,
glass,
ice picks,
pens,
broken bottles,
coat hangers and elements that can cause stab wounds.
Practical Tips for Assessing TBMI
A number of CT signs of bowel and mesenteric trauma are recognized.
These may be classified into those that are specific to,
or indicative of,
significant bowel or mesenteric injury and less specific signs.
Unfortunately,
the imaging diagnosis of TBMI often relies on being vigilant in identifying the indirect signs as there are only a few direct signs that can be identified on CT .
For bowel injuries,
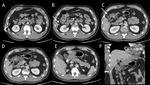
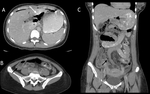
direct signs include transection of the wall with focal discontinuity (figure 3),
extraluminal oral contrast,
extraluminal gas pneumoperitoneum,
and pneumoretroperitoneum [12].
The most severe bowel injuries are seen directly on CT as frank perforations with a focal interruption in the continuity of the bowel wall,
and can be classified as bowel lacerations.
Although this sign is almost 100% specific,
its sensitivity is low,
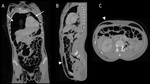
because only approximately 7% of injuries present with this finding. Indirect signs of bowel injuries are more common and include the presence of free fluid,
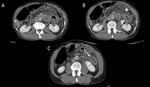
bowel wall thickening differential bowel wall enhancement and ill-defined increased attenuation (“stranding”) of the mesentery [13]. (figure 4 and 5)
Direct signs of mesenteric injuries include vascular beading,
abruptly terminated vessels and contrast extravasation.
Indirect signs of mesenteric injuries include hematoma formation (sentinel clot),
mesenteric infiltration,
and secondary changes in the accompanying bowel [6-8].
Studies that used a different generation of scanners and relied on the multiple signs detailed in this article report a sensitivity between 70% and 95% and a specificity between 92% and 100% for the diagnosis of bowel and mesenteric injuries [7,14]
Pneumoperitoneum is found on CT in 20% to 75% of patients with proven bowel perforations.
The amount of extraluminal gas varies widely and can be massive,
filling all peritoneal compartments,
or very small,
with only a few bubbles noted outside of the bowel lumen [6-8].
Pitfalls in interpretation
No visualization of pneumoperitoneum on tomography does not exclude intestinal perforation,
this can happen for several reasons: Perforation may be partially contained or sealed,
development of ileus prevents gas leakage,
small collections of air can spontaneously be reabsorbed by the peritoneal membrane.
Free intraperitoneal gas is a highly suggestive but not a pathognomonic sign of bowel perforation.
Others intra abdominal pathologies can causes of pneumoperitoneum thats include intraperitoneal rupture of the urinary bladder,
massive pneumothorax (if a diaphragmatic rupture coexists),
barotrauma,
benign pneumoperitoneum (eg,
as observed in some patients with systemic sclerosis),
and surgical procedures.
Pseudopneumoperitoneum is another potential pitfall caused by air confined between the inner layer of the abdominal wall and the parietal peritoneum,
may be found in patients who experience injuries to the extraperitoneal segments of the rectum,
rib fractures,
pneumothorax,
or pneumomediastinum,
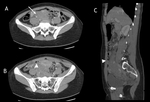
with collections of extraluminal gas accumulating between the deep layers of the abdominal wall and the parietal peritoneum [6.7]. (figure 6)